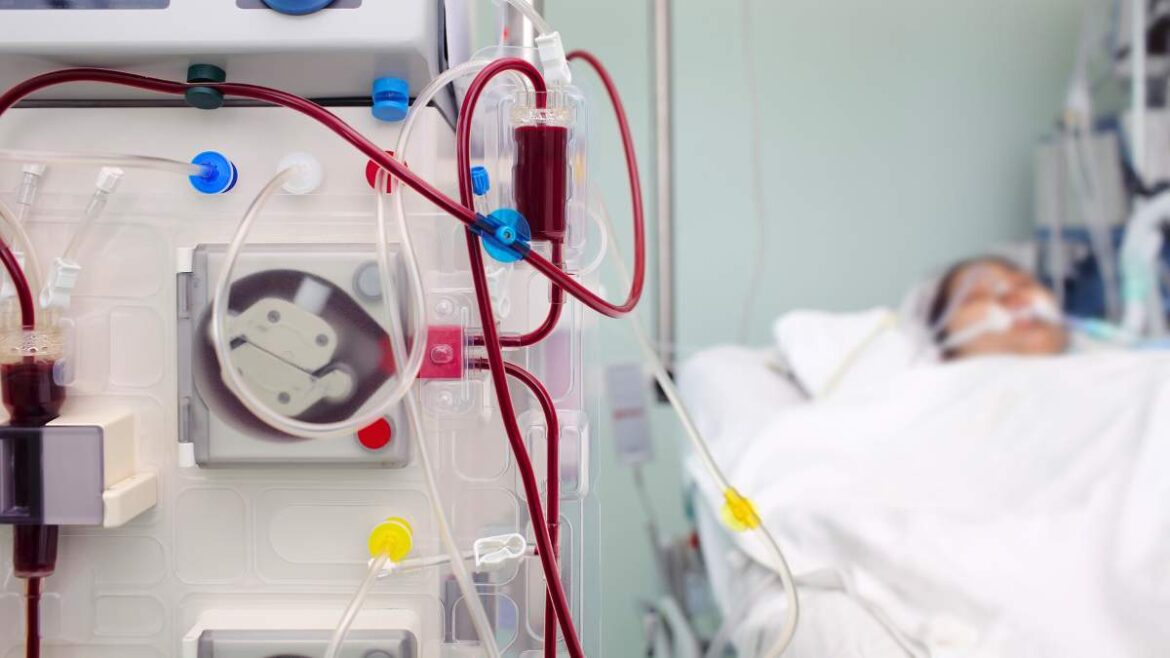
Find out what kidney dialysis is, when it is necessary, how it’s performed, its potential side effects, and what life is like for dialysis patients.
Table of Contents
- Kidney Dialysis – What Is It and When Is It Used?
- Types of Dialysis: Hemodialysis and Peritoneal Dialysis
- The Dialysis Procedure – Step by Step
- Cost and Availability of Dialysis in Poland
- Side Effects of Dialysis and Possible Complications
- Living with Dialysis – Tips and Support for Patients
Kidney Dialysis – What Is It and When Is It Used?
Kidney dialysis is an advanced medical procedure designed to replace the functions of damaged or failing kidneys. These organs are responsible for removing metabolic waste, regulating fluid and electrolyte balance, and maintaining acid–base equilibrium in the body. When the kidneys can no longer function properly, toxic waste and excess fluids accumulate, resulting in serious, life-threatening disorders. At this point, dialysis becomes not just a form of treatment but an essential measure to maintain basic life functions. There are two main types of dialysis: hemodialysis (extracorporeal dialysis, where blood is cleaned by a special machine—an “artificial kidney”) and peritoneal dialysis (which occurs within the body using the peritoneal membrane as a natural filter). The choice of method depends on the patient’s overall health, coexisting conditions, lifestyle preferences, and the severity and progression of kidney failure.
Dialysis becomes essential when chronic kidney disease (CKD) reaches the end stage, known as uremia, and the natural excretory and regulatory functions of the kidneys are severely impaired. Doctors decide to start dialysis based on detailed laboratory tests, evaluation of parameters such as glomerular filtration rate (GFR), creatinine, or blood urea levels, and clinical symptoms like swelling, hypertension, nausea, chronic fatigue, electrolyte imbalances, or breathing difficulties. Besides chronic kidney failure, dialysis may also be used in acute kidney failure caused by sudden damage due to infection, drug or chemical poisoning, severe injury, post-surgical complications, or other conditions quickly deteriorating renal filtration. In emergencies, a single dialysis session can rapidly remove toxins or restore electrolyte balance, while in chronic cases, regular sessions are necessary—often for life or until a kidney transplant is done. Dialysis thus acts as a “bridge” supporting life and preparing patients for further treatment, including transplantation. However, dialysis is not a cure that restores the kidneys’ original functioning; instead, it controls symptoms, prevents complications, and aims to improve comfort and life expectancy for those affected.
Types of Dialysis: Hemodialysis and Peritoneal Dialysis
Kidney dialysis comprises two primary replacement treatments: hemodialysis and peritoneal dialysis. Both aim to cleanse the blood of toxins, metabolic byproducts, and excess fluids but differ in procedure, equipment needed, and their impact on everyday life. Hemodialysis is the most common form and involves passing the patient’s blood through a special filter in an external device known as the “artificial kidney” (dialyzer). This requires creating a safe, permanent vascular access—typically an arteriovenous (AV) fistula (connecting an artery to a vein in the forearm) or, when not possible, a catheter inserted in a large vein. Blood is drawn out, filtered in the dialyzer, and then returned to circulation. Each session lasts 3–5 hours, usually three times a week at specialized dialysis centers, or rarely, at home. Sessions are closely monitored by medical staff, necessitating regular visits or proper training for home dialysis. Hemodialysis results in the rapid and effective removal of toxins, reduction of swelling, and quality-of-life improvements. However, it involves a strict schedule, dietary and fluid restrictions, and risks such as vascular access infections, thrombosis of the fistula, and drops in blood pressure during treatment.
An alternative is peritoneal dialysis, which uses the natural membrane lining the abdominal cavity (peritoneum) as a semi-permeable filter. This requires the surgical placement of a permanent catheter into the peritoneal cavity. Special dialysis fluid is introduced via the catheter, stays in the abdomen for several hours, during which wastes and excess water pass through the peritoneum into the fluid, and is then drained and replaced. There are two main methods: continuous ambulatory peritoneal dialysis (CAPD), where exchanges are done manually several times daily, and automated peritoneal dialysis (APD), performed overnight with a special machine called a cycler. This offers greater flexibility, supports independence, and improves the comfort of those wishing to continue work or education. Peritoneal dialysis does not require frequent visits to a medical center, but patients must be well-trained in hygiene, fluid exchange procedures, and monitoring for complications, mainly peritonitis (abdominal infection) or catheter issues. The choice of dialysis method depends on patient age, comorbidities, lifestyle, technical feasibility, and patient and family preference. Some may use one method for years, while others switch as their health and needs change. Both require systematic monitoring of residual kidney function, regular lab tests, and close cooperation with nephrology teams to minimize complications and maximize therapy effectiveness. Regardless of the method, dialysis is a long-term process that fundamentally changes the patient’s routine and demands active involvement in managing health, self-discipline, and adherence to medical and dietary guidelines.

The Dialysis Procedure – Step by Step
Despite being life-saving, kidney dialysis is a multi-stage process that requires strict adherence to procedures by both medical staff and the patient. In hemodialysis, prior to each session, the patient’s general condition is assessed—vital signs such as blood pressure, heart rate, temperature, and body weight are measured to determine the amount of fluid to be removed. The nurse or doctor then prepares vascular access—usually an AV fistula or catheter—through which blood leaves the body for cleaning in the “artificial kidney” (dialyzer) containing a semi-permeable membrane that removes toxins, excess fluids, and metabolic waste. Procedure parameters—blood flow rate, type and composition of dialysate, session duration—are set. Throughout, the patient lies semi-reclined or flat on a special dialysis chair, while staff monitor their condition, responding to issues such as muscle cramps, low blood pressure, or hypovolemia. Sessions last 3–5 hours, depending on individual needs. Afterward, needles or the catheter are removed, with the site dressed to prevent bleeding and infection. The patient’s vital parameters are rechecked, followed by a short observation period, and they receive dietary, fluid, and medication guidance if needed.
Peritoneal dialysis (both CAPD and APD) follows a different, but also multi-step process requiring patient engagement. It starts with surgical placement of a permanent peritoneal catheter. Home peritoneal dialysis begins with careful hand washing and disinfecting the catheter area to reduce infection risk. The patient connects a dialysis fluid bag to the catheter, allowing the fluid into the peritoneal cavity (“inflow”). The fluid remains in the abdomen for several hours (the exchange time), during which waste and excess fluids cross the peritoneal membrane into the fluid. The used fluid is then drained to a separate bag, and the procedure is repeated as advised (typically 4–5 exchanges daily with CAPD or automatically at night with APD). Maintaining sterility, monitoring the skin around the catheter, and watching for complications—like abdominal pain, fever, or cloudy effluent—are all crucial. Peritoneal dialysis is less invasive than hemodialysis and enables active patient participation at home, but demands regularity, precision, and nephrologist follow-up. Regardless of method, dialysis routines are closely monitored and tailored to the patient’s needs and disease stage. Close cooperation with the dialysis team and adherence to medical advice are key to safety and effectiveness, as well as preventing complications during long-term therapy.
Cost and Availability of Dialysis in Poland
Kidney dialysis is a life-saving procedure, with its funding and accessibility being crucial issues for patients, their families, and Poland’s entire healthcare system. Dialysis-related costs involve not only the direct price of treatments but also associated expenses and logistical support. In Poland, most dialysis patients are cared for in the public health system, so both hemodialysis and peritoneal dialysis treatments are fully reimbursed by the National Health Fund (NFZ). Practically, the patient bears no direct cost for regular dialyses performed in centers, regardless of method or frequency. Reimbursement additionally covers other medical services: nephrologist visits, monitoring tests, transport to dialysis centers, and essential medications for chronic kidney failure. However, patients and families often incur travel expenses, need to reorganize working hours, and may need home care—especially for elderly or bedridden individuals. Medical transport for those unable to reach dialysis centers independently is still insufficient in some regions, raising out-of-pocket costs for patients, especially in rural or small-town areas where access to specialized centers is limited. Additionally, starting dialysis usually means a specialized therapeutic diet, which may entail extra spending on special food items or supplements. For peritoneal dialysis conducted at home, under nephrologist supervision, patients need regular supplies of dialysis kits and hygienic materials—these too are reimbursed by the NFZ. However, organizing a hygienic and safe home environment may require investment in equipment or furnishings, which are typically not covered by reimbursement and become the patient’s responsibility.
Dialysis availability in Poland is generally high compared to other Central/Eastern European countries, but still varies by region and type. Most dialysis centers are in larger cities and industrial or voivodeship regions, offering both hemodialysis and peritoneal dialysis. These centers are modern, highly specialized, and work closely with hospital nephrology departments. Availability remains challenging in smaller towns and rural areas, forcing some patients into lengthy commutes multiple times a week. The NFZ tries to mitigate disparities through regulations on dialysis seat numbers relative to the population and by funding new centers in deficit regions, but in practice, not all patient needs are met. Peritoneal dialysis is becoming more available and popular as it doesn’t require regular visits to a medical center, with advanced training and nephrology support enabling many to self-treat at home, reducing strain on the system. However, not all regions equally provide training teams and home support, strongly affecting treatment method choice. Qualification and method selection depend not only on medical indications but logistical, family, and household factors, as treatment requires reorganizing family and work life. Both the standards and availability of dialysis are rising yearly, but shortages of nephrologists, trained nurses, and technical infrastructure remain challenges, especially given the growing prevalence of chronic kidney disease. For patients planning trips, it’s possible to temporarily transfer treatment to other centers, provided arrangements are made in advance. Additionally, Polish patients have access to innovative therapies and psychological/social support, funded largely by public sources and NGOs. All these aspects impact dialysis accessibility and the overall quality of life for those with chronic renal failure.
Side Effects of Dialysis and Possible Complications
While kidney dialysis saves lives and allows people with kidney failure to function, it is associated with many potential side effects and complications, both short- and long-term. In hemodialysis, the most common unwanted effects include post-treatment fatigue, low blood pressure, muscle cramps, nausea, and headaches. Episodes of hypotension—abrupt blood pressure drops during or immediately after sessions—are especially frequent, usually due to excessive fluid removal or electrolyte disturbances. Chronic hemodialysis also leads to increasing anemia (from erythropoietin deficiency), mineral and bone disorders associated with abnormal calcium-phosphate metabolism, and a higher risk of cardiovascular diseases. Persistent vascular access and catheter use may result in thrombosis, access site infections, and aneurysm formation. These infections—especially sepsis—pose a serious life-threatening risk, often needing hospitalization and intensive therapy. Long-term exposure to the dialyzer may also prompt chronic allergic reactions, itching, immune dysfunction, inflammation, or, more rarely, so-called dialysis amyloidosis, where protein deposits accumulate in joint tissues, causing pain and movement difficulties.
Peritoneal dialysis, while providing more flexibility for patients, comes with its own set of complications. The most serious is peritonitis (infection of the abdominal membrane), resulting from contamination during fluid changes. It typically presents as abdominal pain, fever, cloudy dialysate, and malaise. Antibiotic therapy generally resolves these infections, but repeated episodes can cause adhesions, chronic inflammation, or require stopping peritoneal dialysis entirely. Risk is higher in those failing to maintain hygiene or struggling with catheter management. Other side effects include catheter infections, dialysate leakage into subcutaneous tissues, bleeding, hernias, weight gain, and metabolic problems due to glucose absorption from dialysates. Both methods can also cause nutritional disorders, vitamin deficiencies, and chronic low-grade inflammation, leading to reduced exercise tolerance, compromised immunity, and a higher cancer risk. Long-term dialysis negatively affects emotional health—persistent side effects, lifestyle limitations, and chronic stress may trigger depression and lower treatment motivation. Some complications, especially cardiovascular, remain leading causes of mortality among dialysis patients, including left ventricle hypertrophy, atherosclerosis, and thromboembolic events. Timely detection and response to side effects, as well as close cooperation with nephrology teams and patient education, are vital to minimize risks and improve quality of life on dialysis therapy.
Living with Dialysis – Tips and Support for Patients
Starting dialysis therapy is a turning point, bringing many physical and mental challenges. Adapting daily life to the dialysis schedule requires reorganizing work, family, and social routines. Key to accepting new realities is education—understanding how dialysis works, proper hygiene (especially for home peritoneal dialysis), early recognition of complications, and following dietary advice. Patients should work closely with their nephrologist, dialysis nurses, and clinical nutritionist to adjust their diet; restrictions often apply to fluids, sodium, potassium, phosphorus, and protein. Maintaining physical activity as tolerated and establishing a regular sleep pattern benefit well-being and physical fitness. Support from medical staff, participating in peer support groups, and exchanging experiences help patients handle daily difficulties. Many hospitals and patient organizations offer psychological or therapeutic counseling to help reduce depression risk and cope with frustration or anxiety. Open communication with family about emotional needs lays the foundation for support during tough times. Setting up a comfortable and hygienic home environment for treatments, organizing entertainment (books, music, movies) during dialysis helps reduce treatment-related stress.
Planning each day around dialysis requires flexibility and assertiveness, especially in work or social life. It is worth discussing health needs and possible work hour adjustments with employers. Polish labor law protects chronically ill individuals, enabling flexible work schedules or disability allowances, especially regarding transport to dialysis and post-session recovery. Patients should also stay safe—not drive shortly after treatment and inform relatives or caregivers about their well-being. In crises, such as sudden health deterioration, prompt contact with the hospital or dialysis team is crucial. Patients’ rights include being informed, raising concerns, choosing a treatment center, and actively participating in care. Free educational materials, kidney health apps, and consultations with pharmacists can help manage the auxiliary medications used in chronic kidney failure. Being responsible about treatment and using available social, financial, or psychological support lets patients adapt to their new reality, reduce social exclusion, and maintain the highest possible quality of life despite the limitations of dialysis therapy.
Summary
Kidney dialysis is a key method for treating kidney failure, saving the lives of people with serious kidney diseases. This article explained what dialysis is, when and why it is used, and discussed the main types: hemodialysis and peritoneal dialysis. Step by step, we described the procedure, outlined the costs and availability of this therapy in Poland, and presented possible side effects and complications. We also addressed daily life with dialysis, presenting guidance and support options for patients. Understanding this process better prepares individuals for therapy and enables informed care, improving quality of life despite illness.