Hashimoto’s Disease – symptoms, causes, diagnosis, and treatment. Find out how to recognize and effectively manage chronic thyroid inflammation.
Table of Contents
- What is Hashimoto’s Disease? Definition and Basic Information
- Most Common Hashimoto’s Symptoms – How to Recognize Them?
- Causes of Hashimoto’s – Why Does the Immune System Attack the Thyroid?
- Diagnosis of Hashimoto’s – Laboratory Tests and Examinations
- Hashimoto’s Treatment – Pharmacological and Non-pharmacological Methods
- Living with Hashimoto’s – Recommendations and Support for Patients
What is Hashimoto’s Disease? Definition and Basic Information
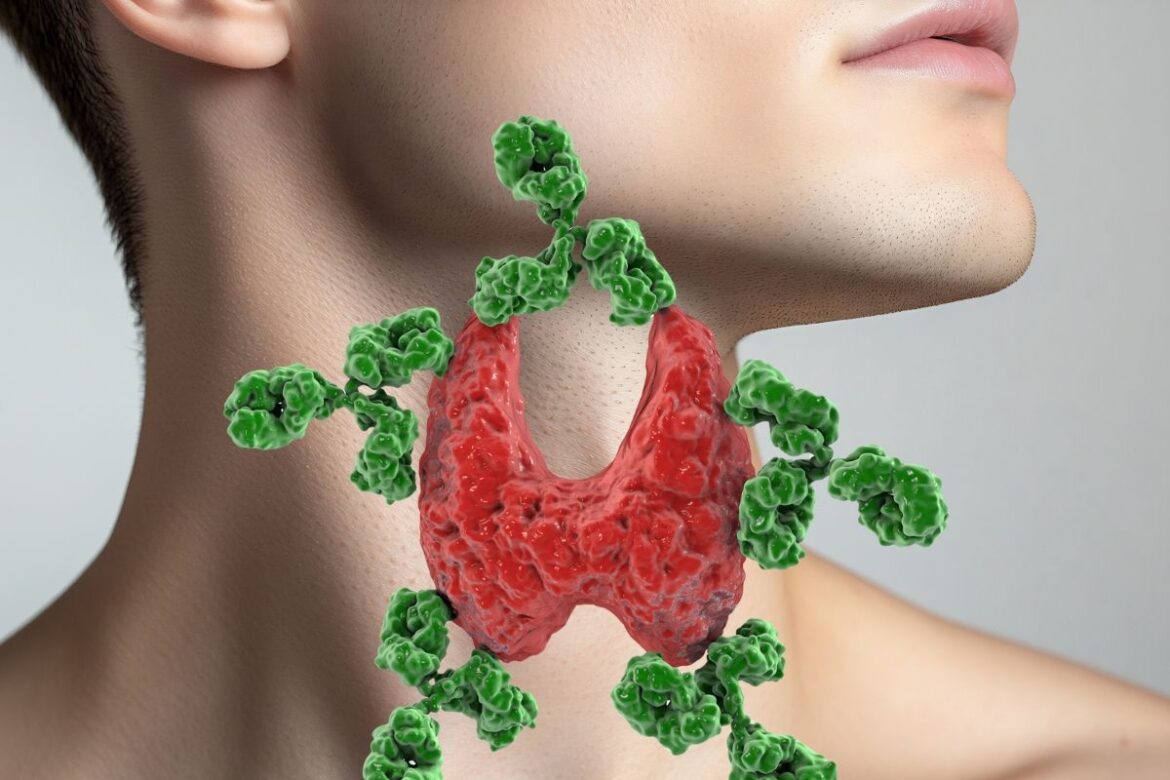
Hashimoto’s disease, also called chronic lymphocytic thyroiditis, is an autoimmune disorder in which the immune system attacks the body’s own thyroid cells. It was first described in 1912 by Japanese physician Hakaru Hashimoto, whose name the condition now bears. Hashimoto’s is currently the most common cause of hypothyroidism in developed countries, and its incidence has been growing for years. The disease develops gradually: a chronic inflammatory state within the thyroid gland progressively destroys the thyroid tissue, causing a slow decline of its hormone production. As a result, the body produces less and less thyroid hormones, which leads to a range of clinical symptoms related to underactive thyroid. Hashimoto’s primarily affects women—up to 10 times more often than men—with peak onset typically between ages 30-50, although it can occur in younger people and even children.
Chronic Hashimoto’s thyroiditis is classified as an autoimmune disease, in which the body mistakenly recognizes its own tissues as foreign and generates an immune response against them. In Hashimoto’s, autoantibodies—most frequently anti-thyroid peroxidase (anti-TPO) and anti-thyroglobulin (anti-TG)—play the main role; these can be identified in laboratory tests and are critical for diagnosis. The autoimmune process leads to progressive damage of the thyroid follicular cells, initially causing subtle dysfunctions of the gland and, with progression, to permanent hypothyroidism. Hashimoto’s often starts with no symptoms and develops slowly over years before the first clinical signs appear. For many, the first warning signs may be nonspecific symptoms such as chronic fatigue, weight gain, or dry skin, which are easily overlooked. In Poland and globally, Hashimoto’s is a serious health concern—an estimated 5% of the population may be at risk, though the actual numbers are likely higher due to undiagnosed cases. The chronic and often nonspecific course of this disease makes swift, accurate diagnosis using laboratory and imaging tests essential for preventing complications and implementing effective treatment.
Most Common Hashimoto’s Symptoms – How to Recognize Them?
Diagnosing Hashimoto’s disease is challenging due to the nonspecific and varying nature of its symptoms, which often develop gradually and may be confused with other ailments. In the early stage, symptoms are usually subtle or absent, while hypothyroidism occurs gradually. The most common symptoms include chronic fatigue and weakness that persist despite rest, sleepiness, and decreased life energy. Patients often report weight gain even without changes in diet or physical activity, which is a consequence of a slowed metabolism caused by a hormone deficiency. Feeling cold—even in warm environments—and increased sensitivity to low temperatures are also characteristic. Patients may experience dry skin, brittle nails, hair loss, and swelling—especially of the face, eyelids, and hands. Constipation, bloating, and digestive disturbances are frequent. Psychological symptoms include low mood, depression, trouble concentrating, slow thinking, and memory problems. Some people also report increased irritability, anxiety, or apathy.
Menstrual disturbances—very heavy or irregular cycles—are common among women with Hashimoto’s and can lead to difficulties becoming pregnant. Men can also experience reduced libido or fertility issues. Cardiovascular symptoms such as bradycardia (slow heart rate), increased blood pressure, or elevated cholesterol may indicate thyroid hormone disturbances. Some patients also observe neck swelling due to thyroid gland enlargement (goiter), which may cause hoarseness, trouble swallowing, or a sensation of throat tightness. The persistent autoimmune process in Hashimoto’s affects the whole body, so the symptom pattern is highly individual—not every person will have them all, and their severity may vary over time. For older adults, symptoms tend to be less obvious—sometimes limited to drowsiness and slowed physical or mental reaction—which can delay diagnosis. The broad spectrum of Hashimoto’s symptoms makes patient and doctor vigilance essential, and diagnosis should always be confirmed by proper lab and imaging studies. Noticing even mild or nonspecific symptoms early and consulting a specialist can prevent serious health consequences and considerably improve life quality.
Causes of Hashimoto’s – Why Does the Immune System Attack the Thyroid?
Hashimoto’s disease develops as a result of an erroneous immune response, where the body starts to recognize thyroid cells as a threat and launches an autoimmune process to destroy them. The mechanism results from a multifactorial interaction between genetic predisposition and environmental factors that together contribute to disease development. The genetic influence is apparent in the increased occurrence of Hashimoto’s among those with a family history of autoimmune conditions such as rheumatoid arthritis, type 1 diabetes, or celiac disease. Polymorphisms in genes responsible for immune system regulation—such as HLA-DR, CTLA-4, or PTPN22—increase the risk of an autoimmune reaction and misrecognition of thyroid antigens as “foreign.” Genes alone do not determine whether a person will develop the condition—many with the genetic predisposition never do. Environmental factors often must be present for Hashimoto’s to manifest.
The most significant environmental triggers include chronic stress, viral and bacterial infections, exposure to toxic substances (such as bisphenol A, cigarette smoke, or excessive dietary iodine), and certain medications, for example, interferon-alpha or amiodarone. Hormonal disturbances—such as during pregnancy or menopause—can trigger or exacerbate autoimmune reactions. Deficiencies in selenium and vitamin D, and disruptions in gut microbiota are also particularly important, as they promote chronic inflammation and increase gut barrier permeability, allowing antigens to enter the body and overactivate immunity. In Hashimoto’s, the immune system produces antibodies against thyroid proteins, especially peroxidase (anti-TPO) and thyroglobulin (anti-TG). This immune attack gradually destroys thyroid cells, leads to fibrosis, and finally a decrease in thyroid hormone synthesis. This process is slow, often takes years, and symptoms may not appear until considerable damage is done. There is no single clear cause of Hashimoto’s—it is most often the result of complex interactions between genetic predisposition, immune dysregulation, and environmental triggers. This variety of causes makes the disease one of the most challenging to prevent or control, and both physician and patient must take a comprehensive approach to diagnosis and treatment.
Diagnosis of Hashimoto’s – Laboratory Tests and Examinations
Diagnosis of Hashimoto’s disease combines a thorough medical history, evaluation of clinical symptoms, and laboratory and imaging tests to confirm autoimmune thyroid inflammation and assess gland function. The core and most common tests are thyroid hormone levels: thyroid-stimulating hormone (TSH), free thyroxine (fT4), and free triiodothyronine (fT3). In early Hashimoto’s, TSH may be elevated with normal fT4 and fT3 levels—a condition called subclinical hypothyroidism. As the disease progresses, fT4 and fT3 decrease while TSH rises further, indicating overt hypothyroidism. At the same time, the presence of thyroid autoantibodies—mainly anti-thyroid peroxidase (anti-TPO) and anti-thyroglobulin (anti-TG)—is crucial for diagnosis. Elevated levels of these antibodies are a strong marker of autoimmunity and one of the main Hashimoto’s diagnostic criteria. It’s worth noting that not all patients will have raised anti-TG antibodies—anti-TPO is more important diagnostically and is elevated in up to 90-95% of Hashimoto’s patients.
If the picture is unclear or another thyroid disease is suspected, imaging tests—particularly ultrasound—may be used. Ultrasound can evaluate the size, tissue structure, and reveal focal changes or goiter. The typical ultrasound pattern for Hashimoto’s is a nonhomogeneous, hypoechogenic tissue and gland enlargement, which, combined with blood test results, supports diagnosis. Sometimes, additional parameters such as TSH receptor antibodies (TRAb) are measured, particularly to differentiate from Graves’ disease. In selected cases, it is also advised to check vitamin D, selenium, ferritin, and other markers of inflammation or general health, since these disturbances are often present in Hashimoto’s and have diagnostic and therapeutic value. A comprehensive assessment of lab results, imaging, and medical history is necessary for an accurate diagnosis and effective treatment plan. Importantly, those suspected of Hashimoto’s should regularly monitor TSH and thyroid hormones, since the disease course may lead to changing thyroid function over time and require therapeutic adjustment.
Hashimoto’s Treatment – Pharmacological and Non-pharmacological Methods
The treatment of Hashimoto’s disease focuses primarily on correcting the deficiency of thyroid hormones and alleviating hypothyroidism-related symptoms. The main pharmacological approach is levothyroxine—the synthetic equivalent of thyroxine (T4)—which replaces the missing hormone and restores metabolic balance. The dosage is individually adjusted based on age, body weight, hormone test results, and the severity of hypothyroidism. Levothyroxine treatment is generally for life and requires regular monitoring of TSH, fT4, and fT3 levels to avoid under- or overtreatment. If other autoimmune diseases are present, additional treatment optimization may be necessary. In pregnant women or those planning pregnancy, special attention is paid to proper thyroid hormone levels, as deficiency may harm fetal development. In some cases—significant thyroid enlargement (goiter), airway compression, or suspected malignancy—surgical intervention is considered, though this is rare and only for clear indications. Medication does not influence autoantibody production, but it effectively controls hypothyroidism symptoms and improves quality of life. Unfortunately, there is no medication that treats the underlying autoimmune process—therapy aims to regulate hormones and address deficiencies caused by the disorder.
Non-pharmacological methods play an increasingly significant role in Hashimoto’s comprehensive treatment, including lifestyle changes, a proper diet, supplementation, and stress management. Dietary support is crucial—foods rich in fiber, vitamins, and minerals, especially selenium, zinc, and vitamin D, support thyroid function and may ease the disease course. It’s recommended to avoid processed foods, excess iodine, soy, and gluten—especially in those sensitive to these ingredients or with coexisting celiac disease—though elimination diets should be overseen by a specialist. Regular physical activity helps maintain healthy weight, improves mood, and supports metabolism—both vigorous exercise and moderate activities like walking or yoga are advised. Mental health and stress management are also very important: chronic stress can intensify autoimmunity, so relaxation techniques, meditation, psychotherapy, or peer group support are recommended. Good sleep habits are also important, as sleep disorders can disrupt hormonal regulation. In some patients, probiotic supplementation is considered to help with gut microbiota, crucial for the immune system. Monitoring and correcting iron and B vitamin deficiencies is also worthwhile, as these are more common with autoimmune diseases. Modern diagnostic tools allow for therapy individualization and adjustment of pharmacological and non-pharmacological approaches, which, in the long run, contributes to better health stabilization and reduces hypothyroidism-related complication risks.
Living with Hashimoto’s – Recommendations and Support for Patients
A Hashimoto’s diagnosis changes a patient’s everyday life and requires a broad approach to physical and mental health care. It’s crucial to establish a regular health monitoring routine—especially through thyroid hormone testing and seeing an endocrinologist at least once or twice annually, or more often if advised by a doctor. Taking the prescribed dose of levothyroxine at the same time each day (most often in the morning, on an empty stomach) is a cornerstone of medication adherence, but patients need to understand that therapeutic effectiveness also depends on diet, activity, and lifestyle habits. High-processed foods, excess sugar, and trans fats should be avoided, and instead, focus should be on wholesome grains, vegetables, fruits, healthy fats, and lean proteins. Supplementation deserves particular attention as deficiencies in selenium, vitamin D3, iron, or B vitamins can worsen the disease course. Consulting a clinical dietitian is useful, especially when facing weight reduction challenges or using elimination diets, e.g., due to gluten or lactose intolerance. Regular physical activity, such as brisk walking, swimming, yoga, or strength training adapted to one’s capacities, benefits metabolism and immunity. Besides health aspects, care for psychological stability is essential—relaxation techniques like meditation, mindfulness, diaphragmatic breathing, or regular nature contact help cope with stress, which frequently exacerbates Hashimoto’s symptoms. Family and friend support and open communication about the disease, its limitations, and patient needs help foster acceptance and gain needed help in everyday challenges.
Living with a chronic autoimmune disease like Hashimoto’s can also be challenging socially and professionally, making it vital to seek and build a support network. Psychological or therapeutic help can be crucial, especially with chronic fatigue, low mood, anxiety, or feelings of isolation. Participating in thyroid disease support groups, including online ones, makes it possible to share experiences, exchange practical tips, and find understanding from those facing similar challenges. At work, people with Hashimoto’s should inform their employer of their condition, so that their scope of duties or working hours can be adjusted if required. For women planning pregnancy, prior thorough planning and medical consultation is important, since proper disease management greatly increases the chances of a positive course for both mother and child. Many with Hashimoto’s experience fatigue and difficulties with concentration which impact daily tasks and relationships, so introducing good sleep habits, regular rest, and a clear daily plan may help prevent overwhelm. Conscious self-care, adequate support from others, regular health monitoring, and education on the disease are key to maintaining good quality of life despite the chronic nature of Hashimoto’s, which does not have to mean giving up on personal, professional, or social activity.
Summary
Hashimoto’s disease is a chronic autoimmune condition that gradually destroys the thyroid and disrupts hormonal balance. Recognizing symptoms such as weakness, weight gain, or drowsiness is crucial for swift diagnosis and appropriate treatment. Modern laboratory testing enables fast detection of Hashimoto’s and the launch of effective—pharmacologic and supportive—therapies. Adequate medical care and lifestyle changes can slow disease progression and improve comfort. Psychological support and regular health monitoring remain extremely important for Hashimoto’s long-term management.