Bacterial skin infections are a common health problem affecting people of all ages. Learn how to recognize, effectively treat, and protect yourself against recurrences with up-to-date medical knowledge.
Find out how to identify and effectively treat bacterial skin infections. Discover symptoms, causes, diagnostics, and home prevention methods!
Table of Contents
- What are bacterial skin infections?
- Most common symptoms of skin infections
- Main causes and risk factors of skin infections
- Effective diagnostics of skin infections
- Modern treatment methods and home remedies
- How to prevent bacterial skin infections?
What are bacterial skin infections?
Bacterial skin infections are a group of conditions caused by various species of bacteria that penetrate the epidermis, dermis, or deeper tissues and begin to multiply, resulting in inflammation. Under normal conditions, the skin serves as a natural protective barrier against microorganisms, and its surface hosts the so-called physiological bacterial flora, which not only is harmless, but actually helps protect the body from pathogenic bacteria. Infection usually occurs when this barrier is compromised—such as from a cut, abrasion, insect bite, burn, scratch, improper squeezing of acne lesions, or even from vigorous scratching of itchy skin. In such situations, pathogenic bacteria—most commonly staphylococci (Staphylococcus aureus, including MRSA strains resistant to methicillin) and streptococci (mainly Streptococcus pyogenes)—take advantage of the “open gate” and rapidly multiply. Bacterial skin infections encompass a wide spectrum, ranging from relatively superficial and mild conditions like impetigo or folliculitis to deep, potentially life-threatening states such as abscesses or necrotizing fasciitis. The common feature of these disorders is the presence of inflammation, typically manifesting as redness, warmth, swelling, pain, and sometimes purulent discharge. Unlike viral or fungal infections, bacterial skin infections usually have a rapid, dynamic course—skin changes may enlarge from day to day, become more painful, with the appearance of pus-filled blisters, yellowish crusts, or weeping ulcers. Importantly, these infections can affect individuals of any age—from newborns and young children to adults and seniors—although people with weakened immunity, diabetes, obesity, chronic diseases, or those who have undergone surgery, dialysis, or invasive medical procedures are particularly at risk. It is crucial to understand that a bacterial skin infection is not always limited to the skin itself—in some cases, bacteria may penetrate deeper, reaching the subcutaneous tissue, muscles, or even the bloodstream, leading to sepsis, a generalized inflammatory response. For this reason, ignoring even seemingly minor purulent lesions and picking at them can have serious health consequences.
From a medical perspective, bacterial skin infections are classified according to the depth and extent of lesions, as well as the involvement of skin appendages such as hair follicles, sebaceous, or sweat glands. Superficial infections include, among others, impetigo (common in children, manifesting with honey-yellow crusts around the mouth and nose), folliculitis (small pustules around hair follicles), or paronychia (purulent inflammation of the nail folds). Deeper infections include boils and carbuncles, abscesses, and also psoriasis and cellulitis, where the inflammatory process affects the subcutaneous tissue and often spreads along lymphatic vessels. In clinical practice, it is also important to distinguish typically cutaneous infections from those that originate in other organs but manifest with skin changes—an example could be disseminated skin abscesses in bacteremic patients. Although the usual cause is contact with pathogenic bacteria in the environment (e.g., dirty towels, sports equipment, door handles, pools, beauty salons), the condition of the skin itself and the entire body are also significant. Dry, cracked, or irritated skin, chronic dermatological diseases (e.g., atopic dermatitis, psoriasis), excessive sweating, as well as poor hygiene or, conversely, overly aggressive washing that destroys the natural hydrolipid barrier—these all promote bacterial colonization and facilitate the development of infection. An equally important factor is the unconsidered use of antibiotics, both oral and topical, which may lead to the emergence of antibiotic-resistant bacteria and recurring skin infections. From the patient’s perspective, bacterial skin infection should be understood as a state in which the balance between “good” and “bad” bacteria on the skin surface and the integrity of the epidermal barrier have been severely disrupted—the body then mounts a strong defense reaction, resulting in visible inflammatory symptoms. Early detection, accurate assessment of the infection’s type and depth, and rapid implementation of appropriate treatment (ranging from simple antiseptics and proper care to antibiotics and surgical interventions in severe cases) determine whether the disease process is effectively halted or whether there is a risk of further infection spread and systemic complications.
Most common symptoms of skin infections
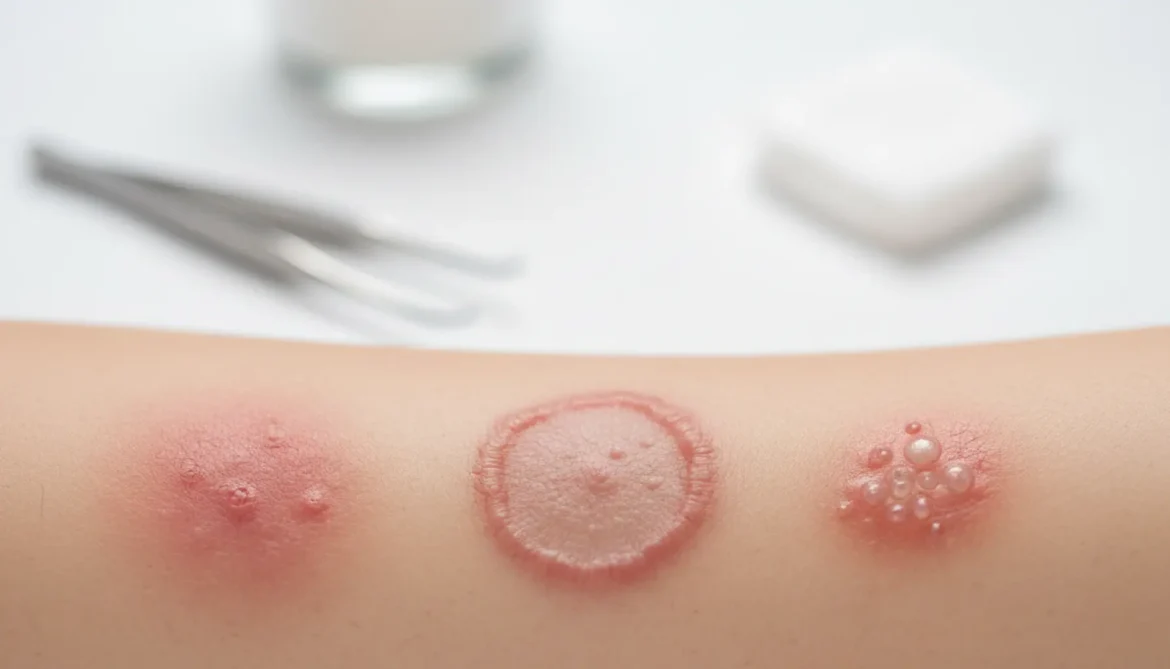
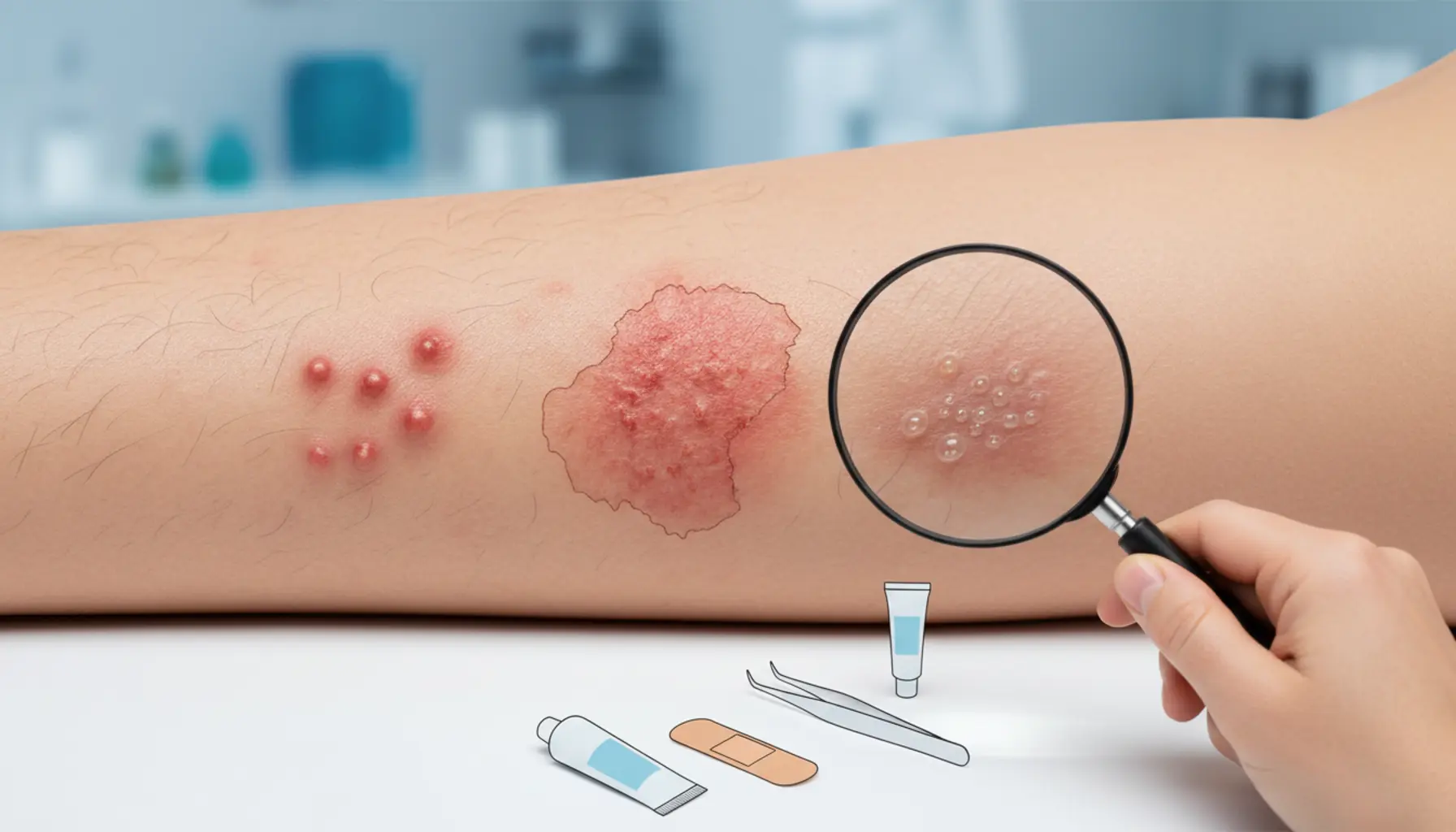
Bacterial skin infections can present with very diverse clinical pictures, but several typical symptoms most often appear and should raise vigilance. The basics include redness (erythema), swelling, pain, and increased warmth of the skin at the infection site—these are classic signs of inflammation. Erythema usually has sharply demarcated edges or, conversely, gradually spreads into surrounding tissues; the skin may feel tense and “hot” to the touch. Patients often describe a sensation of throbbing, pressure, or “pulling” in the affected area, resulting from increasing swelling and heightened blood flow. A characteristic, though not always immediate, symptom is also pain—ranging from slight tenderness to deep, stabbing pain that may hinder mobility or daily activities, especially if lesions are near joints or on the feet. In addition to local discomforts, there is often the appearance of a rash of varying character. These may be small red spots, papules, pustules with purulent content, or vesicles filled with cloudy fluid or larger blisters that, after rupture, leave weeping erosions and crusts. In impetigo, the typical sign is honey-yellow crusts on a red base, most often on children’s faces and hands, whereas in folliculitis, a small pustule is visibly located around the hair, often with a whitish purulent tip. Alarm signs are lesions that enlarge in a short time, harden, the skin above becomes glossy and tight, and pain increases—this may indicate abscess or phlegmon formation requiring urgent medical attention. In some patients, bacterial skin infections also manifest with itching, especially at first, due to irritation of sensory receptors by bacterial toxins and inflammatory mediators. Scratching further damages the epidermis and facilitates bacterial spread to adjacent areas, which over time may lead to the appearance of additional inflammatory foci. In the course of some skin infections, scaling of the skin, cracks, painful fissures, and serous-purulent exudate that dries into scabs are observed. These changes may have an unpleasant odor, which is an additional clue of active bacterial involvement and not just a sterile inflammatory or allergic disease.
Besides local symptoms affecting only the skin and nearby tissues, bacterial infections increasingly cause systemic symptoms, indicating a whole-body reaction. These include fever (over 38°C), chills, malaise, muscle and joint pain, and general fatigue. Appearance of such symptoms usually indicates a more advanced infection or involvement of a larger body area, with the immune system intensely fighting the pathogen. In more serious cases, there may also be enlargement and tenderness of nearby lymph nodes, such as axillary in hand infections, inguinal in leg lesions, or cervical in facial and scalp infections. Red, slender “streaks” along the skin towards the lymph nodes may be visible—this indicates inflammation spreading through lymphatic vessels (lymphangitis) and requires prompt treatment. In addition to infection-related symptoms, patients may experience problems related to lesions in sensitive body areas. Infections around the eyes may cause eyelid swelling, trouble opening eyes, tearing, and photophobia; changes near the mouth can make eating and drinking difficult, while purulent foci on the feet and shins often lead to walking problems, limping, and a need to offload the affected limb. Attention should also be paid to atypical or “masked” symptoms, especially in the elderly, diabetic patients, those with neuropathy, or impaired sensation—in these cases, infection can develop almost painlessly, with less pronounced redness, and the first sign may be sudden weakness, sleepiness, or marked deterioration in glycemic control. In children, skin infections are often accompanied by anxiety, irritability, crying, loss of appetite, or sleep difficulties, even when skin lesions seem minor. Thus, it is crucial not only to observe the lesions, pustules, or swelling but also to monitor the whole body and symptom dynamics: rapidly increasing pain, swelling, emergence of fever, malaise, or red streaks along a limb are warning signs that should prompt urgent medical consultation and diagnostics for a more serious bacterial skin infection.
Main causes and risk factors of skin infections
Bacterial skin infections are most often triggered by bacteria that naturally reside on our skin or in the environment and become pathogenic only when they find a “gateway” into deeper tissue layers. The main pathogens are staphylococci (especially Staphylococcus aureus, including methicillin-resistant MRSA) and beta-hemolytic group A streptococci. Normally, they are partially controlled by the skin’s acidic pH, sebum layer, proper microbiome, and an efficiently functioning immune system. When this balance is disturbed—e.g., by mechanical injury, excessive sweating, skin maceration, or improper care—bacteria easily penetrate the epidermis, hair follicles, or damaged hydrolipid barrier and begin to multiply. Thus, the key reason is any breach of skin continuity: small wounds, shaving abrasions, scratches from insect bites, cracked heels, calluses, heat and chemical burns, as well as postoperative wounds or bedsores. Even seemingly trivial cracks in very dry or atopic skin can become a starting point for extensive infection, since the damaged skin no longer serves its protective function. Poor hygiene is another significant factor—both insufficient hygiene (rare washing, wearing sweaty clothes, sharing towels or razors) and excess in the form of aggressive cleansers, which destroy the natural lipid cover and disrupt the physiological skin flora. Bad habits, like popping pimples, picking scabs, scratching allergic or insect-irritated lesions, also increase the risk by mechanically introducing bacteria deeper into the tissues. Secondary causes also include chronic skin diseases such as atopic dermatitis, psoriasis, or contact eczema—the accompanying microtraumas, itching, and constant scratching favor colonization by pathogenic bacteria and recurrent infections. Infections may also occur more frequently on areas of skin exposed to chronic irritation and pressure—e.g., under straps, bras, where prostheses, sports protectors, or tight footwear rub the skin, accumulating sweat and bacteria, and a lack of ventilation exacerbates maceration and inflammation. Climate and environment also matter—warm, humid conditions, use of pools with poorly disinfected water, saunas, gyms, and close skin-to-skin contact in crowded places (locker rooms, fitness clubs, dormitories) increase exposure to pathogenic strains, particularly MRSA. In children and physically active individuals, frequent causes are sports injuries, abrasions, and cuts that do not receive sufficient hygienic care—not cleaning and securing wounds immediately creates ideal conditions for infection development. Another risk factor is excessive use of topical and systemic antibiotics without proper indications and medical supervision—this leads to selection of resistant bacterial strains that more easily colonize the skin and trigger more severe and harder-to-treat infections.
The risk of developing bacterial skin infections greatly depends on overall health and immune system function. People with weakened immunity—due to diabetes, chronic kidney failure, liver disease, cancers, HIV infection, after chemotherapy, immunosuppressive therapy, or long-term use of glucocorticoids—have much more frequent, extensive infections such as multiple boils, phlegmons, or carbuncles. Diabetic patients also suffer from microcirculation disorders, neuropathy, and slow wound healing, especially predisposing them to infections of the feet (the so-called diabetic foot), where even a tiny skin crack or shoe abrasion may turn into a dangerous infection. The elderly are also at risk, as their skin is thinner, drier, more prone to injury, and usually comorbid with chronic diseases and polypharmacy that may weaken immune response. Children, especially those in nurseries, kindergartens, and schools, are exposed to rapid transmission of contact infections (such as impetigo) via direct touch, shared toys, or textiles. Lifestyle factors are also significant: smoking and excessive alcohol use impair skin blood supply and wound healing; chronic stress, insomnia, and improper diet (low in protein, vitamins A, C, E, zinc) weaken the body’s natural defenses. Overweight and obesity promote deep skin folds with warm, humid environments that encourage maceration, abrasions, and bacterial superinfection—recurrent inflammations are common in the armpits, under breasts, groin, or lower abdomen. Invasive medical and cosmetic procedures are also significant risk factors: surgeries, catheter insertions, intravenous sticks, piercing, tattoos, or unprofessionally performed procedures such as manicure, pedicure, waxing, or microneedle mesotherapy. If not performed in strictly sterile conditions, they are a direct route for microorganisms to enter the tissues, leading to both superficial infections and serious abscesses or hospital-acquired infections that can be hard to treat. The role of contact with other carriers of pathogenic bacteria should also not be neglected—especially for those living in communal settings (care homes, barracks, dormitories) or families in which someone has recurring boils or MRSA infections. Sharing bedding, towels, sportswear, or even electronic devices touched with bare hands may facilitate microorganism transfer. Particularly at risk are also healthcare workers, beauticians, hairdressers, and contact sport athletes (wrestlers, judokas, combat fighters), who regularly encounter others’ skin and sweat; minor skin injuries can be quickly colonized and develop into infection. All these factors—from local skin-barrier damage, through chronic diseases, to environmental and hygienic habits—interact to determine whether bacteria contact results in a temporary colonization or full-blown, and sometimes severe, bacterial skin infection.
Effective diagnostics of skin infections
Effective diagnosis of bacterial skin infections is primarily based on a detailed medical interview and physical examination, with additional tests being secondary. The doctor begins by speaking with the patient, asking about the timing of lesion appearance, rate of progression, prior injuries, scratches, insect bites, or contact with others having similar symptoms. Information about chronic diseases is crucial, especially diabetes, heart failure, autoimmune disorders, immunosuppressive medications, or recent surgery—all of which can increase susceptibility to infection and influence its course. At this stage, the doctor also assesses the patient’s general state, asking about fever, chills, muscle aches, weakness, or nausea, which might indicate that the infection is spreading beyond the skin. The next step is a thorough inspection of the skin: the doctor evaluates the location and extent of changes, their color, warmth, presence of swelling, blisters, pustules, scabs, ulcers, or purulent discharge. A typical bacterial skin infection presents as a vivid red, painful, warm, often swollen area, sometimes with clearly demarcated edges (as in erysipelas) or a diffuse erythema (as in cellulitis). Skin abscesses are characterized by a tense, painful lump with possible fluctuation, indicating a pus pocket. Careful palpation helps determine whether the process is limited to the epidermis and dermis, or also involves the subcutaneous tissue and deeper structures, which is crucial for planning further management. It is also extremely important to differentiate bacterial skin infections from other conditions with similar appearances, such as allergic contact dermatitis, urticaria, shingles, thrombophlebitis, gouty lesions, or rheumatic diseases. A dermatologist or family doctor, based on typical clinical presentation, can often diagnose in the first appointment, but if in doubt, orders additional tests.
Additional tests in skin infection diagnostics are selected individually depending on symptom severity, concomitant diseases, and suspicion of complications. The basic tool is a swab from the surface of the lesion or tissue sampling (e.g., abscess content) for bacterial culture and antibiogram. This helps identify the precise microbe responsible (e.g., Staphylococcus aureus, including MRSA or Streptococcus pyogenes) and choose the most effective antibiotic, which is particularly important with recurring, extensive, or hard-to-treat infections. In some cases, especially when the lesion is dry or hard to access, gentle epidermal scrapings or skin biopsy are performed, allowing a pathologist to assess the histopathological image and confirm or exclude bacterial, fungal, or autoimmune infection. When systemic spread of infection is suspected or strong general symptoms are present, laboratory blood tests are ordered: blood count (often with increased leukocytes), CRP, ESR, and procalcitonin to assess inflammation severity and sepsis risk. In patients with chronic ulcers, burns, or large wounds, especially on the shins, glucose levels and kidney and liver parameters are also checked to catch healing barriers. For imaging, soft tissue ultrasound is commonly used—it helps differentiate simple inflammatory swelling from pus pockets requiring incision and drainage, and assess the depth of infection spread. In severe, atypical, or rapidly progressing cases (such as suspected gas gangrene or necrotizing fasciitis), CT or MRI is performed for precise extent assessment and surgical planning. Rapid bedside tests, such as strip tests detecting bacterial toxins, are increasingly important, though not yet standard. It is essential to remember that diagnosing skin infections also involves identifying facilitating factors—thus, patients are often referred to a diabetologist, angiologist, or immunologist for systemic assessment. Using a comprehensive approach—thorough history, skin exam, targeted microbiological, laboratory, and imaging studies—makes it possible to not only make an accurate diagnosis but also select optimal therapy and prevent recurrences.
Modern treatment methods and home remedies
Modern treatment of bacterial skin infections combines precise pharmacotherapy with judicious use of topical methods and support from home care. The cornerstone is a properly chosen antibiotic—topical or systemic—selected based on the type and extent of lesions, patient age, coexisting diseases, and risk of bacterial resistance. For mild and limited infections such as minor impetigo or folliculitis, topical preparations in ointment, cream, or gel form containing antibiotics (e.g., mupirocin, fusidic acid), or antibiotic-anti-inflammatory combinations, are usually sufficient. Increasingly, modern dressings with added silver, medical honey, or polyhexanide are used, offering antibacterial action, preventing biofilm, and supporting faster healing while reducing the need for frequent dressing changes. In more extensive infections accompanied by fever or systemic symptoms, oral or intravenous antibiotics are started based primarily on likely etiological factors (usually staphylococci and streptococci) and current resistance guidelines, including MRSA strains. In more complex cases, culture and antibiogram testing is performed to select the narrowest but most effective agent possible, helping limit antibiotic resistance problems. Surgical treatment, such as incision and drainage of abscesses, remains the gold standard for pus collections—antibiotics alone are often insufficient if infected material is not mechanically removed. Modern techniques are used, such as ultrasound-guided drainage or vacuum-assisted closure (VAC) dressings, which help cleanse wounds and accelerate granulation. For patients with chronic conditions like diabetes, multidisciplinary care is crucial—simultaneous glucose control, adjustment of immunosuppressants, correction of nutritional deficiencies (protein, zinc, vitamin C and D), and education on daily skin care significantly increase treatment success. Supportive procedures are gaining importance, including low-level laser therapy, anti-inflammatory LED light therapy, and use of specialized preparations to restore the skin microbiome balance—especially relevant for recurring infections or coexisting dermatoses such as atopic dermatitis.
Medical therapy can be complemented by well-chosen, safe home remedies that do not substitute antibiotics but may relieve symptoms, speed healing, and reduce complication risk. Proper, daily hygiene of the infected area is key—gentle washing with lukewarm water and a mild cleanser of neutral pH, without vigorous rubbing, followed by careful but delicate drying with a clean, separate towel. It is important to avoid “at home” popping, squeezing of pustules, or self-incision of abscesses, as this increases the risk of spreading bacteria and scar formation; such procedures should be performed only in a medical office. At home, you can use warm, but not hot compresses of sterile gauze soaked in saline, which promote spontaneous drainage of small purulent lesions and relieve pain—remembering to wash hands thoroughly before and after wound contact. It is also beneficial to use preparations with dexpanthenol, allantoin, or zinc, supporting epidermal regeneration, but only on areas without active pus ooze—otherwise, prior medical consultation is necessary. Some natural substances, such as medical honey or aloe, have documented anti-inflammatory and soothing properties, but should only be used in safety-confirmed products and after consulting with a doctor, especially in people with allergies. Everyday habits are essential for relapse prevention: wearing breathable, cotton clothes, frequent underwear and sock changes, avoiding sharing towels, razors, or cosmetic utensils, regular disinfection of bathroom surfaces, and thorough hand washing after wound contact. For those using gyms or pools, it is recommended to shower immediately after exercise, use one’s own flip-flops and towels, and avoid sitting directly on mats or benches without a fabric barrier. A healthy lifestyle also supports recovery: a diet rich in vegetables, fruits, whole-grain cereals, quality protein, proper hydration, sleep, and stress reduction helps keep the immune system strong, lowering the risk of severe infection. Home remedies should always be adapted to your doctor’s instructions—if symptoms worsen despite using them, fever, chills, severe pain, rapidly spreading redness, or pus appear, urgent medical consultation and possible adjustment of therapy to current treatment standards are necessary.
How to prevent bacterial skin infections?
Preventing bacterial skin infections primarily relies on maintaining an intact skin barrier and limiting exposure to pathogenic microorganisms. Daily but sensible hygiene plays a key role. It’s worth washing skin with gentle products of neutral or slightly acidic pH that do not disturb the natural hydrolipid layer. Excessive use of strongly degreasing gels, mechanical scrubs, or alcohol-based agents leads to drying and microcracks, paradoxically increasing the risk of bacterial entry. After washing, skin should be gently patted dry with a clean towel—avoid rubbing; each household member should have their own towel and replace it regularly. Hand washing is also important in prevention—use water and soap for at least 20 seconds—especially after using the toilet, before preparing and eating food, and after contact with wounds, secretions, or surfaces in public places. People using gyms, pools, or saunas should wear flip-flops, avoid sitting bare on shared benches, and shower as soon as possible after workouts, removing sweaty clothing that promotes bacterial proliferation. Proper clothing choice is important: breathable materials, preferably cotton, wick moisture away and do not cause abrasions. Tight clothes, synthetic fabrics, or prolonged wear of wet swimsuits or underwear create an ideal environment for bacterial growth and should be limited.
It is equally important to properly manage any skin damage—even minor ones. Every cut, scratch, cracked heel, or shoe-induced abrasion should be promptly rinsed with running water and disinfected with a gentle, skin-friendly antiseptic. If needed, wounds can be covered with a sterile plaster or dressing, remembering to change them regularly and watch for increasing redness, pain, or purulent exudate. Popping pimples, abscesses, or boils must be strictly avoided—such “at-home” activities let bacteria spread more deeply into tissues and the bloodstream. People with chronic skin conditions (e.g., atopic dermatitis, psoriasis, acne) should strictly follow medical recommendations to limit scratching and skin cracking. Diabetics are a special risk group—for them, daily foot care (checking for cracks, calluses, wounds), proper footwear, careful nail trimming, and prompt doctor consultation for any suspicious injury are essential. Lifestyle also matters: maintaining a healthy weight, eating a balanced diet rich in vegetables, fruits, whole grains, healthy fats, and adequate protein needed for tissue regeneration, avoiding smoking and excessive alcohol (which impair body defenses and slow healing). Sleep and stress reduction should not be overlooked—chronic stress and lack of sleep disrupt immune function, promoting recurrent infections. Another important element is avoiding sharing personal items like razors, towels, sponges, nail scissors; in homes where someone suffers from an active skin infection, frequently touched surfaces such as doorknobs, taps, and remotes should be regularly disinfected. For recurring infections or suspected contact with resistant bacteria (e.g., MRSA), it’s advisable to consult a doctor for a prevention plan, which may include short-term special nasal or skin preparations as well as testing and possible treatment of carriers in the patient’s close environment.
Summary
Bacterial skin infections are a common condition that can lead to serious complications if not recognized and treated in time. Early symptom detection and knowledge of risk factors enable a quick response and effective treatment implementation. Professional diagnostics, modern treatment methods, and support from home remedies help not only accelerate recovery but also avoid recurrence. By maintaining proper hygiene and preventive habits, you can significantly reduce the risk of reinfection. Remember to consult a dermatologist at the first worrying symptoms.