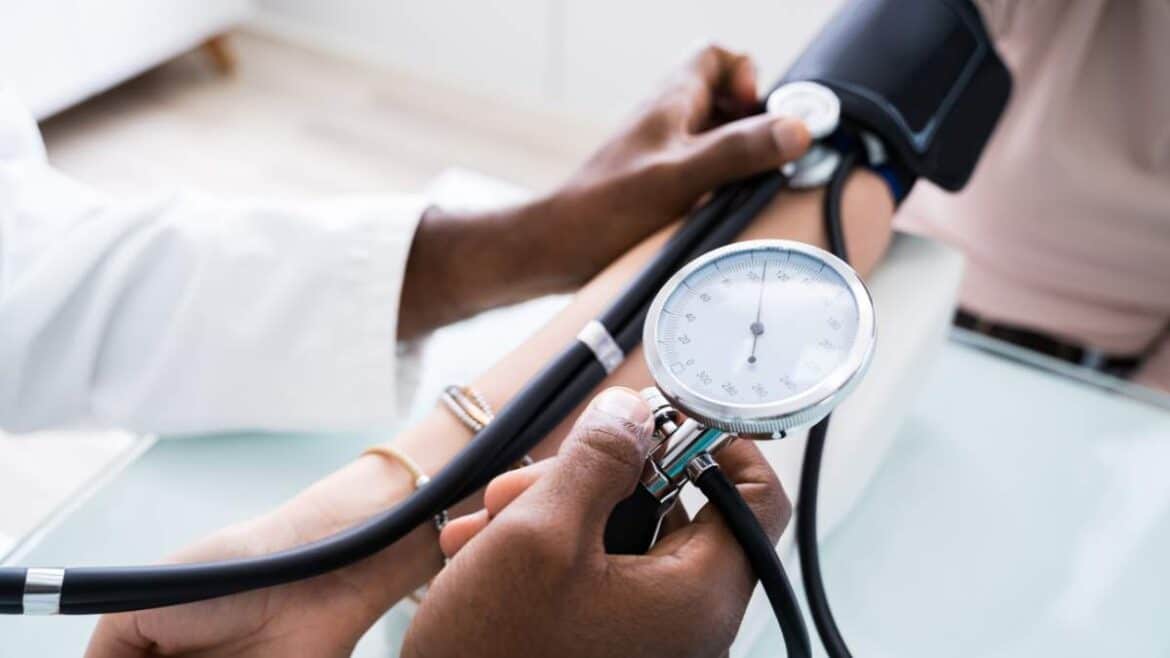
Learn why regularly measuring your blood pressure is important for heart health and prevention. Discover recommendations and practical tips.
Table of Contents
- What Is Blood Pressure and How to Measure It Correctly?
- Most Common Factors Affecting Blood Pressure Results
- Consequences of Untreated Hypertension
- Benefits of Regular Blood Pressure Monitoring
- Doctor’s Recommendations: How Often to Check Blood Pressure at Home?
- What Preventive Actions Help Maintain Healthy Blood Pressure?
What Is Blood Pressure and How to Measure It Correctly?
Blood pressure is one of the most important vital parameters, reflecting the force with which blood presses against blood vessel walls as it flows through the circulatory system. This measurement is expressed in two values: systolic pressure (upper value), showing the pressure generated when the heart pumps blood into the arteries, and diastolic pressure (lower value), indicating the pressure in the vessels when the heart relaxes between beats. Optimal adult values usually hover around 120/80 mmHg, but normal blood pressure can vary slightly depending on age, sex, health status, and even time of day. Too high blood pressure (hypertension) and too low blood pressure (hypotension) carry the risk of serious health complications such as heart disease, stroke, or internal organ damage. That’s why regular monitoring of this parameter is crucial for maintaining health and preventing cardiovascular diseases.
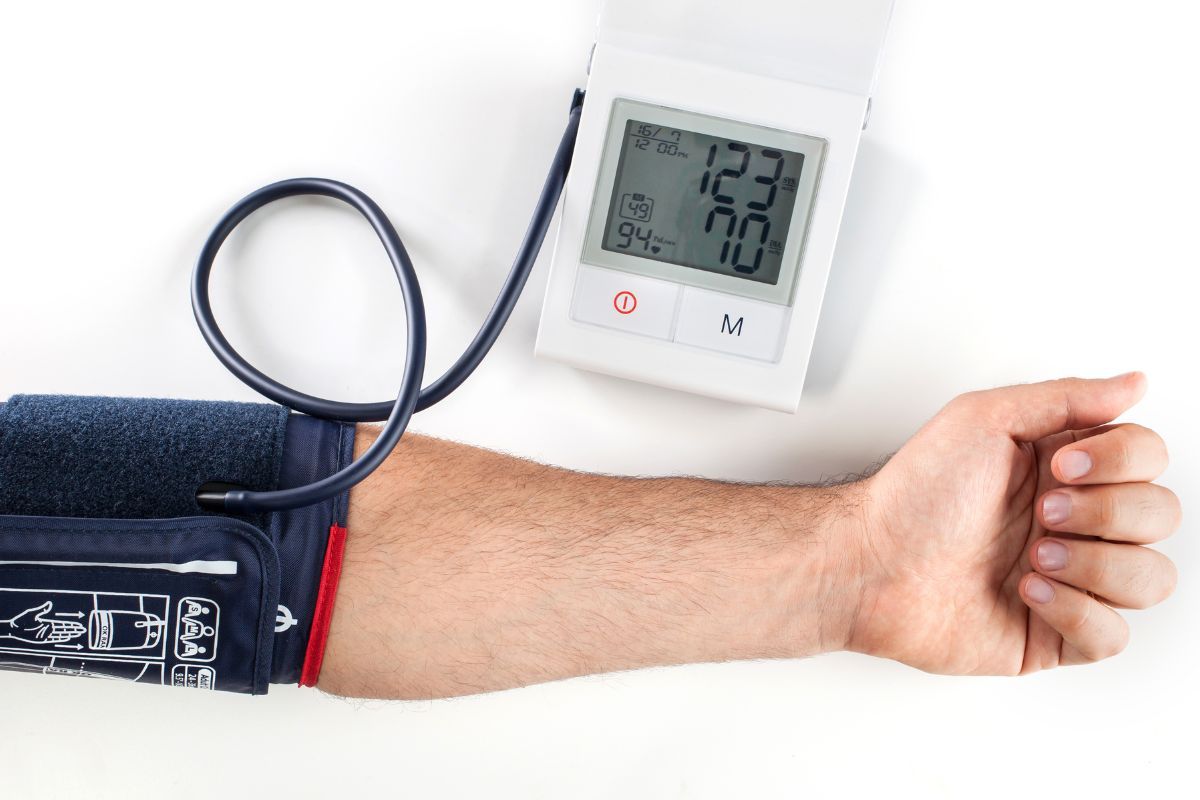
Proper blood pressure measurement requires the right technique and consideration of several important factors that significantly impact results. The most common method involves using an automatic or manual sphygmomanometer, placing the cuff above the elbow on the upper arm. While measuring, sit comfortably with your back supported, legs uncrossed, and arm resting at heart level. Before measurement, rest in a quiet room for at least 5 minutes, avoid physical exertion, coffee, smoking, and meals for at least 30 minutes beforehand, as all these can temporarily raise or lower blood pressure. Measurement should be done at the same times each day—ideally in the morning after waking and in the evening—to get a reliable picture of blood pressure throughout the day. For those suspected of hypertension or with other cardiovascular issues, doctors often recommend regular, multiple readings, keeping a diary, and consulting a specialist. Choosing the right equipment is also very important: arm-cuff monitors yield the best results, while wrist monitors should only be used if arm measurement is impossible. Using equipment correctly and following the measurement procedure minimizes errors and helps to detect abnormalities at an early stage. Regular self-measurement of blood pressure at home allows the creation of a detailed blood pressure profile and helps detect even slight deviations that might be missed during a single, occasional doctor’s visit.
Most Common Factors Affecting Blood Pressure Results
Blood pressure readings can vary widely, even in the same person, depending on numerous external and internal factors that significantly affect their reliability. The first basic aspect is the emotional state—stress, anxiety, nervousness, or even brief discomfort can cause significant, often transient, increases in blood pressure. Thus, a short period of relaxation before the test, as well as a calm and quiet environment, are key. Physical activity right before the measurement is also important—even minor exertion such as walking up stairs or lifting heavy objects can temporarily raise both systolic and diastolic values. Diet matters as well: consuming coffee or other caffeinated drinks, smoking, or eating a heavy meal shortly before the measurement may lead to elevated readings. Alcohol, even in small amounts before the test, has a similar effect to caffeine—it stimulates the circulatory system and interferes with accurate results. Dehydration, especially common among the elderly or on hot days, can artificially lower readings, which can be misleading when interpreting home measurements. Regular use of blood pressure medication or other chronic condition drugs, as well as supplements or herbal preparations (prescribed or not), often greatly affects blood pressure values, highlighting the importance of keeping a medication diary alongside blood pressure records.
Technical and procedural factors are also a frequent source of measurement errors. The right cuff size matters a lot—too narrow or too wide a cuff can significantly distort results. The correct body position during measurement is equally important: the arm should be supported at heart level, feet flat on the floor, and back resting against the chair. Ignoring these guidelines leads to inaccurate readings. Speaking or moving during the measurement disrupts the result, so the person being tested should remain still and silent throughout. Ambient temperature also plays a role—cold can cause blood vessel constriction and raise pressure, while excessive heat favors a decrease. Poorly calibrated or outdated, unserviced devices are another source of errors in home measurements. Regular monitor maintenance and using certified devices eliminates potential equipment errors. The individual’s health conditions, such as infections, fever, severe pain, and chronic diseases like diabetes, atherosclerosis, or kidney failure, can also cause blood pressure fluctuations regardless of lifestyle. The body’s daily rhythm and natural hormonal fluctuations during the day (for example, higher blood pressure in the morning, lower in the evening) directly affect one-time results. For a reliable diagnosis of blood pressure disorders, pay attention to measurement consistency and conditions, minimizing or eliminating the interfering factors mentioned above.
Consequences of Untreated Hypertension
Untreated hypertension is a serious health issue that can have extremely dangerous consequences for both the heart and the entire body. Persistently high blood pressure causes irreversible damage to blood vessels, leading to accelerated atherosclerosis, with arteries hardening and narrowing. These changes facilitate cholesterol deposits and increase the risk of coronary artery disease, which can result in a heart attack. Hypertension also increases the workload on the heart muscle, requiring the heart to work harder to pump blood through the vascular system. Over time, this strain leads to left ventricular hypertrophy and heart failure—a disorder that significantly reduces quality of life and may be directly life-threatening. High blood pressure is also a main risk factor for stroke. Extremely elevated values can cause weakened brain vessels to rupture and consequently result in bleeding into the brain, leading to permanent neurological disorders, disability, or even death. Untreated hypertension negatively affects the kidneys, damaging their delicate filtration structures. Excessive blood pressure disrupts proper blood flow through the kidneys, resulting in chronic kidney disease, and eventually, kidney failure requiring dialysis or a transplant.
The consequences of untreated hypertension are not limited to the cardiovascular system or kidneys. Pathological changes affect virtually all organs, including the eyes—hypertensive retinopathy can gradually diminish vision or even result in permanent blindness. Persistently high blood pressure also impairs brain function, leading to so-called hypertensive encephalopathy, impairing cognition, memory, concentration, or orientation. In the elderly, hypertension can contribute to vascular dementia. High blood pressure accelerates vascular aging, making arteries more prone to aneurysms, ruptures, or dissections. Uncontrolled hypertension can also trigger metabolic diseases, such as type 2 diabetes, by disrupting carbohydrate, lipid, and hormone regulation. It is often responsible for chronic headaches, fatigue, breathlessness, or sleep disorders, which increasingly worsen and reduce quality of life over time. Unfortunately, in many cases, hypertension develops silently over years, so its effects are usually detected only when complications occur. All the more reason to regularly monitor blood pressure to avoid the silent but extremely dangerous consequences of untreated hypertension, directly threatening health and life and potentially leading to permanent disability.
Benefits of Regular Blood Pressure Monitoring
Regular blood pressure monitoring offers numerous tangible health benefits—both for early detection of abnormalities and effective management of existing cardiovascular conditions. The most essential benefit is the ability to quickly identify increased or decreased blood pressure, which often remains asymptomatic for a long time. By measuring regularly, even subtle value changes can be detected, which from a medical perspective may signal the onset of diseases requiring prompt intervention. This is especially crucial for at-risk populations such as the elderly, people with obesity, diabetes, kidney disease, or a family history of hypertension, and for pregnant women, in whom blood pressure disorders pose risks for both mother and child. Monitoring blood pressure at home enables a fast response to abnormalities, preliminary diagnosis, and provides the doctor with more complete data for further analysis—even transient rises or drops, which could be missed at a doctor’s visit, are recorded and considered in health assessment.
Another key advantage is support for effective prevention and precise therapy management for diagnosed hypertension or other blood pressure disorders. Systematic self-monitoring motivates a healthy lifestyle, as it allows the patient to see how specific habits affect their readings—a high-sodium diet, excess alcohol, inactivity, or stress can be immediately related to blood pressure results, which encourages lifestyle change and faster positive outcomes. Regular measurement and record-keeping increase health awareness, educate about risk factors, and encourage seeking medical advice for worrying trends. It is an invaluable tool in cooperation with your doctor: reliable, systematic data enable medication adjustments, assessment of current therapy effectiveness, and faster identification of side effects or the need for modification. Home monitoring also eliminates the so-called “white coat effect,” i.e., artificial blood pressure elevation during a medical visit due to stress, allowing a more realistic view of everyday levels. Therefore, regular measurement means not only better hypertension control, but also prevention of complications such as stroke, heart attack, heart and kidney failure, and a significant increase in overall life quality through assurance and control over one’s health. By detecting irregularities early, raising health awareness, and enhancing cooperation with the medical team, regular blood pressure monitoring becomes a fundamental tool in cardiovascular prevention and the active maintenance of good health.
Doctor’s Recommendations: How Often to Check Blood Pressure at Home?
Cardiology experts and doctors have long emphasized that regular home blood pressure monitoring has become an increasingly important element of health prevention. Recommendations for measurement frequency are individualized and depend mainly on age, the presence of risk factors, ongoing therapies, and patient health history. For healthy adults without diagnosed hypertension or other chronic diseases, most scientific societies—including the Polish Cardiac Society and the European Society of Hypertension—recommend blood pressure measurement at least every few months, ideally every three to six months. This allows for the rapid detection of unexpected changes and early intervention. The situation changes dramatically for at-risk groups, including the elderly (usually over 60), patients with diagnosed hypertension, heart disease, chronic kidney disease, diabetes, or pregnant women. For these individuals, more frequent monitoring is recommended—at minimum once a week, and often daily, especially when initiating new drug therapy or adjusting medication doses. Doctors recommend that in case of health changes (e.g. symptoms like dizziness, headaches, worsening wellbeing, or limb swelling), additional measurements should be taken regardless of set routines. Blood pressure control should also be more intensive following events like stroke, heart attack, or with coexisting chronic ailments—regular readings allow rapid detection of worrying trends and fast modification of therapy by the attending physician.
Guidelines for home measurement are based on consistency and repeatability to obtain the most reliable health picture. Experts point out that measurements should always be performed at the same time of day—preferably in the morning upon waking and in the evening, before meals or medications, after several minutes of rest. In the early phase of hypertension diagnosis (for example, following European Society of Hypertension guidelines), measurements should be performed for at least 3–7 consecutive days (ideally two in the morning, two in the evening), with the results carefully recorded in a personal health diary. This allows the doctor to more accurately assess blood pressure dynamics and spot the “white coat effect”—falsely elevated values occurring only in the doctor’s office. This is also important when changing medications—during the first weeks of new or adjusted therapy, measurements should be performed daily, then, according to physician guidance, gradually reduced to several times a week or less. Especially for patients with unstable pressure or multiple comorbidities, closely monitoring the body for worrying symptoms and reporting them with the measured values enables a fast medical response. Regardless of frequency, reliability can be improved by following the previous section guidelines: staying calm, correct body positioning, regularity, and diligent record-keeping. It should be emphasized that self-monitoring at home serves not only for early diagnosis and tracking treatment effectiveness but also encourages greater responsibility and engagement in one’s own health care. Implementing these recommendations leads to increased safety and prevention effectiveness for cardiovascular diseases, allowing quick reactions to abnormal trends or values.
What Preventive Actions Help Maintain Healthy Blood Pressure?
Maintaining normal blood pressure requires a broad range of preventive actions encompassing both lifestyle and proper medical monitoring. The key element is physical activity—regular aerobics such as brisk walking, swimming, cycling, or dancing significantly improve vessel elasticity and contribute to long-term blood pressure reduction. The World Health Organization recommends at least 150 minutes of moderate activity per week, which not only stabilizes blood pressure but also helps maintain a healthy weight, reducing the risk of obesity—a major cause of hypertension. Diet is another pillar of prevention; the Mediterranean and DASH (Dietary Approaches to Stop Hypertension) diets are scientifically proven to lower blood pressure. They focus on limiting sodium (table salt), increasing intake of potassium, magnesium, calcium, fiber, and antioxidants found in fresh fruits and vegetables, whole grains, fish, nuts, and healthy plant oils. It is recommended to limit saturated fats—mainly from meat and highly-processed foods—and to avoid fast food, convenience products, and foods high in preservatives and artificial additives. Alcohol consumption should be strongly minimized—even moderate drinking may increase blood pressure. Studies also show that wholesome sleep (at least 7–8 hours per day), regular rest, and effective stress management reduce hypertension risk. Relaxation techniques like meditation, yoga, breathing exercises, or tai chi positively influence the nervous system, mitigating the harmful effects of chronic stress and stabilizing blood pressure values.
Regular medical check-ups and monitoring metabolic parameters such as cholesterol and blood glucose are also crucial, since advanced atherosclerosis and diabetes are strongly linked with blood pressure dysregulation. People in high-risk groups (e.g. family history, overweight, chronic kidney or heart disease) should monitor their health more closely and undergo periodic reviews. Eliminating stimulants like cigarettes or e-cigarettes is fundamental—tobacco causes vessel constriction and endothelial damage, resulting in higher blood pressure. Environmental factors such as excessive noise, air pollution, and a sedentary lifestyle (e.g. office work) also affect daily blood pressure values. Where possible, more time should be spent outdoors and breaks should be taken during prolonged sitting. Good practices include effective time management, establishing routines, regular breaks, maintaining hydration (at least 1.5–2 liters of fluids daily, preferably water). Dietary supplements—following medical consultation—such as magnesium or omega-3 fatty acids, can also support cardiovascular function. Responsible prevention also includes health education—updating knowledge of risk factors, hypertension symptoms, and continuously building healthy habits at the family and community level. It is crucial to tailor preventive actions to age, sex, lifestyle, and health burden for effective, long-term maintenance of proper blood pressure and significantly improving overall health.
Summary
Regular blood pressure measurement is a simple yet extremely effective tool for taking care of cardiovascular health. Monitoring blood pressure enables early detection of hypertension and implementation of preventive actions. Following doctor’s recommendations on measurement frequency and closely observing bodily changes help reduce the risk of serious health complications such as heart attack or stroke. By maintaining proper blood pressure, we gain control over our own health and increase our chance for a longer, more active life.