Gout – discover the causes, symptoms, effective treatment, and recommended diet. Find out how to prevent recurrences and take care of your health.
Table of Contents
- What is gout? Causes of the disease
- Most Common Gout Symptoms – How to Recognize Them?
- Gout Diagnosis – Key Examinations
- Gout Treatment – Drugs and Therapeutic Strategies
- Gout Diet – What to Eat and What to Avoid?
- Prevention and Avoiding Recurrences of Gout
What is gout? Causes of the disease
Gout, also known as podagra, is a chronic metabolic disease caused by excessive deposition of sodium urate crystals in body tissues, especially in the joints and periarticular tissues. The main factor leading to the development of gout is hyperuricemia, i.e., elevated uric acid levels in the blood. Uric acid is produced as the terminal product of purine breakdown – compounds present both naturally in body cells and supplied through the diet. When the balance between the production and excretion of uric acid is disturbed, it starts to deposit in the form of microscopic crystals, triggering an inflammatory response and pain. In addition to the joint system, gout can also lead to kidney damage, nephrolithiasis, and cardiovascular complications.
Many factors contribute to the development of gout, which can be divided into primary and secondary. In primary gout, the disorders are genetic and related to a defect in purine metabolism, causing the body to naturally produce more uric acid or be unable to effectively excrete it. Secondary gout develops due to other diseases and disorders, such as chronic kidney failure, hypertension, diabetes, obesity, and as a result of certain medications (e.g., diuretics or some cytostatic drugs). Environmental and lifestyle factors also play an important role, such as a diet rich in purines (excessive consumption of red meat, offal, seafood, alcohol – especially beer), lack of physical activity, frequent dehydration, and chronic stress. Elevated uric acid levels are more often observed in men over the age of 40 and in women after menopause, but the disease can also affect younger people. It is also worth noting that a family history increases the risk of developing this condition, so people with cases of gout in the family should pay special attention to risk factors. Other potential causes of gout include metabolic disorders such as metabolic syndrome, and excessive body weight promotes increased production and simultaneous reduction in excretion of uric acid by the kidneys. All these elements make gout a civilization disease, whose incidence is increasingly observed among inhabitants of developed countries.
Most Common Gout Symptoms – How to Recognize Them?
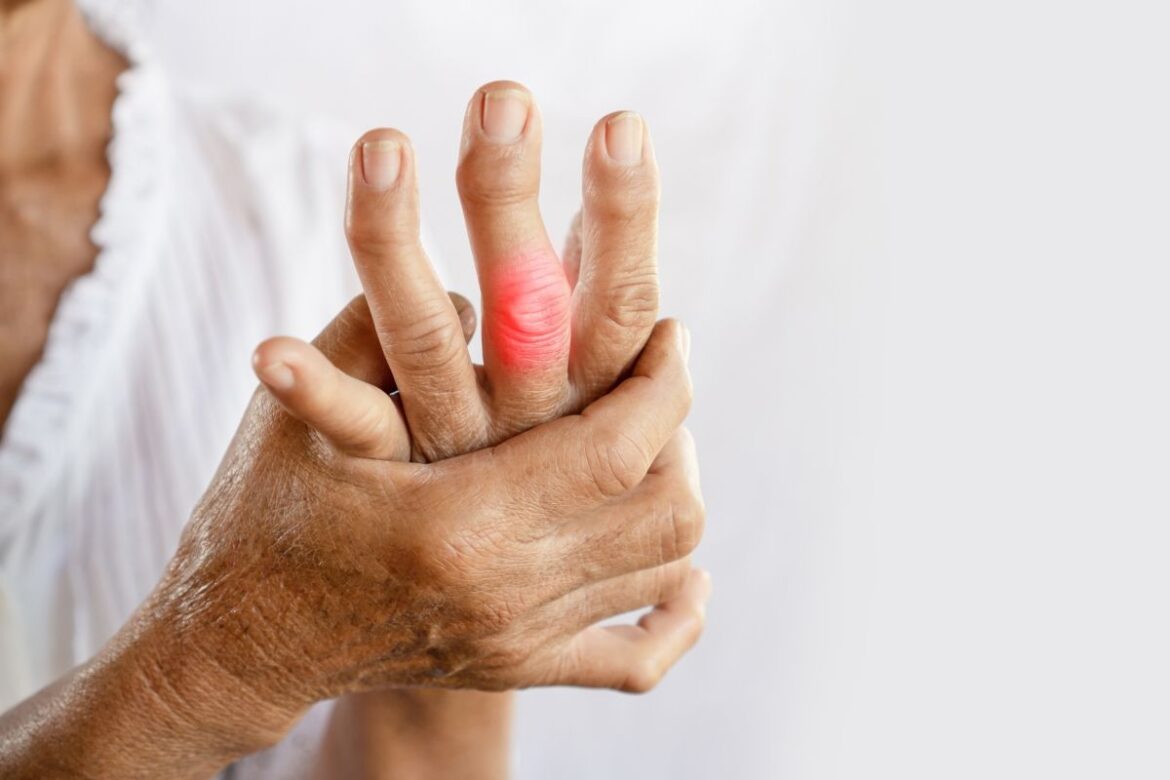
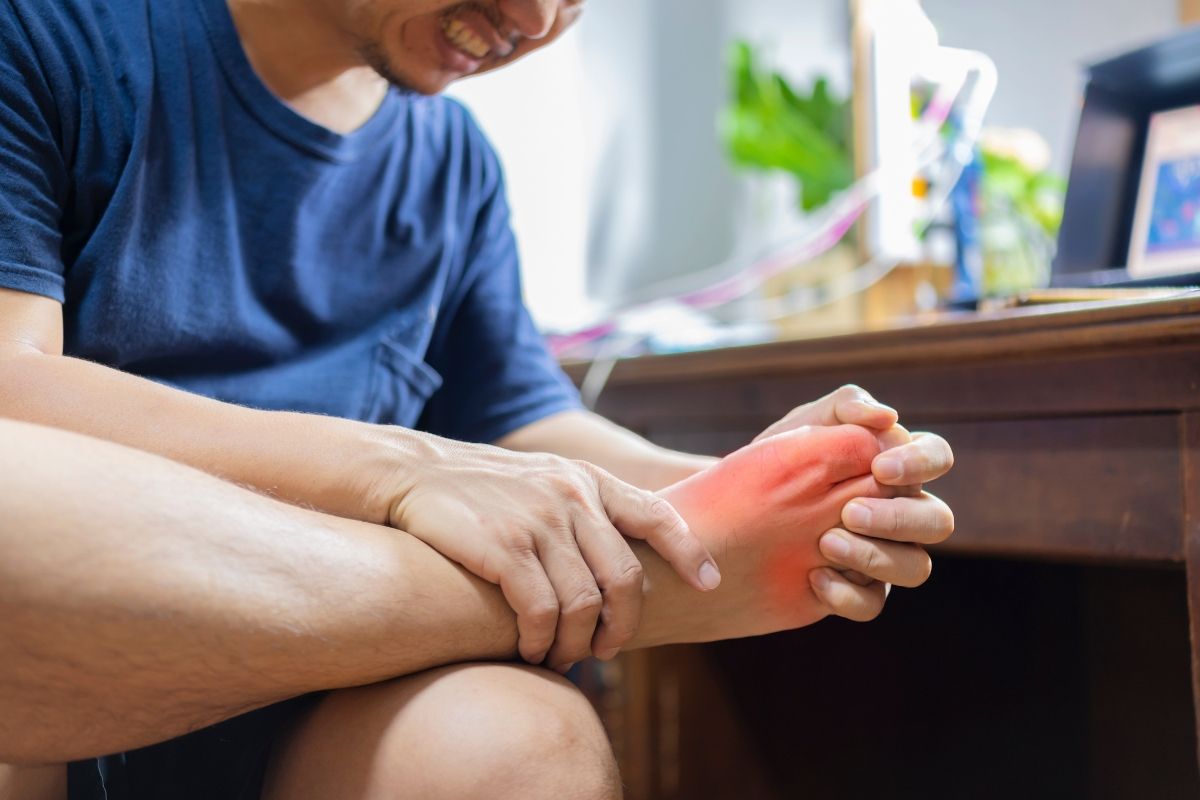
Gout primarily manifests as sudden and very severe joint pain, which most often appears at night or in the early morning hours. A gout attack can surprise even previously healthy individuals, and the intensity of the pain makes even a gentle touch or slight brushing of the affected joint extremely painful. A characteristic symptom is also redness, swelling, and increased temperature of the skin over the affected joint. In most cases, the first joint to become inflamed is the big toe’s metatarsophalangeal joint (so-called podagra), though any other joint may be affected, e.g., the knee, ankle, wrist, or elbow. These symptoms have a rapid onset and develop within a few hours, reaching peak intensity within 24 hours. Gout attacks are often accompanied by general malaise, fever, chills, or even a sense of weakness or reduced appetite, differentiating gout from other rheumatic diseases. Usually, symptoms subside spontaneously after a few days to 2 weeks, but untreated gout becomes chronic, leading to recurrent attacks and permanent joint changes.
As the disease progresses, gout symptoms may intensify and become less typical. Over time, pain attacks occur more frequently and affect more joints (polyarticular gout). Some people develop characteristic tophi – hard, painless lumps located under the skin around joints, tendons, and sometimes on the auricles or elbows. These form as a result of many years of sodium urate crystal deposition and can lead to tissue damage, joint deformities, and loss of function. Laboratory tests show elevated uric acid levels in the blood, and with chronic progression, symptoms of kidney damage may appear, such as swelling or high blood pressure. Sometimes, gout starts with atypical symptoms, e.g., chronic back pain or small skin changes, leading to delayed diagnosis. Therefore, gout diagnosis is based not only on the evaluation of clinical symptoms but also on additional tests, such as joint fluid analysis for the presence of sodium urate crystals, blood tests, and imaging diagnostics. Early recognition and accurate diagnosis are crucial to prevent complications and irreversible damage to the musculoskeletal system. Therefore, it is important to pay attention to the first symptoms of an attack, especially in people with risk factors for gout.
Gout Diagnosis – Key Examinations
Gout diagnosis is based on a thorough medical history, observation of clinical symptoms, and the results of specialized laboratory and imaging tests. The key element is confirming hyperuricemia, or elevated blood uric acid, but the presence of this marker alone is not sufficient for diagnosis – many people with elevated levels never experience gout attacks. For this reason, doctors focus primarily on directly identifying sodium urate crystals in joint fluid obtained by arthrocentesis. Microscopic examination of synovial fluid is the gold standard in diagnosis: using polarized light microscopy, characteristic needle-like crystals can be identified, confirming the diagnosis. In some cases, samples may be taken from tophi or periarticular tissues. Besides synovial fluid analysis, serum uric acid measurement is commonly ordered – values over 6.8 mg/dl are considered elevated, although during acute attacks these may even be normal or reduced, so interpreting results always requires clinical experience and must be correlated with the patient’s disease presentation. Additional lab tests include markers of inflammation, such as ESR (erythrocyte sedimentation rate) and CRP (C-reactive protein), which are often increased during a gout attack.
The broader diagnostic process also utilizes imaging tests, especially ultrasound (USG), which visualizes joint inflammation, synovial fluid, and sodium urate deposits in soft tissues – especially in patients with chronic gout. In ultrasound, characteristic signs include the “double contour sign,” indicating urate crystals on joint cartilage surfaces. In diagnostically challenging cases, computed tomography (CT), magnetic resonance imaging (MRI), and X-rays may be used to detect late bone structure changes and erosions. Gout diagnosis is not limited to confirming the disease; it is also important to identify risk factors and any comorbidities, such as hypertension, diabetes, obesity, or chronic renal failure. This is supported by additional laboratory tests, including kidney function assessment (creatinine, eGFR), lipid panel, or blood glucose. Thanks to such a comprehensive approach, it is possible not only to confirm a diagnosis of gout but also to individualize treatment and monitor therapy progress and complication risks. It is worth remembering that collaboration with an experienced rheumatologist or internist increases diagnostic accuracy and helps prevent irreversible changes in joints and kidneys.
Gout Treatment – Drugs and Therapeutic Strategies
Gout treatment is based on a comprehensive approach encompassing pharmacotherapy, lifestyle modification, and management of co-morbid diseases. The key goal of therapy is to alleviate acute inflammation, lower uric acid levels (hyperuricemia), and prevent recurrences and complications. In an acute gout attack, the first step is to relieve pain and suppress inflammation – nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, naproxen, or indomethacin, are used for rapid reduction of pain and joint swelling. If NSAIDs are contraindicated or insufficient, the doctor may prescribe colchicine, known for its anti-inflammatory action, but its dosage must be closely controlled due to the risk of gastrointestinal side effects. Glucocorticoids, administered orally, intravenously, or intra-articularly, are an alternative or adjunct, especially if other methods are inadequate or contraindicated. The choice of treatment method and intensity depends on the severity of symptoms, co-morbidities, and patient’s individual drug tolerances.
Once the acute inflammation is controlled, long-term uric acid management becomes the key element of therapy. The basis of chronic treatment is drugs that lower uric acid level – uricosuric agents (increase uric acid excretion with urine, e.g., probenecid) and xanthine oxidase inhibitors (inhibit uric acid production, such as allopurinol or febuxostat). Medication choice depends on the patient profile, kidney function, tolerance of each drug, and any contraindications. Pharmacotherapy is often supported by non-pharmacological therapeutic strategies, including weight reduction, limiting alcohol, introducing a low-purine diet, and increasing physical activity. It is also very important to avoid triggers such as dehydration or excessively rapid weight loss. In severe cases or in patients with tophi, biological therapy using pegloticase – an enzyme breaking down uric acid, used in selected resistant cases – may sometimes be considered. Regular control of uric acid, systematic medication use, and patient education play essential roles in preventing flare-ups and complications such as joint or kidney damage. Effective treatment requires an individual approach and close cooperation with a rheumatologist, and sometimes consultation with a dietitian or nephrologist, especially if other metabolic disorders are present. Properly managed therapy allows remission of the disease and improves patients’ quality of life, even with chronic gout.
Gout Diet – What to Eat and What to Avoid?
Diet plays a key role in the treatment and prevention of gout, being one of the most effective non-pharmacological elements of therapy. A properly balanced menu makes it possible to control uric acid concentration in the blood by limiting the intake of purine-rich foods, which are the precursor to uric acid. The basis of a gout diet is to avoid or significantly limit red meats, especially beef, pork, lamb, and offal such as liver, kidneys, and pancreas. Poultry, though less purine-rich, should also be eaten in moderation. Fatty fish such as sardines, herring, mackerel, anchovies, and shellfish are also inadvisable, as they can sharply raise uric acid levels. Strongly forbidden are meat and bone extracts, canned foods, highly processed meat products, and stock cubes. Another group to avoid are legumes such as peas, beans, lentils, and broad beans, as well as spinach, rhubarb, and asparagus, which, despite their nutritional value, still contain relatively high levels of purines.
Beverages have a significant impact on the course of the disease – absolutely eliminate alcohol, especially beer and strong liquors, as these hinder the kidneys’ excretion of uric acid and promote acute gout attacks. Reducing sugar and foods high in sugar content, such as sweetened drinks, cakes, and confectionery is also important, since excessive fructose intake increases uric acid production. Body weight control is crucial – overweight and obesity promote the development of gout, so the diet should be based on rational, easily digestible nutrition and a caloric deficit in overweight individuals. Recommended foods include low-fat dairy products such as natural yoghurts, kefir, and milk, which can additionally lower uric acid levels. Eggs, whole grains, wheat pasta, rice, groats, and potatoes are also allowed and encouraged. Large amounts of vegetables (excluding the aforementioned), fruits (especially berries and citrus), which, due to their antioxidant properties, support the fight against inflammation, are recommended. Proper hydration is very important – it is recommended to drink at least 2-3 liters of fluids daily, mainly mineral water, weak fruit and herbal teas, while avoiding caffeine and carbonated drinks. Limiting saturated fats and table salt also protects the cardiovascular system, which is key for people with gout. Meals should be regular, light, and preferably boiled or stewed; frying and deep-fat baking should be kept to a minimum. In daily meal planning, it is worth choosing nuts, seeds, healthy vegetable oils, and natural herbal spices, which not only enhance taste but also have anti-inflammatory properties, supporting treatment and helping prevent gout relapses.
Prevention and Avoiding Recurrences of Gout
Effective prevention and avoidance of gout recurrences require a multi-faceted approach combining long-term lifestyle modification, ongoing laboratory monitoring, and appropriate pharmacological treatment under the guidance of a specialist. A key role is played by maintaining healthy body weight and avoiding overweight, as excess fat tissue promotes both production and retention of uric acid. Weight reduction should be gradual, with a well-balanced low-purine diet rich in vegetables (excluding types high in purines such as spinach, peas, or asparagus), fruits, and low-fat dairy products. Highly processed foods, fatty meats, sardine- or herring-type fish, as well as fructose and sugary sodas that can increase uric acid levels, should be eliminated. Alcohol – especially beer and spirits – should absolutely be avoided, as their consumption is linked to a higher risk of acute attacks, disturb uric acid excretion, and promote dehydration. Regular, moderate physical activity (e.g., brisk walking, cycling, swimming) supports metabolism, improves circulation, and cardiovascular fitness. It is recommended to spend at least 30 minutes a day in physical activity, adjusting intensity to your abilities and doctor’s recommendations. An active lifestyle also helps control other risk factors, such as type 2 diabetes, lipid disorders, or hypertension, which often coexist with hyperuricemia and increase the recurrence risk of gout attacks.
An essential element of prevention is systematic monitoring of blood uric acid levels and regular check-ups for kidney function and inflammation markers. Patients at especially high risk of recurrence (e.g., with comorbidities, a history of gout attacks, or a family history of gout) should be under close care of a rheumatologist, who will adjust therapy as needed and apply preventive pharmacological treatment. Most commonly, uric acid–lowering drugs – allopurinol or febuxostat – are used, which inhibit its synthesis; in selected patients, uricosurics that increase uric acid excretion may be prescribed. Consistent medication adherence is crucial: interruptions or irregularity increases the risk of acute attacks and long-term complications, such as kidney damage or chronic joint inflammation. Aside from pharmacotherapy, patient education is equally important: recognizing prodromal symptoms and self-monitoring allow quick intervention and avoidance of full-blown attacks. Adopting habits that support prevention is recommended, such as drinking plenty of water (2–3 liters daily, unless contraindicated by other medical conditions), avoiding severe stress, sleeping well, and maintaining life balance. Removing environmental risk factors, managing stress, promoting sleep hygiene, and psychological support can significantly influence the disease course and reduce relapse frequency. Optimal prevention results are achieved through close cooperation with the medical team and active implementation of recommendations, adjusted to the patient’s lifestyle, work pattern, and comorbidities.
Summary
Gout is a chronic disease that requires proper treatment and a conscious approach to diet. Early symptom recognition and regular check-ups help reduce the negative effects of the disorder. Adhering to medical recommendations, appropriately chosen anti-inflammatory drugs, and avoiding purine-rich foods effectively support treatment and decrease the risk of recurrence. Remember, prevention, a healthy lifestyle, and regular physical activity are the keys to maintaining joint health for years to come.