Coronary artery disease – discover the most important causes, symptoms, methods of diagnosis as well as effective treatment and prevention strategies. Find out how to take care of your heart!
Table of Contents
- What is coronary artery disease? Definition and basics
- Main causes of coronary artery disease development
- Symptoms of coronary artery disease – how to recognize them?
- Diagnosis of coronary artery disease: tests and process
- Effective treatment of coronary artery disease: pharmacotherapy, procedures, and lifestyle changes
- Prevention and prophylaxis of coronary artery disease
What is coronary artery disease? Definition and basics
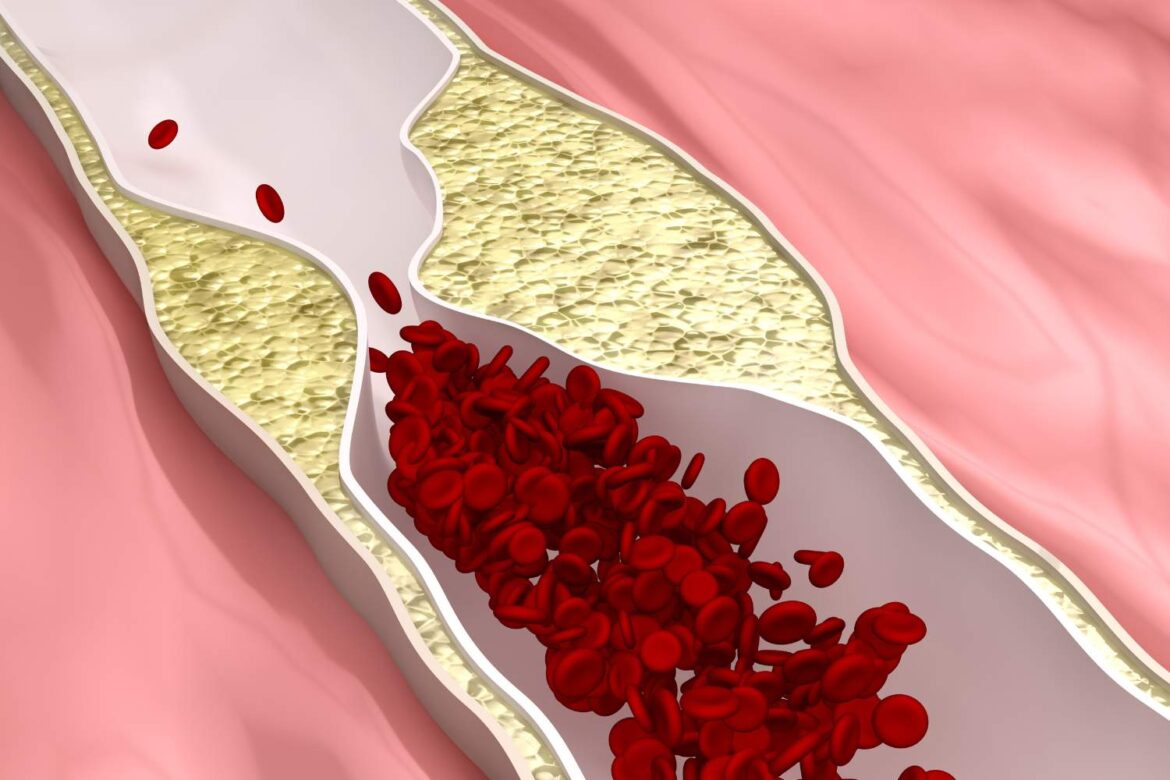
Coronary artery disease, also known as ischemic heart disease, is a chronic cardiovascular disorder characterized by progressive narrowing and hardening of the coronary vessels—the arteries responsible for delivering oxygen and nutrients to the heart muscle. The main underlying mechanism of this process is atherosclerosis, which involves the deposition of atherosclerotic plaques on the arterial walls. Over time, these plaques build up, hindering the free flow of blood. Insufficient oxygen supply to the heart leads to myocardial ischemia, causing characteristic symptoms such as chest pain (angina pectoris) and may result in dangerous complications, including heart attack. Coronary artery disease ranks among the leading causes of death worldwide and is recognized as a global health challenge, especially in highly developed countries where lifestyle habits promote risk factors such as a diet rich in animal fats, low physical activity, smoking, or chronic stress. Although coronary artery disease can progress for many years without symptoms, its effects are often dramatic when acute ischemia suddenly occurs. Very often, the first serious incident, such as myocardial infarction, becomes apparent only at an advanced stage of the disease. That is why this disease is referred to as a “silent killer.” It should be noted that symptoms of coronary artery disease can be atypical or vary in intensity depending on the individual, making correct diagnosis and therapeutic management highly individualized.
Understanding the basic mechanisms underlying the development of coronary artery disease is crucial for effective prevention and treatment. Endothelial injury – damage to the thin layer of cells lining the blood vessels – plays a significant role in the etiological process. This damage can be caused by factors such as high blood pressure, elevated LDL cholesterol levels, excessive free radicals, or the presence of diabetes. The damaged endothelium becomes a site for cholesterol and other lipid deposits, which are gradually surrounded by inflammatory cells, forming atherosclerotic plaques. Over time, these plaques may rupture or cause significant narrowing of the vessel lumen, impairing blood flow to the heart. When the heart’s demand for oxygen suddenly increases—during physical exertion, severe stress, or illness—such changes may provoke pain and potentially dangerous complications. Besides typical angina, the patient may experience various other symptoms, such as shortness of breath, fatigue, palpitations, or even fainting. Less commonly, so-called “silent ischemia” occurs—an asymptomatic form of coronary artery disease only discovered accidentally during diagnostic tests. Clinically, coronary artery disease presents in several forms, including stable angina, unstable angina, and heart attack as the most advanced form of acute ischemia. However, coronary artery disease is not inevitable; adequate knowledge, preventive measures, and treatment of risk factors can effectively slow its progression and improve quality of life for those at risk. Today, it is believed that a complex interplay of genetic and environmental factors determines the risk of developing coronary artery disease, which is why regular health monitoring and prompt response to early warning symptoms are so important.
Main Causes of Coronary Artery Disease Development
Coronary artery disease develops as a result of a complex interplay between genetic, environmental, and metabolic factors, which affect the functioning of the heart’s blood vessels. The key pathomechanism is atherosclerosis, meaning the accumulation of atherosclerotic plaques in the walls of the coronary arteries. Chronic endothelial damage, mainly caused by abnormal lipid profiles—especially high LDL cholesterol (“bad” cholesterol) and low HDL (“good” cholesterol)—is essential here. An unfavorable lipid profile causes cholesterol to accumulate in the artery wall, leading to the formation of atherosclerotic changes and gradual narrowing of the vessel lumen. Another key predisposing factor for vascular damage is persistently high blood glucose in people with diabetes or prediabetic states. Diabetes not only promotes atherosclerosis, but also intensifies inflammation, accelerating degenerative changes within the vessels. In addition, high blood pressure increases vascular resistance and stresses the artery walls, speeding up degeneration. Hypertension often co-occurs with other risk factors, amplifying adverse effects on the heart and vascular system.
Among the most important risk factors are also smoking—which directly damages the endothelium and increases platelet aggregation, favoring intravascular clot formation. Chronic stress is also harmful—those exposed to long-term psychological strain show elevated cortisol and adrenaline, which foster inflammation and high blood pressure. Lack of physical activity, a sedentary lifestyle, and excess calories result in gradually increasing body weight, which, apart from obesity, predisposes to insulin resistance, type 2 diabetes, and elevated blood triglycerides. Genetic predisposition is also crucial—if there are cases of premature coronary artery disease in the family, the risk increases significantly. Age and sex are also of importance: men after the age of 45 and women post-menopause are especially at risk, due to the loss of natural hormonal protection. Chronic inflammatory diseases, such as rheumatoid arthritis or chronic kidney disease, also negatively affect vascular health. The presence of several risk factors greatly accelerates the atherosclerotic process and worsens prognosis; thus, it is essential to control blood pressure, glucose, lipids, and eliminate environmental factors, especially smoking and obesity. Coronary artery disease does not result from a single factor—it’s the outcome of years of interaction of various lifestyle aspects, metabolic factors, and individual predisposition. The complexity of these processes means that recognition and effective prevention require a broad health context for each patient and systematic monitoring of all elements influencing coronary artery health.
Symptoms of coronary artery disease – how to recognize them?
Coronary artery disease may develop for a long time without any symptoms or present very subtle ailments easily attributed to other causes, such as fatigue or stress. Its most characteristic and recognizable symptom is chest pain, known by doctors as angina pectoris. This pain usually feels like pressure, tightness, or burning, is located behind the sternum, and may radiate to the left arm, shoulder, neck, jaw, back, or even the upper abdomen. Angina most often occurs in situations where the heart’s demand for oxygen increases, such as during intense exercise, psychological stress, strong emotions, heavy meals, or exposure to cold. In advanced forms of coronary artery disease, discomfort may even appear at rest, indicating significant narrowing of the arteries. Shortness of breath often accompanies chest pain, especially during physical activity or climbing stairs, resulting from insufficient oxygen supply to the cardiac muscle. Patients may also experience fatigue, weakness, palpitations, and dizziness, and sometimes fainting or temporary loss of consciousness. A particularly concerning symptom is a sudden decrease in exercise tolerance—that is, a noticeable difficulty in performing everyday activities that previously posed no problem. In some people, angina pain can be atypical—instead of classic chest pain, symptoms may include just nausea, abdominal discomfort, fatigue, or sweating. This atypical presentation is more common in women, the elderly, and people with diabetes, among whom abnormal pain perception is especially frequent. That is why it’s so important not to ignore any, even subtle, worrisome signals from your body.
Early symptoms of coronary artery disease are often mistaken for gastrointestinal, musculoskeletal, or respiratory complaints, which significantly delays proper diagnosis and treatment. Patients will often explain chest discomfort as the effect of excessive exertion, aging, or lack of physical fitness, even though nonspecific symptoms, such as chronic fatigue, sudden weakness, or shortness of breath, may indicate serious problems with the blood supply to the heart muscle. It must be remembered that in some cases, the first manifestation of ischemic heart disease can be a heart attack—a sharp, intense chest pain combined with anxiety, cold sweats, nausea, or loss of consciousness. For this reason, any sudden, previously unknown cardiovascular complaint should prompt immediate medical consultation. Vigilance is especially important in high-risk groups, such as those with high blood pressure, diabetes, hypercholesterolemia, smokers, or those with a family history. Recognition of coronary artery disease symptoms, therefore, requires special attention from both patient and physician—relying not only on typical anginal pains, but also on other, less obvious symptoms. Early detection, even of atypical complaints, and swift initiation of appropriate diagnostics significantly increases the chances for effective treatment and reduces the risk of serious cardiovascular complications.
Diagnosis of coronary artery disease: tests and process
The diagnostic process for coronary artery disease requires a multi-step approach that enables both the detection of the disease and precise assessment of the extent of changes in the coronary vessels and the risk of cardiovascular complications. Diagnosis begins with a thorough medical interview, paying particular attention to the nature and frequency of symptoms, risk factors (such as hypertension, diabetes, smoking, hypercholesterolemia, or family burden), as well as the patient’s lifestyle. The physician then conducts a detailed physical examination, evaluating, among other things, heart function, blood pressure, presence of murmurs over the heart, and any peripheral edema. The key phase of diagnosis involves a wide array of non-invasive and invasive tests, chosen individually depending on the disease form, presence of symptoms, and advancement of the disorder. Among the primary and frequently performed tests is the resting electrocardiogram (ECG), which can reveal arrhythmias, signs of heart muscle hypertrophy, and ischemia. However, given the possibility of asymptomatic disease or symptoms that only occur under stress, an exercise ECG (stress test – treadmill test or bicycle test) is also necessary, during which ECG changes linked to increased heart demand for oxygen are recorded. This exam allows an objective assessment of exercise tolerance and can unmask otherwise hidden cardiac ischemia, making it a valuable tool for chest pain differential diagnosis.
Another important step in diagnosing coronary artery disease is imaging, such as echocardiography (heart echo), which assesses the structure, function, and efficiency of the heart muscle, locates any ischemia, and detects complications such as heart attack or valve damage. Increasingly, non-invasive coronary CT angiography (coronary CTA) is performed, helping to evaluate the presence and extent of atherosclerotic plaques and the degree of vessel narrowing. In cases of high likelihood of coronary disease or unclear non-invasive results in patients with severe symptoms, invasive coronary angiography is performed—the gold standard of diagnostics—injecting contrast into the coronary arteries and taking X-ray images for clear visualization of narrowing or blockages. Besides imaging, labs assess total cholesterol, LDL, HDL, triglycerides, blood glucose, and inflammatory markers (CRP, homocysteine), helping to quantify risk and monitor treatment effectiveness. For difficult diagnoses, modern methods such as heart scintigraphy (SPECT) or cardiac MRI (with flow and viability assessment) can provide valuable information. It’s crucial that every case of coronary artery disease is approached individually, considering the patient’s age, comorbidities, symptoms, and risk of complications. The effectiveness of the entire diagnostic process relies on the appropriate combination of clinical interview, examination, lab tests, and imaging, enabling early detection, optimal treatment selection, and long-term disease control. The accuracy of modern diagnostic techniques means coronary artery disease is increasingly detected at the asymptomatic or early stage, opening up greater opportunities for prevention and effective treatment, slowing atherosclerosis progression and improving patients’ prognosis.
Effective treatment of coronary artery disease: pharmacotherapy, procedures, and lifestyle changes
Treatment of coronary artery disease is based on a comprehensive approach combining pharmacotherapy, advanced medical procedures, and major lifestyle modification. The aim of therapy is not only to reduce symptoms but above all to prevent complications such as heart attack, heart failure, or sudden cardiac death. Every patient requires an individual therapeutic strategy considering the course of the disease, its stage, coexisting conditions, and risk factors. Pharmacotherapy is the cornerstone of treatment, with a wide range of medications used. Most often, drugs are prescribed to reduce myocardial ischemia, including nitrates, beta-blockers, or calcium channel blockers. Their task is to decrease the heart’s oxygen demand, dilate coronary vessels, and improve exercise tolerance. Another key group are antiplatelet drugs, primarily acetylsalicylic acid, which limits the formation of intravascular clots. Statins lower LDL cholesterol, inhibit atherosclerosis progression, and reduce the risk of further cardiovascular events. For patients intolerant of statins or with insufficient therapeutic effect, PCSK9 inhibitors as well as ezetimibe may be used. Some patients additionally require ACE inhibitors or angiotensin receptor blockers, especially if hypertension, diabetes, or heart failure is present. The choice of drugs and doses is individualized, considering tolerance and effectiveness, with regular medical supervision essential for treatment safety.
For some patients, despite proper pharmacotherapy, progression of coronary artery narrowing or episodes of acute ischemia occur, requiring interventional procedures. The most common is percutaneous coronary angioplasty (PCI), restoring blood flow by dilating the narrowed vessel segment with a balloon and placing a stent. In cases of multivessel coronary disease or complex narrowing, coronary artery bypass grafting (CABG) is recommended—creating “detours” for blood to bypass blocked arteries. Indications for these procedures are based on imaging results, risk factors, and the patient’s general health. The success of interventions depends not only on procedural quality but also on further management—precise control of risk factors and ongoing drug therapy. An extremely important, yet often overlooked, pillar of therapy is lifestyle modification: dietary changes, increasing physical activity, combating obesity, quitting smoking, and managing stress effectively. Diet should be rich in vegetables, fruit, whole grains, fish, and low-fat protein sources, while low in saturated fats, cholesterol, salt, and simple sugars. Regular, individually adapted physical activity—for example, brisk walking, cycling, or swimming—improves cardiovascular and metabolic efficiency, reduces body weight, regulates blood pressure and lipids, and lowers blood sugar. Equally important is smoking cessation, since tobacco smoke compounds further vessel damage and destabilizes atherosclerotic plaques. Suitable psychological and pharmacological support may be necessary to quit the habit or manage chronic stress, which negatively affects the cardiovascular system by raising blood pressure, disturbing sleep, and triggering uncontrolled appetite. Education of patients and their families on healthy lifestyles, recognizing alarm signals, and motivating regular medical check-ups are among the most important elements for long-term success in treating coronary artery disease.
Prevention and prophylaxis of coronary artery disease
Prevention of coronary artery disease is a crucial element of public health policy, aimed not only at preventing the development of the disease itself but also at minimizing the risk of serious complications such as heart attack or sudden cardiac death. Effective preventive strategies are based on strict control of both modifiable and non-modifiable risk factors. The most important include hypertension, lipid metabolism disorders (high cholesterol, especially LDL), diabetes, obesity, smoking, low physical activity, unhealthy diet, chronic stress, and alcohol abuse. Meanwhile, age, male sex, family and genetic factors are risks beyond our control, but knowing about one’s own predisposition can motivate special care for a healthy lifestyle. It is currently estimated that with proper prevention, the overall risk of developing coronary artery disease in the population can be reduced by several dozen percent, thus combating the main causes of premature death in developed countries. Primary prevention is dedicated to healthy individuals—to prevent risk factors from developing or detect them early. Regular measurements of blood pressure, blood sugar, and lipid profile are recommended at least once a year, especially after the age of 40. This should be complemented by systematic physical activity—at least 150 minutes of moderate exercise weekly (e.g. brisk walking, cycling, swimming)—positively influencing blood vessel elasticity, glucose, and lipid metabolism. Dietary modification is equally important: the Mediterranean diet—rich in vegetables, fruits, nuts, whole grain cereals, lean fish, and healthy plant fats—not only prevents atherosclerosis but also helps stabilize body weight and regulate blood pressure. Limiting salt, simple sugars, red meat, and trans fats has positive effects on cardiovascular risk. Total elimination of smoking is also vital; smoking multiplies the risk of vessel spasm and atherosclerosis progression. Studies show that even twelve months after quitting, the risk of death from circulatory diseases decreases markedly and endothelial function improves within weeks. It is also important to reduce excessive stress, using relaxation techniques, such as breathing exercises, mindfulness meditation, or walking outdoors. Adequate sleep and psychological balance support heart function and help manage other risk factors.
Just as important as primary prevention is secondary prevention, aimed at people with diagnosed risk factors or after cardiovascular incidents—such as heart attack, stroke, or revascularization procedures. Secondary actions focus on strict monitoring of vital signs: regular checks of cholesterol, triglycerides, glycemia, blood pressure, as well as systematic use of pharmacotherapy as recommended by the doctor. It is crucial to follow recommendations regarding statins, beta-blockers, ACE inhibitors, antiplatelet drugs, and, if necessary, other preparations reducing thrombosis or atherosclerosis progression risk. Participation in cardiac rehabilitation programs is also recommended—they help return to active life, teach healthy habits, and minimize fear of repeat cardiac events. Health education plays a paramount role: an aware patient is more likely to cooperate with the therapeutic team and to implement everyday changes. Significant support from family, ready to motivate the patient to continue treatment and develop lasting healthy behaviors, is crucial. Modern prevention programs conducted at primary care offices, cardiac outpatient clinics, and via community education campaigns increase risk factor detection and enable special care for the most vulnerable people. Digital tools—health-monitoring apps, educational platforms, and teleconsultations—are playing an increasing role, helping ensure regular health monitoring and raising public awareness of coronary artery disease prevention. Ultimately, effective prevention requires cooperation among many entities—from patients, the medical community, to institutions responsible for systemic solutions and promoting a healthy lifestyle throughout society.
Summary
Coronary artery disease is one of the most common and serious heart conditions, but with early diagnosis and conscious lifestyle changes, its progression and symptoms can be effectively limited. Careful attention to initial symptoms, appropriate diagnosis, and effective treatment—including medication and a healthy diet—allow patients to improve quality of life and prevent dangerous complications. Prevention also remains key—regular physical activity, balanced diet, weight control, and avoidance of risk factors. By caring for your heart, you gain the chance for a longer, healthier life.