Find out what atherosclerosis is: learn about its symptoms, causes, treatment methods, and prevention strategies. Discover how to effectively protect your health every day!
Table of Contents
- What is atherosclerosis? Definition and characteristics of the disease
- Most common symptoms of atherosclerosis – how to recognize them?
- Causes and risk factors for the development of atherosclerosis
- Diagnostics – when to see a doctor?
- Atherosclerosis treatment methods – pharmacological and non-pharmacological
- Prevention of atherosclerosis – effective ways to prevent the disease
What is atherosclerosis? Definition and characteristics of the disease
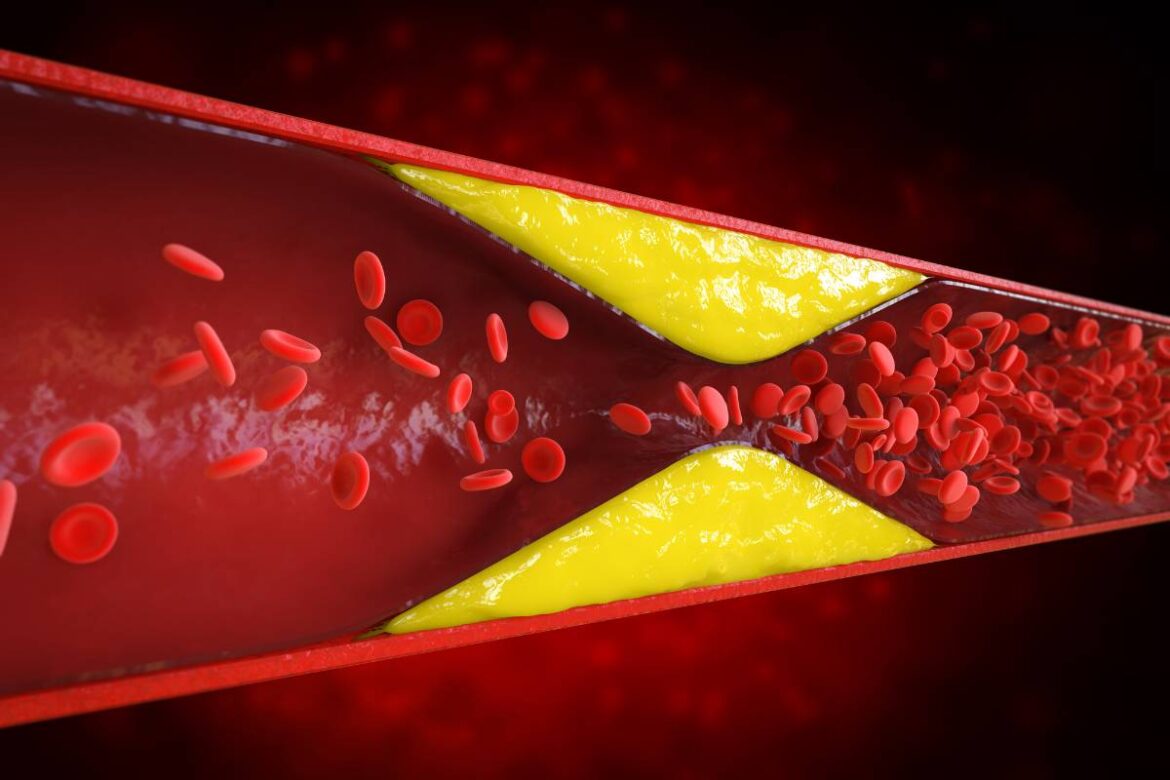
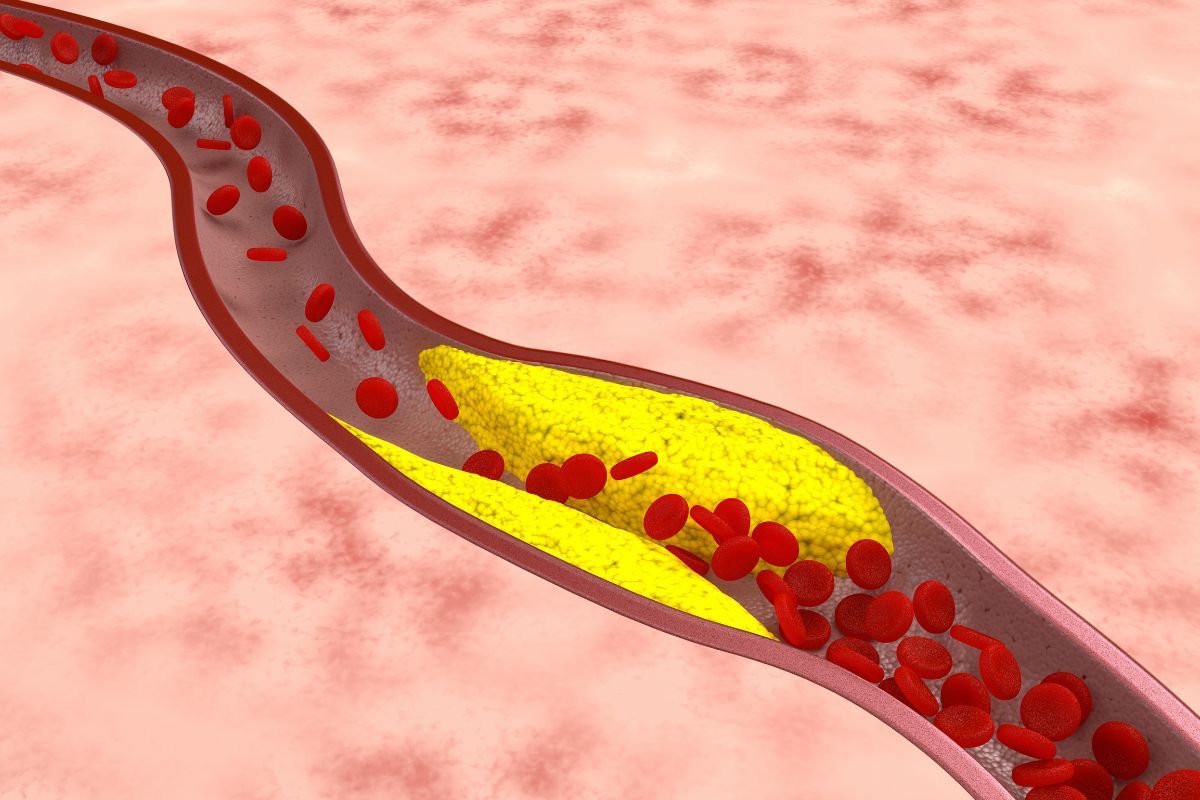
Atherosclerosis, also known as arteriosclerosis, is a chronic, progressive disease of the arterial vessels that plays a key role in the development of cardiovascular diseases, which are the most common cause of death in developed countries. The essence of the atherosclerotic process is the gradual deposition of so-called atherosclerotic plaques in the walls of arteries, composed primarily of lipids (mainly cholesterol), proteins, calcium, and inflammatory cells. This process typically starts in early adulthood and can remain asymptomatic for many years, leading to narrowing of the arteries, their hardening, and loss of elasticity. This disruption in the function of arteries—responsible for transporting oxygenated blood to all tissues and organs—directly leads to ischemia of key body areas, such as the heart, brain, or lower limbs. Importantly, atherosclerosis is not just a local problem affecting a single artery, but is considered a generalized disease of the entire vascular system, significantly increasing the risk of serious complications such as myocardial infarction, stroke, coronary artery disease, or organ failure.
The development of atherosclerosis involves a series of stages that can take several or even dozens of years before clinical symptoms manifest. In the initial phase of atherosclerosis, the endothelium (the thin layer of cells lining the arteries) is damaged, facilitating the penetration of LDL cholesterol molecules into the vessel wall and their oxidation. In response, the body triggers an inflammatory reaction that prompts immune cells (macrophages) to migrate and engulf accumulated fats, creating so-called foam cells— the basic building blocks of atherosclerotic plaques. These plaques gradually enlarge, causing artery narrowing, impaired blood flow, and increasing the risk of blood clots. In advanced stages, plaques may rupture, resulting in the formation of a thrombus that blocks blood flow and directly leads to life-threatening events such as heart attack or stroke. A characteristic feature of atherosclerosis is that it most often develops in medium and large arteries— including the coronary, carotid, cerebral, and lower limb arteries— which is why it causes a wide range of complications depending on the location of the changes. Despite clear morphological changes in the vessels, atherosclerosis may remain symptomless for a long time, so it is considered the “silent killer.” Only significant blood flow restriction manifests as pain, organ dysfunction, intermittent claudication, or even sudden death. Atherosclerosis is not an inevitable consequence of vascular aging but results from the combination of multiple risk factors, such as an improper diet rich in saturated fats and cholesterol, smoking, lack of physical activity, hypertension, diabetes, obesity, and family predisposition. Understanding what atherosclerosis is, how it develops, and how degeneration of vessel walls progresses allows for a full appreciation of the serious health consequences associated with this disease, emphasizing the need for consistent prevention and effective treatment.
Most common symptoms of atherosclerosis – how to recognize them?
Atherosclerosis can develop for many years without noticeable symptoms, and the first signs often appear only when vascular changes are already advanced. The symptoms depend on the location and extent of arterial narrowing, so they may vary greatly between individuals. Symptoms are most often related to ischemia in specific organs—heart, brain, lower limbs, or kidneys. In the case of coronary arteries supplying blood to the heart muscle, one of the main symptoms is chest pain, known as angina pectoris. Patients describe this pain as pressure, choking, or burning, often radiating to the arm, neck, jaw, or back. It may occur during physical exertion, stress, and in more advanced cases—even at rest. Shortness of breath, a feeling of heaviness in the chest, palpitations, fatigue, and general weakness are also typical symptoms indicating narrowing of the coronary arteries. When atherosclerosis affects the arteries supplying blood to the brain (carotid and vertebral arteries), it may manifest as dizziness, transient visual disturbances, speech or balance problems—so-called transient ischemic attacks (TIA). Affected individuals may suddenly have difficulty maintaining motor coordination, experience unilateral weakness or numbness of limbs, a drooping mouth corner, and, in more severe cases, suffer a full-blown ischemic stroke. Early recognition of these warning signs is crucial because timely intervention can save lives and minimize permanent nervous system damage.
Another characteristic symptom of atherosclerosis arising from changes in the arteries of the lower limbs is intermittent claudication. This is a sensation of pain, burning, fatigue, or cramping in the calves that occurs during walking and passes after a short rest. As the disease progresses, the distance a patient can walk without pain gradually decreases. These symptoms result from inadequate oxygen supply to the muscle tissues of the legs. Advanced stage atherosclerosis of the lower limbs can lead to chronic ulcers, hard-to-heal wounds, necrosis, and even the necessity for amputation. Atherosclerosis can also manifest as erectile dysfunction in men or kidney deterioration if the disease affects the renal arteries. It is important to note that these symptoms are very often ignored by patients or attributed to other ailments, such as “ordinary” muscle pain or aging. Atherosclerosis is especially insidious because of its hidden course, where the first and often dramatic symptom may be a heart attack, stroke, or sudden worsening of limb blood supply. For this reason, even subtle, recurring, or new complaints such as pain, numbness, cramps, weakness, or mobility issues should always prompt consultation with a doctor and diagnostic tests to assess the circulatory system, including blood pressure measurement, a lipid profile, or non-invasive imaging tests such as Doppler ultrasound of the arteries or CT angiography. Early identification of atherosclerosis symptoms significantly increases the chances of effective treatment and limiting dangerous complications.
Causes and risk factors for the development of atherosclerosis
Atherosclerosis develops through a complex interaction of genetic, environmental, and lifestyle factors that gradually damage the blood vessel walls. The main initiating cause is chronic damage to the endothelium—the thin layer of cells lining the arteries that is responsible for proper blood flow, blood pressure regulation, and protection against adhesion of inflammatory cells and lipids. This damage may be mechanical or chemical in nature, and is usually the result of long-term exposure to factors such as high blood pressure (hypertension), tobacco smoke, hyperglycemia in diabetes, or chronic inflammation. An unhealthy diet high in saturated fats, trans fats, and cholesterol is particularly harmful as it leads to elevated levels of “bad” LDL cholesterol in the blood, which readily deposits in arterial walls. Additional factors favoring atherosclerosis include a lack of unsaturated fats (omega-3, omega-6), fresh vegetables and fruits—thus, low-fiber diets increase susceptibility to development of the disease.
The key risk factors for atherosclerosis prominently include cigarette smoking, which not only damages the endothelium but also exacerbates inflammatory processes and increases blood viscosity, promoting clot formation. Physical activity plays a protective role, whereas its lack increases atherosclerosis risk because it worsens lipid metabolism, increases hypertension, and promotes insulin resistance and obesity. Chronic stress is also a significant factor, negatively affecting hormonal balance, blood pressure, and eating habits. Overweight and obesity, especially abdominal type, cause increased triglycerides, LDL, and reduced “good” HDL cholesterol, disrupting lipid balance and promoting chronic microinflammatory processes in the vessel walls. Underlying many cases of atherosclerosis is also type 2 diabetes—chronic hyperglycemia causes endothelial glycation, increasing permeability for LDL cholesterol and disrupting anti-inflammatory signaling pathways. Genetic predisposition is also important, with familial hypercholesterolemia, obesity, or early heart disease placing individuals at higher risk, even when maintaining healthy lifestyle habits. Age and gender also play a role—the risk of atherosclerosis increases after age 45 in men and post-menopause in women, due to hormonal changes and the loss of the protective effects of estrogen. Less commonly recognized, but increasingly emphasized factors include chronic bacterial and viral infections, insomnia, homocysteine metabolism disorders (hyperhomocysteinemia), and exposure to air pollution. The coexistence of multiple risk factors usually works synergistically, significantly accelerating the development and progression of atherosclerosis. Prevention focused on minimizing environmental factors and early diagnosis of metabolic disorders forms the foundation of today’s strategies for combating this disease, but its effectiveness largely depends on individual commitment and permanent lifestyle changes.
Diagnostics – when to see a doctor?
Early detection of atherosclerosis is crucial to prevent serious complications such as heart attacks or strokes, so it is extremely important not to ignore even subtle symptoms that may indicate the onset of vascular disease. There are many warning signs that require prompt medical attention—chief among them: recurrent chest pain and pressure, shortness of breath on minor exertion, limb weakness, sensations of cold or numbness in the feet and hands, as well as visual disturbances, sudden dizziness, or problems with speech and balance. A specialist visit should also be prompted by the presence of risk factors such as chronic hypertension, diabetes, significant overweight, or a family history of cardiovascular disease. It is crucial to note that even mild or transient symptoms should not be ignored—especially in individuals over 40, smokers, those leading a sedentary lifestyle, or those with improper diets. Regular preventive check-ups—monitoring cholesterol levels, blood pressure, fasting glucose, or body mass index (BMI)—should become routine, not only for those already identified with risk but for all adults, since atherosclerosis can progress asymptomatically for many years.
The atherosclerosis diagnostic process usually begins with a thorough medical interview, in which the specialist analyzes symptoms, patient lifestyle, and risk factors, followed by a physical examination—assessing, among other things, limb pulses, presence of vascular murmurs, and the condition of the skin and mucous membranes. The next stage involves laboratory tests, including lipid profile (total cholesterol, LDL, HDL, triglycerides), glucose level, and kidney function parameters. Modern imaging techniques play an extremely important role in diagnosis. The most commonly used are Doppler ultrasonography of peripheral and carotid arteries, computed tomography (angio-CT), and magnetic resonance angiography, which allow for detailed assessment of arterial narrowing, the presence of atherosclerotic plaques, and blood flow. In patients suspected of coronary atherosclerosis, stress tests, echocardiography, or coronary angiography may be performed, especially if there is a risk of heart attack or typical angina symptoms. The so-called ABI (ankle-brachial index) is also important for detecting ischemia in the lower limbs—it enables rapid identification of even early arterial changes. The diagnostics of atherosclerosis are multi-staged and should always be supervised by a specialist, who, based on test results, will select an appropriate plan for further management—both in terms of pharmacology and comprehensive lifestyle modification. Consistent medical monitoring and prompt response to any alarming symptoms make it possible to slow disease progression and significantly improve health prognosis.
Atherosclerosis treatment methods – pharmacological and non-pharmacological
Treatment of atherosclerosis is a multi-stage process aimed not only at slowing disease progression but also effectively preventing complications such as heart attack, stroke, or organ failure. A multidisciplinary approach is essential, combining pharmacological therapies with non-pharmacological lifestyle changes. Pharmacological treatment focuses primarily on lowering “bad” LDL cholesterol and stabilizing atherosclerotic plaques. The most commonly used are statins, which effectively reduce cholesterol levels and decrease the risk of cardiovascular events. In cases of statin intolerance or insufficient effectiveness, a doctor may recommend ezetimibe or PCSK9 inhibitors—more modern therapeutic options. Fibrates are often used, especially in patients with diabetes and high triglyceride levels. In addition to lipid-lowering drugs, treating hypertension is also critical—agents such as angiotensin-converting enzyme inhibitors (ACE-I), sartans, and beta-blockers benefit vessel walls and inhibit atherosclerotic plaque growth. In specific cases, especially with coexisting heart disease, antiplatelet drugs such as acetylsalicylic acid are recommended to reduce the risk of clot formation. Glycemic control in diabetics is equally important, with agents that improve insulin sensitivity and oral hypoglycemic drugs being crucial. Besides conventional drug therapy, advanced cases of atherosclerosis and life-threatening situations may require invasive treatment: balloon angioplasty, stent implantation, or even coronary artery bypass surgery. Effective pharmacological therapy must always be coupled with regular effectiveness monitoring (lipids, blood pressure, glucose) and individualized treatment based on age, comorbidities, and atherosclerosis stage.
Alongside standard pharmacological treatment, non-pharmacological methods play a significant role in atherosclerosis therapy, helping to improve vessel condition and slow disease progression. The foundation of both prevention and treatment is lifestyle modification, particularly adopting a Mediterranean or DASH (Dietary Approaches to Stop Hypertension) diet, rich in vegetables, fruits, whole grains, fish, healthy plant-derived fats, and minimal in salt or saturated fats. Regular physical activity is equally crucial—at least 150 minutes of moderate effort per week (walking, cycling, swimming) is recommended, affecting weight control, risk reduction of obesity, and improving cardio-respiratory fitness. An important non-pharmacological intervention is complete smoking cessation and avoidance of passive smoking, which radically increases the risk of atherosclerotic complications. Working on stress control, relaxation techniques, and psychotherapy also play a growing role in improving the overall health of patients with atherosclerosis. Sufficient sleep, limiting alcohol consumption, and maintaining a healthy weight should be daily preventive practices. Modern medicine also recognizes the importance of health education and regular consultations with specialists (cardiologist, diabetologist, dietitian), enabling rapid detection of complications and treatment adjustment. Non-pharmacological interventions, although they require patient commitment and self-discipline, can significantly inhibit atherosclerosis progression and reduce the need for aggressive drug therapy or surgical procedures. Only comprehensive therapy, integrating both modern pharmacological methods and conscious lifestyle changes, offers a real chance of improving quality of life and significantly reducing cardiovascular risk.
Prevention of atherosclerosis – effective ways to prevent the disease
Atherosclerosis prevention is based on a multidimensional approach aimed at eliminating or maximally reducing the risk factors that lead to this dangerous vascular disease. Implementing a healthy lifestyle at an early stage is crucial, since atherosclerotic plaques often start accumulating long before clinical symptoms appear. The most important element of effective prevention is regular physical activity, adjusted to age and physical capabilities. Exercise lowers LDL cholesterol and triglyceride levels, helps maintain a healthy weight, improves insulin sensitivity, and positively affects blood pressure. It is recommended to engage in at least 150 minutes of moderate-intensity activity per week, such as brisk walking, cycling, or swimming, and to limit sedentary habits. A healthy diet—rich in vegetables, fruits, whole grains, legumes, nuts, and healthy unsaturated fats found in marine fish and olive oil—is also crucial for atherosclerosis prevention. Reducing consumption of saturated fats found in fatty meats, dairy products, processed foods, and eliminating trans fats from fast food and sweets is essential. Salt intake should be minimized, replaced by herbs and spices; high sodium intake increases blood pressure and accelerates atherosclerotic changes. Regular weight control and maintaining a proper BMI are essential—overweight and obesity strongly correlate with atherosclerosis risk.
Avoiding harmful habits is equally critical in preventing atherosclerosis—the priority is to quit smoking, which greatly increases the risk of vascular changes and their dangerous complications. Cigarette smoke damages the endothelium, intensifies pro-inflammatory reactions, and accelerates plaque accumulation, so complete nicotine abstinence is one of the most effective preventive measures. Alcohol consumption should also be limited; excessive drinking raises blood pressure, promotes obesity, disrupts lipid and carbohydrate metabolism, and damages the liver. Regular monitoring of biochemical parameters, such as a lipid profile (LDL, HDL, triglycerides), blood glucose, and blood pressure, allows for early detection of abnormalities and implementation of preventive measures in time. Managing stress is also key—chronic stress promotes inflammation and high blood pressure, so relaxation techniques, yoga, meditation, or other active forms of rest are recommended. Prevention also includes maintaining a regular sleep schedule and ensuring adequate hours of rest—lack of sleep and an irregular lifestyle disrupt hormonal and metabolic balance, increasing predisposition to the disease. At-risk individuals, such as those with a family history, diabetes, hypertension, or kidney disease, should have regular specialist check-ups and follow medical recommendations. Modern prevention increasingly relies on health education, promoting screening programs, and increasing awareness about risk factors—comprehensive measures noticeably reduce atherosclerosis incidence at the stage of primary prevention. Environmental and social factors, such as air quality and access to healthy food, also play a role and may support or hinder the implementation of a healthy lifestyle. Effective atherosclerosis prevention is an investment in the future of society and one of the most important public health strategies.
Summary
Atherosclerosis is a silent and insidious disease that can develop over the years without prominent symptoms. Early diagnosis is crucial for effective treatment and limiting its progression. Risk factors such as poor diet, lack of physical activity, or smoking can be minimized through appropriate prevention. Modern treatment methods, in cooperation with a doctor, make it possible to minimize the negative effects of atherosclerosis. Remember—regular check-ups and a healthy lifestyle are the best protection against the development of this cardiovascular disease.