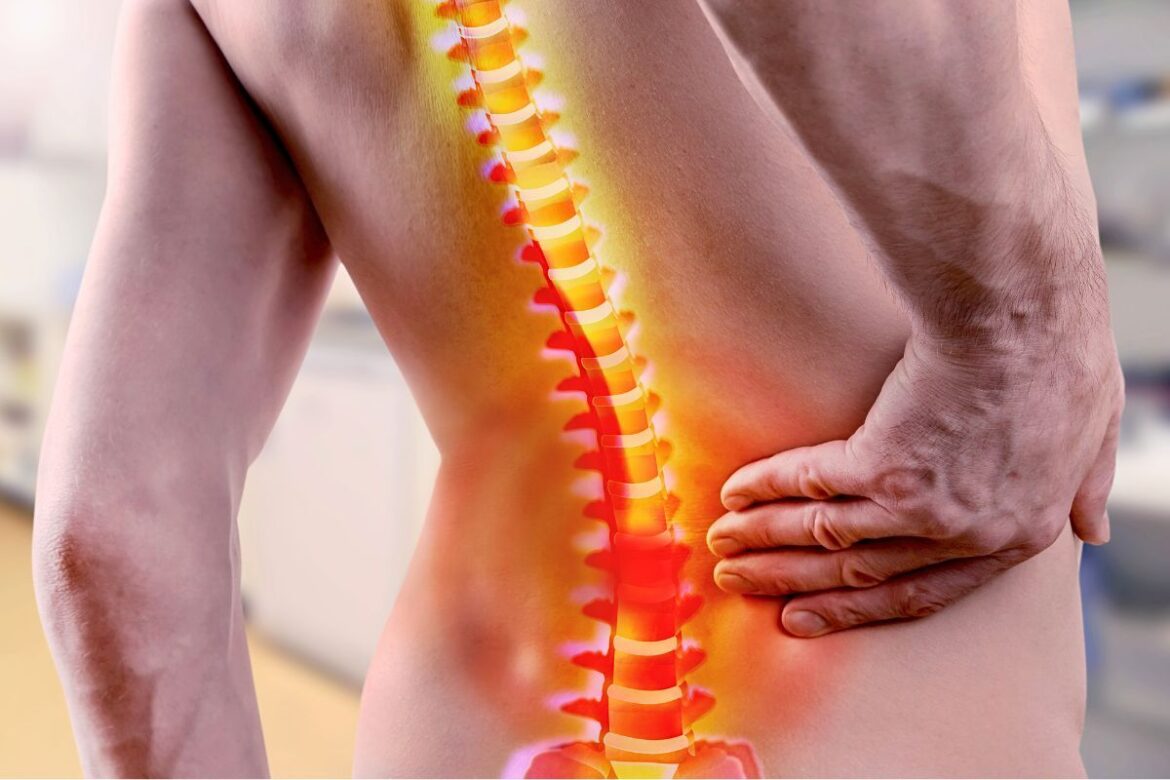
Learn what sciatica is, discover its symptoms and causes, and check out effective methods for treating and preventing spinal pain.
Table of Contents
- What is sciatica? Definition and basic information
- Most common symptoms of sciatica
- Main causes of sciatica development
- Diagnosis of sciatica – how to recognize the condition?
- Modern methods of treating sciatica
- Prevention and ways to avoid recurrence of pain
What is sciatica? Definition and basic information
Sciatica, also known as ischialgia or sciatic nerve neuralgia, is a condition caused by irritation or compression of the sciatic nerve – the largest and longest nerve in the human body, running from the lower spine through the buttocks and down the back of the thigh to the feet. This ailment manifests as severe, radiating pain, usually starting in the lumbar area and radiating down through the buttock to the back of the thigh, calf, and often even the foot. Medically, sciatica is not a disease in itself, but a set of symptoms most often caused by compression or damage to nerve roots in the lower spine (typically L4-L5 or L5-S1). The most common causes of nerve compression are discopathy, herniated nucleus pulposus, spinal canal stenosis, spondylosis, or degenerative changes in the spine resulting in mechanical pressure on the nerves. Sometimes sciatica is triggered by injuries, inflammation, tumors, infections, or anatomical abnormalities. Interestingly, sciatica symptoms may occur suddenly due to acute overstrain, or develop gradually over a longer period as a result of chronic unfavorable loads or micro-injuries.
In practice, sciatica involves not only sudden, stabbing pain, but also a range of other symptoms, which can significantly hinder daily functioning. The pain often intensifies during movement, bending over, coughing, sneezing, or even when changing body position – therefore, many people avoid physical activity, paradoxically delaying recovery. Besides pain, patients may experience numbness, tingling, burning, or muscle weakness in the leg innervated by the sciatic nerve. These symptoms can lead to restricted mobility, difficulty walking, and in severe cases, even sensory disorders or neurological symptoms such as paresis of the lower limb. Sciatica is common among both working-age and older people, and its occurrence significantly reduces quality of life, work efficiency, and overall physical capability. From a diagnosis and treatment perspective, early identification of the pain’s cause and implementation of appropriate therapy is crucial in order to avoid chronicity. It is also worth highlighting that sciatica is often mistakenly equated solely with lower back pain, but its specific course – including buttock, leg, and foot – distinguishes it from other lower back pain syndromes. For many who suffer from sciatica, rapid intervention is key, including not just medication, but also rehabilitation, lifestyle modification, and preventative exercises, which can help prevent recurrence and improve overall spinal fitness.
Most common symptoms of sciatica
The characteristic symptoms of sciatica usually begin with sudden, very severe pain radiating from the lumbosacral region down through the buttock, along the back of the thigh, and often even into the lower leg or foot. This pain is often described as stabbing, burning, or piercing, and its intensity may be so great that it hinders movement, forcing the patient to assume specific, load-relieving body positions. Also typical is the so-called Lasegue’s sign – an increase in pain when straightening the knee while lying on the back, a test doctors use for diagnosis. Sciatica very frequently develops unilaterally, though bilateral presentations do occur. Along with pain, other neurological symptoms such as numbness, tingling (described as “electricity,” “pins and needles”) or sensory disturbances follow the sciatic nerve’s path. Patients often also report a sensation of “numbness” of the skin, burning, or sometimes even difficulty with precise foot movement. Weakness in leg muscle strength may manifest as difficulty walking on the toes or heels, and in more severe cases can lead to foot drop. All this significantly limits movement – many sufferers have trouble walking, sitting down, or performing simple daily tasks such as getting out of bed or bending down. Pain particularly intensifies with coughing, sneezing, laughing, and during prolonged sitting or standing. These symptoms can last from several days to several weeks, but without effective treatment can become chronic, negatively influencing the patient’s quality of life and psychological well-being.
One of the most bothersome aspects of sciatica is the variability and recurring nature of its symptoms. Pain and accompanying signs can fluctuate at different times of day, sometimes lessening when lying down and resting, but becoming worse with every attempt at physical activity. In many cases, a feeling of stiffness in the lower back and limited spine mobility appears, making bending or straightening the torso difficult. Besides sensory and motor disturbances, sometimes autonomic signs are noted, such as sweating disorders, sensations of cold or warmth in the leg, and in rare, advanced cases – loss of bladder or bowel control, which require urgent medical consultation. Sciatica symptoms can begin suddenly, often after strain, abrupt movement, or lifting a heavy object, but can also emerge gradually over days or weeks, with varying pain intensities. Often, only minor lumbar discomfort appears first, which then evolves into clear, radiating pain and other sensory disturbances. Defensive muscle reaction may also occur – a strong spasm of paraspinal muscles further intensifies pain and restricts movement. Symptom intensity and course may be highly individual – for some, the pain is constant and very severe, while others experience it intermittently, e.g., only when performing certain tasks. Not all sufferers need to experience every symptom described – their range and intensity depend on the degree of nerve compression or damage, and how long the illness has persisted.
Main causes of sciatica development
Sciatica is a set of pain symptoms most often due to mechanical compression or irritation of the sciatic nerve or its roots in the lumbosacral region of the spine. The most significant and common cause is discopathy, that is, degenerative changes in the intervertebral discs. Degenerative processes cause ruptures in the annulus fibrosus and displacement of the nucleus pulposus outside its anatomical area (herniated disc), possibly resulting in direct nerve root compression. Such disc displacement – most often at L4/L5 or L5/S1 level – causes severe pain radiating along the lower limb. In addition to disc herniation, degenerative changes in the spine are equally important causes, associated with the natural process of aging. Lower elasticity of bone and ligament structures, osteophyte formation (bone spurs), narrowing of the spinal canal, as well as thickening of ligaments can all result in narrowing of intervertebral foramina through which the nerve roots exit. Under such conditions, even slight movement or effort can increase compression and trigger sciatica symptoms.
Mechanical injuries, overstrain, micro-traumas, and inflammatory states involving structures surrounding the sciatic nerve are also very important. Sciatica can develop after falls, sudden torso twists, or improper heavy lifting, especially in people doing physical work or athletes. In some cases, sciatica develops due to the piriformis syndrome, when a tight or enlarged piriformis muscle compresses the sciatic nerve underneath it, causing characteristic pain. Other causes include posture defects, scoliosis, overweight, or a sedentary lifestyle, all of which lead to chronic strains and micro-injuries of the lumbar spine. Less frequently, sciatica arises from spinal or spinal cord tumors, infections affecting the nervous system, or in the course of metabolic diseases such as diabetes, which can damage neural structures. In addition to strictly anatomical and mechanical factors, genetic predisposition and improper lifestyle – e.g., physical inactivity, smoking, chronic stress causing muscle tension – may increase susceptibility to sciatica. The complexity of mechanisms leading to this condition means that proper diagnosis requires not only symptom analysis but also individual assessment of risk factors and thorough imaging and laboratory tests, enabling clinicians to distinguish sciatica from other causes of lower spine and lower limb pain.
Diagnosis of sciatica – how to recognize the condition?
Diagnosing sciatica requires a detailed and holistic evaluation of the patient’s health, since the symptoms can resemble other neurological or orthopedic conditions. The process begins with a thorough medical interview. The specialist asks about the nature of the pain (e.g., radiating, stabbing, worsened by movement, changes in posture, or coughing), its duration, course, and history of previous spine injuries. It is also crucial to identify risk factors, such as occupation and lifestyle, as well as coexisting chronic diseases predisposing to sciatica. Next, the doctor performs a physical exam, focusing on neurological symptoms typical of sciatica, such as numbness, tingling, muscle weakness, or reflex disorders. Key diagnostic tools include provocative tests, especially the Lasegue’s sign, which involves passively raising the straightened leg – severe radiating pain during this maneuver often indicates sciatic nerve irritation. The doctor also assesses muscle tone symmetry, hip and knee range of motion, and other lower limb abnormalities that may suggest nerve root compression. Neurological symptoms outside the spine are also examined to differentiate conditions imitating sciatica, such as peripheral neuropathy, hip arthritis, or compression syndromes in the buttock region.
When symptoms are atypical, chronic, or severe, imaging is recommended to confirm the diagnosis and rule out other pathologies. The main method is lumbar spine magnetic resonance imaging (MRI), which allows for a very precise assessment of nervous structures and identification of changes in the intervertebral discs, disc herniations, canal stenosis, and degenerative changes. MRI is especially recommended when serious nerve injury is suspected, no improvement occurs with conservative treatment, or alarming symptoms arise – e.g., perineal sensory disturbances, urinary or fecal incontinence, which may indicate cauda equina syndrome requiring urgent intervention. In limited situations or MRI contraindications, computed tomography (CT) is performed to better visualize bone structures. Additionally, X-rays are used, particularly to assess general spine condition and detect degenerative changes, fractures, or congenital defects. In certain cases, electrophysiological studies, such as electromyography (EMG) and electroneurography, provide precise information about nerve conduction and confirm whether the sciatic nerve is involved. Basic laboratory tests – especially in suspected inflammation or infection – are also performed, assessing morphology, ESR, CRP, and other infection markers. Differentiating sciatica from other diseases, such as hip joint disorders, abdominal aortic aneurysm, tumors, or spinal infections, is also crucial, as incorrectly identifying the source of pain can delay and derail treatment. A comprehensive diagnostic algorithm, based on a detailed interview, clinical examination, modern imaging, and additional tests, allows for an accurate diagnosis and implementation of treatment tailored to the patient’s individual needs.
Modern methods of treating sciatica
Modern sciatica treatment methods focus on an individualized approach, utilizing advanced diagnostics and therapies tailored to the clinical presentation and underlying cause. At the first stage, drug therapy is usually implemented according to symptom severity, increasingly using modern nonsteroidal medications with high pain-relief effectiveness and preparations acting directly on neural conduction. In cases of acute pain and severe neurological symptoms, doctors may use nerve root blocks with steroids or anesthetic agents, precisely administered under ultrasound or fluoroscopic guidance. This quickly reduces inflammation and provides pain relief without high doses of oral medication, thus minimizing risks of side effects. Biologic preparations regulating nerve repair processes have also gained popularity, especially for chronic pain syndromes. Rehabilitation based on advanced physiotherapy methods – such as manual therapy, neuromobilization, or individually selected stabilizing exercises – is key to combating chronic pain and improving movement. Physical treatments such as deep magnetic field, high-power laser therapy, TENS electrostimulation, and ultrasound therapy have also shown significant effectiveness, accelerating tissue healing and alleviating pain by affecting nerve conduction and decreasing muscle tension. In recent years, more treatment centers have begun offering minimally invasive procedures, enabling rapid return to activity and shorter recovery time.
Among innovative surgical procedures, microdiscectomy and endoscopic discectomy are especially significant, enabling precise removal of herniated disc fragments compressing the sciatic nerve with minimal disruption to surrounding tissues. These procedures are performed under local anesthesia or short sedation, with patients often able to begin rehabilitation and return to normal activity within hours of surgery. Percutaneous techniques – such as nucleoplasty or hydrodiscectomy – offer a modern alternative to traditional operations, reducing the volume of the disc nucleus and nerve root pressure through a small skin incision. Specialized clinics also employ radiofrequency ablation and cryotherapy, targeting damaged nerve structures without affecting healthy tissues and without lengthy hospital stays. Modern approaches to sciatica go beyond classic medical interventions – increasingly using stem cell therapy and platelet-rich plasma (PRP), accelerating nerve fiber regeneration and rebuilding spinal tissues. Patient education and modern prevention-rehabilitation programs, utilizing mobile apps, telemedicine, or virtual reality to monitor treatment and promote self-exercises at home, also play an invaluable role. Such comprehensive, individualized actions effectively eliminate sciatica symptoms, shorten their duration, and minimize recurrence risk, while ensuring patients’ quality of life and ability to function actively in society.
Prevention and ways to avoid recurrence of pain
Preventing sciatica and effectively avoiding recurrence of spinal pain require a holistic approach, combining physical activity, ergonomics, and overall health maintenance. One of the most essential pillars of prevention is regular and properly chosen physical activity. Strengthening exercises for the core muscles, especially those stabilizing the lumbar spine, can significantly reduce the risk of future pain episodes. Pilates, yoga, and core stabilization training are particularly recommended, as they improve posture control, balance, and muscular flexibility – all of which directly reduce spinal overload. Stretching leg muscle groups, especially the piriformis muscle, is also important, as it frequently irritates the sciatic nerve. Strengthening the gluteal and thigh muscles contributes to even distribution of load on the hip joints and lower spine during daily activities. From a preventive viewpoint, maintaining a healthy weight is likewise important. Overweight and obesity not only burden the spine but also foster chronic inflammation in the body, exacerbating recurring pain. Thus, a healthy, balanced diet rich in anti-inflammatory components (omega-3 fatty acids, B vitamins, magnesium) is advised. Proper hydration is beneficial for the elasticity and nutrition of the intervertebral discs, whose dehydration and degeneration are frequent causes of sciatica. Another vital component of prevention is attention to ergonomics at work and home. Prolonged single-position sitting substantially increases the risk of lower back overload. One should ensure correct chair and desk height, use lumbar supports, and take regular breaks to stretch and change body position. Experts recommend not sitting continuously for longer than 45–60 minutes. When lifting heavy objects, use proper technique (bending at the knees, keeping the back as straight as possible). Movements requiring trunk rotation should be minimized, and all physical activities performed in moderation, gradually increasing intensity. The right bed and mattress, which provide adequate spinal support at night – not too soft or too hard – are equally important.
Effective sciatica prevention and recurrence avoidance also involves responding to the body’s early warning signals. Regular self-observation and swift initiation of appropriate actions at the first sign of discomfort, such as pain or tingling, can prevent full-blown sciatica attacks. Chronic stress should not be ignored, as it worsens muscle tension and may intensify pain symptoms. Relaxation techniques, like breathing exercises, meditation, or massage, are recommended for chronic spinal conditions. Regular consultations with professional physiotherapists help assess body posture, joint mobility, and movement habits, and if necessary, provide personalized exercise programs. Patient education on spinal health, teaching correct sitting, standing, lifting, and sleeping positions, is also good practice. Physically active or athletic individuals should pay close attention to regular stretching and warm-ups and avoid overburdening the spine via dynamic or improperly loaded movements. In case of recurring symptoms or new spinal complaints, prompt consultation with a doctor or therapist is crucial – delayed treatment increases chronicity and reduces therapy effectiveness. Prevention should also include limiting risk factors like smoking, excessive alcohol consumption, and neglecting management of chronic diseases that may worsen spinal conditions. By following these principles, one can both minimize sciatica recurrence risk and keep the spine in good condition for years, even with existing degenerative disorders or after previous pain episodes.
Summary
Sciatica is a condition that significantly affects quality of life, presenting as acute pain from the lower back down the leg. This article has covered how to recognize its first symptoms, the main causes, and which diagnostic methods enable swift treatment. Thanks to modern therapy solutions – such as physiotherapy, pharmacological treatments, or rehabilitation – a return to full fitness is possible. Take care to use regular prevention to minimize risk of recurrence. Rapid response and proper medical care are the keys to effectively overcoming sciatica and improving daily comfort.