Discover the causes, symptoms, diagnosis, and treatment of aneurysms. Find out what to watch out for and how to effectively protect your health. Read expert advice!
Table of Contents
- What is an aneurysm? Definition and basic types
- Causes of aneurysm formation – main risk factors
- Aneurysm symptoms – what to look out for?
- Aneurysm diagnostics – how to detect the problem early?
- The most effective methods of aneurysm treatment
- Aneurysm complications and prevention – how to protect your health?
What is an aneurysm? Definition and basic types
An aneurysm (lat. aneurysma) is a local, pathological dilation of the wall of a blood vessel, most often an artery, occurring as a result of weakening of its structure. Simply put, an aneurysm can be compared to a balloon that gradually enlarges under pressure, losing its natural strength and elasticity. This process most often takes place in places where the vessel wall has been damaged or weakened, for example as a result of cardiovascular diseases, chronic arterial hypertension, atherosclerotic changes, infections, or congenital defects. Aneurysms can develop asymptomatically for years, remaining undetected until reaching a large size or rupturing, which constitutes a serious and direct life threat. There are different types of aneurysms depending on their location, shape, and etiology. The most common are aortic aneurysms, mainly of the abdominal aorta (abdominal aortic aneurysm – AAA) and thoracic aorta, but cerebral vessel aneurysms, known as intracranial aneurysms, are also frequently observed. Peripheral arterial aneurysms such as those of the femoral, popliteal, or splenic arteries, are also not uncommon.
The characterization of aneurysms is based not only on their location but also their structure and morphology. True aneurysms involve all layers of the vessel wall (intima, media, and adventitia) and usually take a saccular or fusiform form. Saccular aneurysms resemble a small balloon, are round, and have a distinct neck, typical especially of cerebral vessels. Fusiform aneurysms, on the other hand, are characterized by an even dilation along a longer segment of the vessel, most commonly seen in the aorta. Pseudoaneurysms are a separate group formed by rupture through all layers of the vessel wall; blood leaks outside the vessel, forming a hematoma that surrounds the damaged site and connects with the vessel lumen—common after trauma or vascular interventions. Another type is dissecting aneurysms, where the arterial wall layers are split apart by blood flow, creating two channels—this is particularly serious in the aorta and can lead to rapid death if rupture occurs. Aneurysms are also classified by size—from small changes measuring only a few millimeters (especially in cerebral vessels) to giant pathologies reaching several centimeters (mainly in the abdominal aorta). It’s worth stressing that aneurysms are called “silent killers”—they often remain unnoticed until dangerous complications such as rupture or embolism develop, causing massive hemorrhage, ischemia, or a stroke. Rapid diagnosis and knowledge of aneurysm types and associated risks allow effective monitoring and early treatment that can save lives. Understanding the basic definition of an aneurysm and its various forms is essential not only for physicians but also for anyone who wants to actively care for their health and recognize warning signs from their body.
Causes of aneurysm formation – main risk factors
Aneurysms emerge as a result of a multifactorial process, influenced by both genetic predispositions and acquired environmental factors and lifestyle choices. The key mechanism initiating aneurysm formation is the weakening of the blood vessel wall structure, which most often leads to its gradual stretching and the creation of a pathological bulge. The main risk factors for aneurysm development include atherosclerosis, responsible for nearly 80% of abdominal aortic aneurysm cases. Narrowing of the arteries due to cholesterol deposits leads to degenerative changes in the vessel wall’s middle layer and loss of elasticity, predisposing to bulges and weakening. Arterial hypertension exacerbates these processes by exerting additional pressure on vessel walls, potentially resulting in their gradual dilation and aneurysm formation. Smoking is another significant risk factor—toxins in cigarette smoke damage endothelial cells, accelerate atherogenesis, and degrade collagen and elastin fibers in the arterial wall, substantially increasing the probability of aneurysm formation. Another risk element is age—the risk of developing aneurysms rises significantly after age 60 due to vessel aging and progressive loss of elasticity. Genetic factors are also important—studies show that those with a family history of aneurysms have a higher predisposition to develop them, and some genetic mutations can directly affect vessel wall structure, especially in connective tissue disorders such as Marfan or Ehlers-Danlos syndromes. Injuries and past infections play a role too—in pseudoaneurysms or after bacterial infections of vessel walls (e.g., mycotic aneurysms), direct vessel damage encourages abnormality formation. Gender also matters—aneurysms are more often diagnosed in men, likely due to differences in vessel structure and greater exposure to risk factors like smoking and frequent hypertension.
Other environmental and health factors also impact aneurysm development risk. Chronic inflammatory diseases such as vasculitis or rheumatoid arthritis can cause continuous vessel wall damage, initiating degenerative processes leading to aneurysms, especially in genetically susceptible or immunocompromised people. Long-term use of steroid medications and certain immunosuppressive drugs can deteriorate collagen fiber health. Sensitivity to oxidative stress and metabolic factors, such as elevated homocysteine, are also listed as contributors to arterial structural changes. Additional risk factors include overweight and obesity—especially central obesity—which places more stress on the circulatory system and promotes development of hypertension and type 2 diabetes, both significantly speeding up vessel deterioration. Those with improper diets—lacking antioxidants and rich in trans and saturated fats—should pay special attention to cardiovascular health, as diet strongly influences the rate of atherosclerosis development. Also, lack of physical activity, chronic stress, and poor control of chronic conditions increase the risk of both developing and accelerating existing aneurysms. For specific patient groups, like those post-cardiac surgery or endovascular procedures, pseudoaneurysms can also arise due to iatrogenic complications. Many of these factors can be minimized with proper prevention, early diagnosis, and lifestyle awareness, which is crucial in preventing dangerous aneurysm-related complications. Cancer, chronic kidney failure, and other systemic diseases weakening vessel walls are also noteworthy risk factors for aneurysm formation in both the aorta and peripheral or cerebral vessels.
Aneurysm symptoms – what to look out for?
Many types of aneurysms can develop for a long time with no symptoms at all, and the first signs usually appear only when the bulge significantly increases in size or, most dangerously, ruptures. This insidious progression makes early aneurysm detection extremely difficult and often accidental—discovered during routine imaging for other reasons. Aneurysm symptoms are closely tied to location and size: an abdominal aortic aneurysm often doesn’t cause symptoms for a long time, but if large, may result in a feeling of pulsation or a pulsating mass in the abdomen, abdominal pain radiating to the back, pressure sensations, nausea, or digestive disturbances. Upon rupture, there may be sudden, tearing abdominal or lower back pain, often accompanied by a rapid drop in blood pressure, pale skin, tachycardia, and loss of consciousness. Thoracic aortic aneurysms can also progress silently—if they enlarge, symptoms may include shortness of breath, chest pain, hoarseness (from pressure on the recurrent laryngeal nerve), cough, difficulty swallowing, or symptoms from compression of neighboring organs, including fainting. Sudden rupture of a thoracic aneurysm is marked by intense chest pain, pressure drop, central cyanosis, and shock—life-threatening situations requiring immediate attention.
Cerebral vessel aneurysms (intracranial aneurysms) are a unique group due to dramatic complications—rupture causes so-called subarachnoid hemorrhage, which presents as sudden, very severe headache (“thunderclap headache”), loss or disturbance of consciousness, neck stiffness, nausea, vomiting, photophobia, and neurological symptoms like limb paralysis, speech or vision changes. Before rupturing, some brain aneurysm patients experience warning symptoms: mild headaches, double vision, drooping eyelid, balance problems, or facial numbness—these are usually non-specific and hard to interpret. In peripheral aneurysms (e.g., femoral, popliteal), a pulsating, subcutaneous mass in the lower limb area can often be detected, as well as pain, swelling, or paresthesias due to pressure on surrounding nerves. General symptoms like chronic fatigue, weakness, or weight loss tend to appear in advanced stages or following complications. Notably, sometimes the first and only sign of an aneurysm is an acute event from rupture. That’s why individuals at high risk, especially with cardiovascular disorders, should attend regular preventive check-ups and not ignore unusual ailments—particularly those involving a sudden change in pain type, appearance of a pulsating lump, or neurological symptoms. Early detection allows effective treatment and avoidance of fatal complications from a ruptured aneurysm—so vigilance for seemingly minor symptoms can save lives.
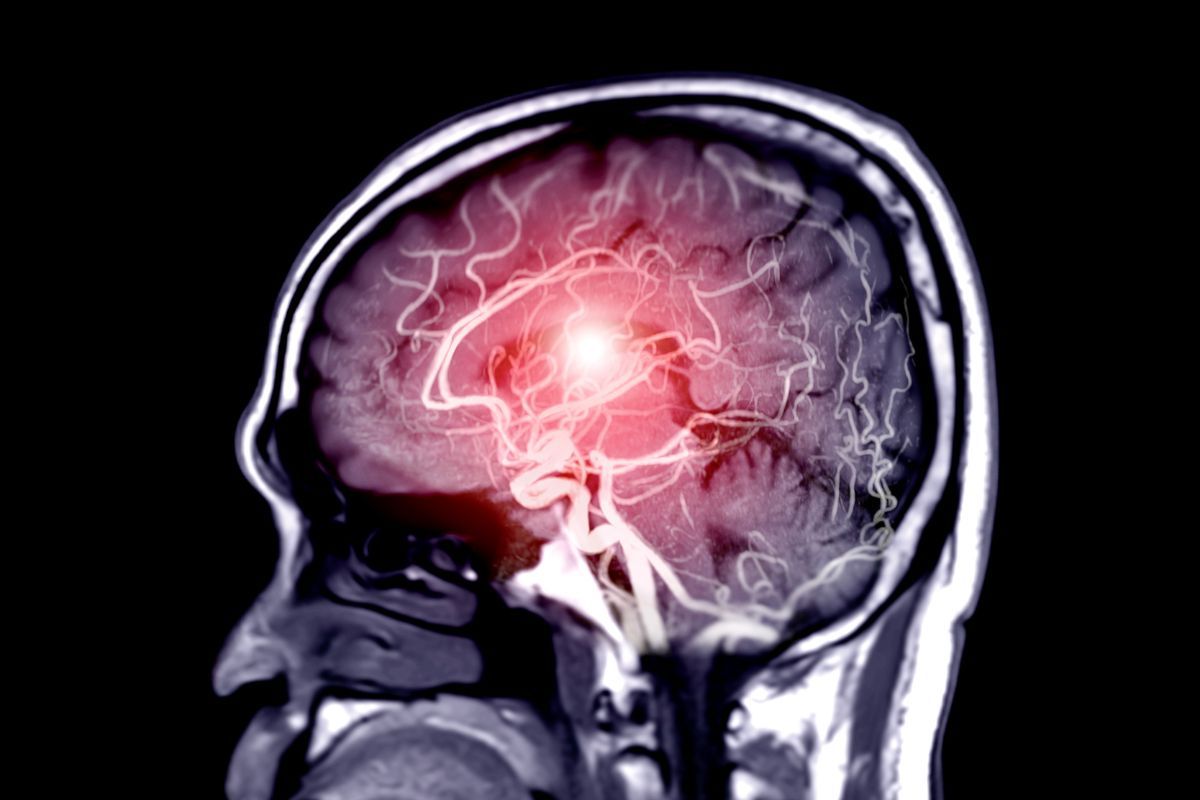
Aneurysm diagnostics – how to detect the problem early?
Aneurysm diagnostics are a crucial part of vascular disease prevention and a chance for effective treatment before serious health complications develop. Early detection of aneurysms is usually accidental during routine imaging, since this disease is often asymptomatic for a long period—hence the importance of both standard screening tests and conscious risk factor monitoring by both doctor and patient. The first diagnostic step is a thorough medical interview, where the doctor assesses general health status, any family history of aneurysms, and other diseases predisposing to its development. Physical examination may in some cases reveal an aneurysm, especially in the abdomen—palpation can detect a pulsating mass. However, in most people, especially those with deeply located or cerebral aneurysms, this examination is insufficient. At this stage, imaging tests are crucial, including ultrasonography (USG), computed tomography (CT), magnetic resonance imaging (MRI), and angiography. USG is the first-choice method for detecting abdominal aortic aneurysms due to its non-invasiveness, availability, and high sensitivity for even small changes. CT and MRI are mainly used for thoracic aortic and cerebral aneurysms, allowing precise determination of size, location, and spatial relationships relative to adjacent organs and vessels. Such diagnostics also allow assessment of rupture risk and treatment planning, directly impacting patient safety.
For suspected cerebral aneurysms, specialists primarily use angio-CT or angio-MRI—advanced imaging with contrast that allows visualization of even small vascular changes in the brain. High diagnostic value is also provided by classic angiography, involving contrast injection into the artery with a series of X-ray images—mainly used in complex cases and before surgery. Increasingly, non-invasive modern solutions like 3D CT scanning are used, allowing highly accurate realization of aneurysm size and shape. Clinically, it is also important to monitor known aneurysms for changes in size and rupture risk—so intervention can be planned in time. For certain high-risk groups, like genetically predisposed individuals or those with known atherosclerosis, periodic imaging checks are recommended even in the absence of symptoms. Modern aneurysm diagnostics depend on close collaboration between radiologists, neurologists, vascular surgeons, and internists, who base further action on test results. It’s important to stress that most aneurysms detected in the asymptomatic phase provide a real chance to implement treatment preventing complications. Medical technology has enabled screening programs, like abdominal aortic USG for those over age 65, greatly reducing the risk of sudden, uncontrolled aneurysm rupture. Effective diagnostics therefore include not just precise exams but also patient education and regular monitoring of those particularly at risk for aneurysms, crucial for prevention and reducing severe complication numbers in this vascular disease.
The most effective methods of aneurysm treatment
Treating aneurysms is a complex process requiring an individualized approach tailored to the aneurysm’s location, size, type, and the patient’s health status. The aim is to prevent aneurysm rupture and life-threatening complications such as internal bleeding or stroke. Modern medicine offers a range of advanced treatment methods for aneurysms—both via surgical operations and minimally invasive endovascular techniques, chosen depending on individual indications. The most important selection criteria are aneurysm size and location, and risk of rupture. Small, stable aneurysms with no tendency to enlarge can be monitored—regular imaging checks assess change dynamics and enable timely intervention if needed (so-called active surveillance). For aneurysms exceeding specific sizes (e.g., abdominal aortic aneurysm over 5.5 cm in men and 5.0 cm in women) or those that enlarge rapidly, interventional treatment is indicated. Symptoms presence also plays a key role—if the aneurysm causes pain, pressure on adjacent structures, or neurological symptoms, intervention becomes more urgent. The patient’s general health, age, comorbidities, and anesthesia tolerance influence treatment method choice, with the process managed by an interdisciplinary team—vascular surgeons, interventional radiologists, neurologists, and anesthesiologists.
The main methods for treating aneurysms are traditional surgical repair and modern endovascular techniques. Open surgical repair, mainly used for large or complex aortic aneurysms, involves opening the abdominal or chest cavity, exposing the diseased vessel, removing the abnormal segment, and grafting a synthetic vascular prosthesis (graft) to replace the damaged section. Open surgery is key for aneurysms in dangerous locations or those that have ruptured, when quick action and complete control are necessary. This method, however, carries risk of perioperative complications and requires longer hospitalization and rehabilitation. A less invasive alternative is endovascular methods—the implantation of stent-grafts (special internal prostheses) inside the vessel percutaneously, typically via femoral artery puncture. For aortic aneurysms (EVAR – Endovascular Aneurysm Repair) or thoracic aortic aneurysms (TEVAR – Thoracic Endovascular Aneurysm Repair), a stent system covered with special material is inserted under radiologic control, reinforcing the vessel wall and excluding the aneurysm from circulation. This treatment shortens hospital stay, allows quicker recovery, and reduces complications associated with open surgery. Endovascular approaches are now standard especially in older patients and those with comorbidities. Modern treatment of cerebral aneurysms also uses endovascular techniques such as microcoil embolization (coiling), in which platinum microcoils are delivered inside the aneurysm through a catheter, causing closure and preventing hemorrhage. Flow-diverting stents are also used, lowering blood flow into the aneurysm and promoting healing. In some cases, traditional neurosurgery with aneurysm clipping is required, placing a clip at the aneurysm base to stop blood flow. Recent years have also seen the development of hybrid methods and pharmacological innovations aimed at vessel wall stabilization and inflammation reduction. In every case, managing comorbidities such as hypertension, hyperlipidemia, and diabetes, and lifestyle changes—quitting smoking, avoiding stress, eating healthily—are essential. Early diagnosis and proper selection of treatment methods are key to improving survival and quality of life for aneurysm patients.
Aneurysm complications and prevention – how to protect your health?
An aneurysm is a silent but very serious health problem, mainly due to the risk of dangerous complications that largely determine this disease’s fatality. The most dramatic complication is aneurysm rupture, often leading to internal bleeding—in the case of abdominal or thoracic aortic aneurysm, this is a life-threatening emergency requiring immediate surgical intervention. Such bleeding quickly results in hemorrhagic shock, organ failure, and brain hypoxia, and mortality in these cases can top 80%. Cerebral aneurysm rupture, on the other hand, risks subarachnoid hemorrhage and serious neurological dysfunction, paralysis, coma, or even sudden death. Besides rupture, other complications include embolism (clot fragment blocks an artery), which can cause organ infarction, such as kidney, bowel, or brain stroke. Another danger is arterial dissection, disturbing blood flow and leading to tissue ischemia, often causing pain, necrosis, or death in a short period. Chronic complications include aneurysm infections and chronic organ ischemia, resulting in organ dysfunction. Expanding aneurysms may compress adjacent structures, causing obstructions of the digestive or urinary tracts. Complication risk depends on location, size, growth rate, and comorbidities such as atherosclerosis or hypertension.
Aneurysm prevention should be a priority not only for those with risk factors but for the wider population, since many aneurysms develop silently. Key elements of prevention are regular health checks—especially blood pressure and lipid panel monitoring—weight reduction, and quitting smoking, which greatly increases vessel wall vulnerability. Physical activity, tailored to the individual, preserves vessel elasticity, supports proper circulation, and lowers blood pressure and cholesterol levels. A diet rich in vegetables, fruit, whole grains, and omega-3 fatty acids reduces inflammation, lowers body weight, and atherosclerosis risk. Salt, trans fat, and saturated fat intake should be limited, as they foster vessel hardening. People with a family history of vascular disease should undergo early diagnostic programs—abdominal aorta USG and angio-CT scanning. If symptoms arise, such as sudden severe pain, neurological disturbance, fainting, or unusual gastrointestinal complaints, see a doctor immediately. Prevention also includes treating hypertension, diabetes, hypercholesterolemia, and regular medical evaluation to detect changes and implement therapy before complications arise. Health education regarding risk factors, promoting a healthy lifestyle, and screening for those with a family history are key to reducing complication rates and improving detection opportunities for early-stage aneurysms. With modern diagnostic tools and attention to prevention, more aneurysms are detected early enough to prevent tragic complications and significantly improve patient prognosis.
Summary
Aneurysms are a serious health issue that may remain asymptomatic for a long time, with potentially life-threatening complications. Early diagnosis and knowledge of warning symptoms such as severe headache, visual disturbances, or sudden loss of consciousness are crucial. Modern medicine offers effective treatment and prevention options, minimizing rupture risk and associated complications. Remember to monitor your health regularly, take care of cardiovascular disease prevention, and never ignore alarming symptoms.


