Discover the causes, symptoms, and effective treatment methods for varicose veins in the legs. Learn how to recognize varicose veins and what to do to prevent their progression.
Table of Contents
- What are varicose veins and why do they develop?
- Main causes of lower limb varicose vein development
- Most common symptoms of varicose veins – how to recognize them?
- Treatment methods for varicose veins – from home remedies to procedures
- Prevention and daily habits that support healthy veins
- Complications of untreated varicose veins – what to watch out for?
What are varicose veins and why do they develop?
Varicose veins in the legs are one of the most common venous system diseases, affecting both women and men, although women are significantly more prone to their formation due to hormonal factors and pregnancy. In practice, varicose veins manifest as enlarged, elongated, and twisted veins running just under the skin’s surface, most often on the calves and thighs. Their color is often bluish-violet, and the structure is distinctly raised above skin level, creating not just a cosmetic problem but, above all, a health issue. The root cause of varicose veins is chronic venous insufficiency—a condition in which blood, instead of flowing freely from the lower limbs toward the heart, accumulates in superficial veins, causing them to dilate inappropriately and increasing venous pressure. This process is most often caused by damage or weakening of the venous valves that, in healthy vessels, prevent the blood from flowing backward due to gravity and blood pressure. When the valves stop functioning properly, blood stasis and backward flow (venous reflux) occur, ultimately deforming and enlarging the walls of superficial veins. Varicose veins are not just a cosmetic defect—they indicate more serious blood flow disorders that carry the risk of complications such as phlebitis, thrombosis, or venous ulcers.
In the pathogenesis of varicose veins, genetic factors and many lifestyle-, health-, and physiology-related risk factors play a significant role. There is a documented family predisposition to chronic venous insufficiency—if varicose veins were present in parents or grandparents, the likelihood of their occurrence in subsequent generations increases significantly. However, other factors also influence the development of the condition, such as a sedentary or standing work style, low physical activity, prolonged sitting with crossed legs, overweight and obesity, as well as periods of increased venous load during pregnancy. Increased intra-abdominal pressure, which is common in pregnant women, encourages the dilation of veins and impairs venous return from the legs. Additionally, the female hormonal system (especially changes related to pregnancy or hormonal contraception) can further weaken vein walls and promote valve loosening. Long-term immobility, such as after surgeries or due to severe illnesses, also lowers the efficiency of the muscle pump in the legs, which hinders venous return. It is worth mentioning that people who regularly wear clothing that is too tight or high-heeled shoes face added challenges to proper blood flow in the veins. Nowadays, particular attention is paid to an unhealthy lifestyle: a diet low in fiber, excessive salt, and also smoking not only indirectly affect the course of chronic venous insufficiency but also increase the risk of advanced varicose vein changes. In summary, varicose veins are the result of the complex interplay of genetic, hormonal, and environmental factors, and understanding their etiology allows for better prevention and conscious approaches to treating and limiting the effects of this troublesome disease.
Main causes of lower limb varicose vein development
Varicose veins of the lower limbs are a complex health problem resulting from a combination of genetic, environmental, and lifestyle-related factors of modern people. The main cause of varicose veins development is chronic venous insufficiency (CVI), caused by malfunctioning venous valves in the lower limb venous system. Healthy valves act like one-way check valves, enabling blood flow upwards, counteracting gravity. When these valves are damaged or weakened, blood begins to flow backward and stagnate in the veins. This leads to increased venous pressure, vessel wall stretching, and, consequently, the appearance of characteristic dilated, winding veins visible under the skin. Key factors triggering valve insufficiency and vascular wall weakening include genetic predisposition—the risk of varicose veins is significantly higher if the condition is present in the family. Hereditary tendencies often concern the structure of blood vessel walls and valves, making them more susceptible to stretching, damage, or failure under environmental and physiological pressures.
A strong risk factor for varicose vein development is also a sedentary lifestyle and lack of regular physical activity, which promote blood stasis in the veins and weakening of the calf muscles responsible for the so-called muscle pump aiding blood return to the heart. Many hours of sitting or standing work common to many professions (e.g., office workers, hairdressers, salespeople, teachers) result in prolonged venous stasis and increased hydrostatic pressure in the leg vessels, leading to stretching and gradual degeneration of vein and valve walls. Hormonal factors also play an important role—especially in women, particularly during pregnancy, when progesterone production increases, which encourages vessel wall relaxation, and the growing uterus puts pressure on the pelvic and lower limb venous system. Similar effects can be caused by hormonal therapies (e.g., oral contraceptives, hormone replacement therapy). Overweight and obesity are other common causes—excess body fat increases intra-abdominal pressure and greater pressure on the veins, disrupting proper blood circulation in the legs. A diet low in fiber and high in salt may also promote fluid retention in the body and increased swelling, exacerbating pre-existing venous circulation disorders. It is also worth emphasizing the harmful effects of smoking on vascular health—substances in tobacco smoke harm the vascular endothelium, exacerbate inflammation, and impair the elasticity of venous walls. Additionally, varicose veins become more frequent with age—aging processes lead to gradual weakening and damage to tissues, decreasing the effectiveness of anti-backflow mechanisms. Less obvious risk factors include the regular use of tight clothing that impedes free blood flow, frequent wearing of high-heeled shoes, as well as chronic constipation, which causes increased intra-abdominal pressure during straining. In addition, the presence of certain chronic diseases, such as heart or kidney disease, or congenital venous system defects, should be considered. All these factors—on their own or combined—can impair venous efficiency and gradually lead to the development and worsening of lower limb varicose veins.
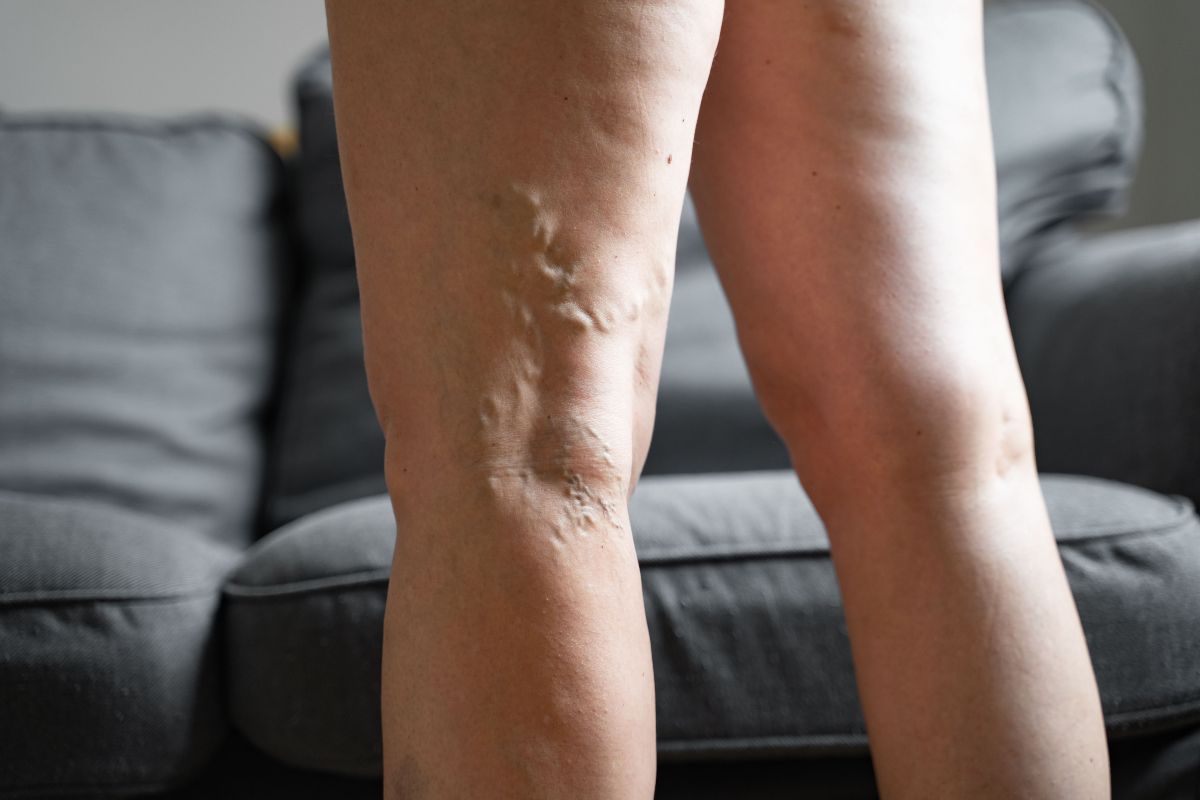
Most common symptoms of varicose veins – how to recognize them?
Recognizing lower-limb varicose veins is extremely important, as quick intervention minimizes the risk of complications and improves quality of life. The symptoms of varicose veins are varied and can manifest both as distinct changes visible on the surface of the skin and as less obvious ailments that signal a problem with the proper functioning of the venous system. The most characteristic and frequently reported symptom are visible, enlarged, bluish-violet or bluish veins, often just beneath the skin on the calves, thighs, or around the ankles. Varicose veins usually appear as twisted, elongated “cords,” and in more advanced stages may form clear, raised nodules. These changes are often accompanied by a feeling of heaviness and fatigue in the legs, particularly after standing or sitting for extended periods, which subsides after rest or leg elevation. Many people also experience a sensation of “fullness” or dull pain, especially at the end of the day, which is the result of increasing blood stasis in the veins of the lower limbs.
Quite often, people suffering from varicose veins report other symptoms that may be ignored or wrongly attributed to general fatigue. The most common are swelling of the lower limbs—initially mild and appearing only at the end of the day, but may worsen and persist throughout the day over time. Other symptoms include itching of the skin on the calves and around varicose veins, sometimes burning or tingling, indicating irritation and slight inflammation of the tissues around the dilated veins. Over time, the skin in the varicose vein area may become thinner, more prone to injuries, and in advanced stages discolorations and trophic changes appear—brown spots or even venous ulcers, which indicate chronic venous insufficiency. Painful muscle cramps in the calves, usually at night or after intense, uneven leg strain, are also frequent. It is worth noting that varicose vein symptoms may intensify in hot weather, during menstruation, or pregnancy due to additional burden and hormonal changes affecting the vascular walls. Symptoms often develop gradually; thus, patients may go years without seeking help, attributing them to lifestyle or age. Early recognition of varicose veins, based on these symptoms, allows you to avoid many complications, such as superficial phlebitis, bleeding from damaged vessels, or irreversible changes in the structure of the skin and subcutaneous tissue.
Treatment methods for varicose veins – from home remedies to procedures
Treatment for lower limb varicose veins includes a wide spectrum of methods—from non-invasive home remedies and pharmacotherapy to modern medical procedures. The choice of therapeutic strategy depends primarily on the stage of the disease, the individual predispositions of the patient, and the presence of additional conditions. In the early stages of varicose veins or for people with mild symptoms, lifestyle changes are often recommended. Home methods include increasing physical activity, such as regular walking, cycling, or swimming, which improve venous circulation and prevent blood stasis in the legs. Avoiding prolonged standing and sitting with legs down, as well as including rest with legs elevated above heart level, is also essential to facilitate blood outflow. It is also recommended to wear special compression stockings, which improve venous return, reduce swelling, and alleviate heaviness in the legs. In addition, it is worth maintaining a proper body weight, a balanced diet rich in fiber, vitamins C and E, and limiting salt intake. Applying cold showers to the legs and massages can provide relief; however, hot baths, sunbathing, and saunas, which promote vein dilation, should be avoided. Herbal supplements containing extracts of horse chestnut, butcher’s broom, or arnica may have mild sealing and anti-edema effects on blood vessel walls, but their effectiveness is mainly confirmed in mild cases. In advanced stages of the disease, when varicose veins become painful, significantly enlarged, or complications occur, phlebological consultation and more advanced methods are necessary.
Modern medicine offers several procedural treatment methods for varicose veins that are increasingly effective and minimize recovery time. The best-known and most traditional surgical method is stripping, involving the removal of the diseased great saphenous vein through small skin incisions, but nowadays less invasive techniques are used more frequently. Sclerotherapy—injection of a special sclerosant substance into the varicose veins—is often used for smaller abnormalities and so-called spider veins. The procedure involves introducing a substance that closes the lumen of the vein, after which the vessel gradually disappears; it is brief, performed on an outpatient basis, and does not require hospitalization. Endovascular methods, such as endovenous laser treatment (EVLT) and radiofrequency ablation (RFA), consist of inserting a fiber or electrode into the diseased vein and heating the vessel wall using laser or radio waves, resulting in closure and degeneration of the insufficient vein. These procedures are particularly effective, performed under local anesthesia, and allow a quick return to daily activities. An alternative is adhesive closure with the VenaSeal method, which introduces a special glue into the vein to close it from within; it does not require compression after the procedure and is very comfortable for the patient. For patients with advanced venous insufficiency, a doctor may also suggest miniphlebectomy—removal of enlarged vein segments through small subcutaneous incisions. The choice of an appropriate treatment method is always based on an individual assessment of health, the extent and location of varicose veins, coexisting diseases, and patient preferences. Patient education and regular specialist follow-up are also extremely important, as varicose veins, especially if untreated or improperly treated, can lead to complications such as chronic ulcers, deep vein thrombosis, or chronic pain and reduced quality of life. Remember, even the most advanced procedural interventions are no substitute for daily prevention, which allows for long-term maintenance of venous health and minimizes the risk of disease recurrence.
Prevention and daily habits that support healthy veins
Proper prevention of leg varicose veins and the development of daily habits play a key role in the prevention of venous diseases. Foremost is regular physical activity, which, by stimulating the muscles of the lower limbs, supports proper blood flow in the veins and decreases the risk of venous stasis. Sports that engage the legs, such as brisk walking, running, cycling, swimming, dancing, or gymnastics, are especially recommended. Even a daily walk, performed regularly, can positively affect vascular wall elasticity and valve performance. However, one should avoid sports that strain joints and veins, such as weightlifting or intensive strength training without appropriate warm-up. The second pillar of prevention is maintaining proper body weight—excess weight and obesity are significant factors that increase venous pressure and burden the circulatory system. Weight control through a proper diet and exercise decreases the risk of developing varicose veins and improves overall fitness.
Maintaining appropriate habits at work and leisure is also important. Those who perform standing or sitting work should regularly change body position, take short breaks to stretch their legs, and avoid crossing their legs, as it impedes venous return. It is also recommended to elevate legs above heart level during rest to facilitate rapid venous emptying and reduce swelling. Proper wardrobe is crucial—wearing loose clothing that does not constrict thighs, waist, or calves and shoes with low, stable heels supports healthy circulation. Compression therapy, i.e., preventive use of specialist compression stockings or knee-highs, may be advisable for people with a tendency to develop varicose veins, those working in standing or sitting positions, as well as pregnant women—such compression aids proper valve function and prevents excessive swelling. Healthy dietary choices are equally important: the diet should be rich in fiber (vegetables, fruits, groats, whole grain products), vitamin C, flavonoids, and antioxidants that strengthen vessel walls and support regeneration. Limiting salt (which causes water retention and swelling) and also simple sugars and trans fats has a positive effect on the circulatory system. Proper hydration improves lymphatic function and helps prevent blood thickening, which is especially important for thrombosis prevention. One should also avoid long hot baths or using the sauna, as high temperatures cause vessel dilation that may exacerbate varicose vein symptoms, and protect legs from injuries and scratches, especially if skin changes are present. Quitting smoking and limiting alcohol consumption are additional core preventive elements—nicotine damages blood vessels, while alcohol promotes dehydration and the weakening of vein walls. Ongoing health monitoring, regular doctor visits, observation of early warning signs (swelling, pain, skin changes), and leg hygiene education significantly increase the chances of keeping veins healthy for many years.
Complications of untreated varicose veins – what to watch out for?
Untreated varicose veins of the lower limbs are not just a cosmetic problem but above all a serious health hazard, leading to numerous, often irreversible complications. Chronic venous insufficiency associated with varicose veins results in persistent blood stasis in the vessels, causing chronic inflammation of the vein walls and nearby tissues. One of the first complications includes pain and chronic swelling, which over time become increasingly troublesome, limiting activity and comfort. Persistent swelling encourages skin changes—discoloration, induration, thinning of the skin, and in the late stage, the development of unhealed venous ulcers. These are some of the most troublesome and difficult to treat complications of varicose veins. Venous ulcers usually form near the inner ankle and are characterized by a prolonged, difficult healing process, susceptibility to bacterial infections, and tendency to recur. Even a small wound at the site of a chronically dilated, poorly oxygenated vein may become the focus of an extensive, painful ulcer that, if untreated, may lead to secondary infections and sometimes even life-threatening septicemia (sepsis).
Another dangerous consequence of untreated varicose veins is the increased risk of clot formation in both superficial and deep veins of the lower limbs. Superficial vein thrombosis (thrombophlebitis) manifests as redness, pain, tenderness, and a palpable hardening of the vein under the skin. Although this is often underestimated, it can lead to a more serious complication—deep vein thrombosis. This, in turn, through detachment of a fragment of the thrombus, can result in pulmonary embolism—a life-threatening condition manifested by sudden shortness of breath, chest pain, or loss of consciousness. Untreated varicose veins also increase the risk of developing chronic venous insufficiency, manifested by permanent skin changes, indurations (lipodermatosclerosis), discoloration, and recurring infections—subcutaneous tissue and skin inflammation (cellulitis), which may require hospitalization. Other dangerous complications include bleeding from varicose veins, particularly those shallowly located under the skin—even a minor trauma can result in heavy, difficult-to-control bleeding from a distended vein, sometimes requiring urgent hospitalization. The clinical picture of untreated venous disease also includes intensified subjective symptoms such as chronic pain, heaviness, numbness of the legs, and worsening sleep quality—all factors that markedly worsen daily functioning and may lead to neglect of other aspects of health. Chronic inflammation in the veins, chronic hypoxia, and swelling also damage nerve fibers, indicating as tingling, itching, and intensified pain. In advanced, untreated stages, there may also be chronic, hard-to-heal wounds, recurring infections, and progressive degradation of the skin and subcutaneous tissues; therefore, quick intervention and specialist treatment are key to preventing these complications.
Summary
Varicose veins in the legs are not just a cosmetic issue but, above all, a health problem. Understanding the causes and symptoms of this disease allows for quick recognition of its first signs and the application of effective—both home and specialist—treatments. Proper prevention and daily habits, such as physical activity or compression therapy, can effectively prevent the development of varicose veins. The symptoms and complications of this disease should not be ignored, as early intervention is key to healthy and light legs. Take care of your veins every day!


