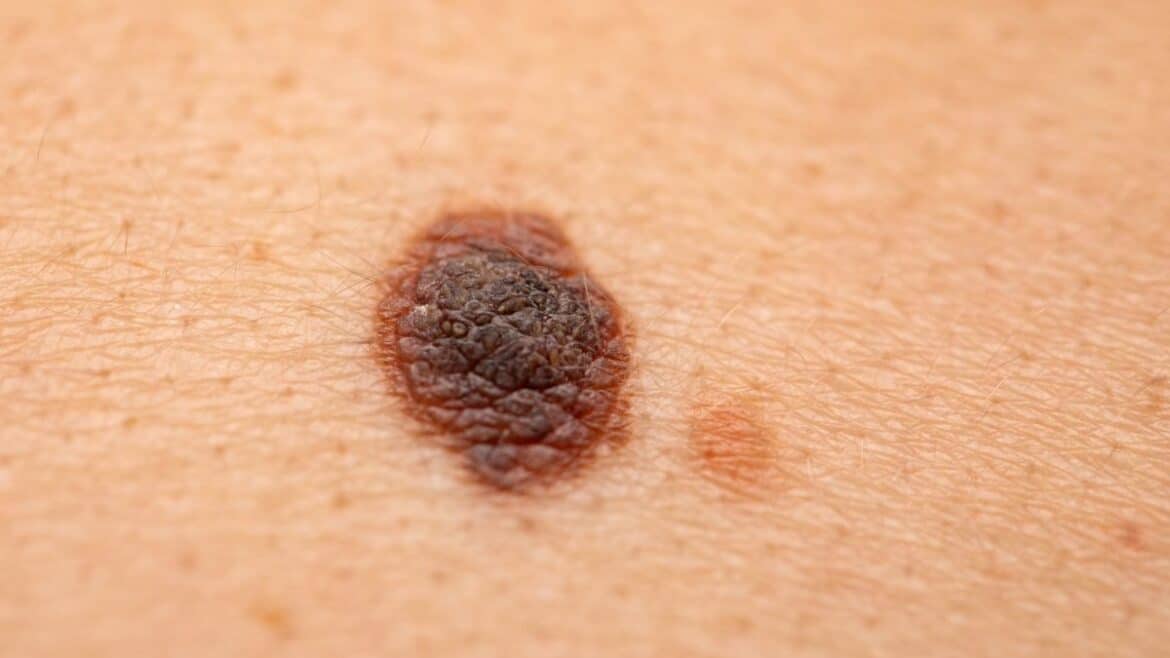
Learn about the symptoms and appearance of skin melanoma. Learn how to distinguish cancer from a common mole, and learn about melanoma diagnosis and prevention.
Table of Contents
- What is skin melanoma? Definition and epidemiology
- What does melanoma look like? Typical features and differences from a mole
- Symptoms of skin melanoma – what to watch for?
- Melanoma diagnostics: tests and recognition methods
- Melanoma prevention – how to protect yourself from skin cancer?
- Treatment of skin melanoma – chances for cure and the latest methods
What is skin melanoma? Definition and epidemiology
Skin melanoma is one of the most aggressive malignant tumours originating from the skin’s pigment cells, called melanocytes. It is considered particularly dangerous due to its tendency for rapid growth and early metastasis, both to nearby lymph nodes and to other internal organs, such as the lungs, liver, or brain. Melanoma can develop virtually anywhere on the skin, also on mucous membranes (mouth, genital organs) or in the eye, but most often forms in areas exposed to intense ultraviolet (UV) radiation, such as the back, lower limbs, or face. This cancer can arise either from healthy, undamaged skin or from pre-existing pigmented lesions, such as nevi (commonly called “moles”). Melanoma shows diverse clinical and histopathological appearances, which is why it often goes unnoticed for a long time, and its diagnosis may be delayed—significantly affecting the patient’s prognosis. The development of melanoma is strictly related to the accumulation of mutations in the DNA of melanocytes, which may be caused, among other things, by chronic or intense sun exposure, as well as by frequent use of tanning beds. Important risk factors include genetic predisposition, fair skin, numerous atypical moles, and a previous family history of melanoma.
Melanoma is relatively less common than other skin cancers, such as basal cell carcinoma or squamous cell carcinoma, yet it accounts for the highest number of skin cancer-related deaths worldwide. According to World Health Organization (WHO) data, up to 325,000 people develop melanoma every year, and global deaths exceed 57,000 annually. In Poland, the annual number of new melanoma cases is systematically rising—currently estimated at about 4,000, with almost half diagnosed at an advanced stage, when treatment options are limited. The increase is especially visible among young adults and middle-aged individuals, directly linked to lifestyle changes such as the popularity of tanning and more frequent travel to sunny countries. Environmental factors, such as increased UV radiation due to ozone layer depletion, also have a significant impact. Melanoma affects both women and men, with different lesion locations: in women, changes most often appear on the lower limbs, while in men, the torso and back are more affected. Despite advances in diagnostics and treatment, melanoma remains a cancer with high mortality, much of which could be avoided through increased social awareness, regular monitoring of skin lesions, and early detection of worrying symptoms. Melanoma epidemiology also points to the essential role of prevention programs that can reduce incidence and improve therapeutic outcomes by promoting a healthy lifestyle and responsible sunlight exposure.
What does melanoma look like? Typical features and differences from a mole
In its early stages, melanoma may resemble a regular mole (pigmented nevus), but there are important differences that allow it to be distinguished from benign changes—a key factor for early diagnosis and effective treatment of this serious cancer. Melanoma most often appears as a lesion with an irregular shape and color, with uneven, jagged borders and varied pigmentation—shades of brown, black, gray, and sometimes red, navy, or even white can all be visible. The cancerous lesion frequently grows rapidly—sudden increase in the size of a mole or the appearance of a completely new lesion, especially in adults, is a cause for concern. Another characteristic sign of melanoma is asymmetry—if you imagine drawing a line through the lesion, both halves are often not identical, which distinguishes melanoma from benign moles that are usually symmetrical and round. Melanomas may be flat or slightly raised above the skin surface, and sometimes take the form of an ulceration or nodule that bleeds easily, itches, or hurts. It’s worth remembering that melanoma can occur anywhere on the body, even in areas rarely exposed to the sun—on the soles of the feet, palms, buttocks, or under a nail (subungual melanoma).
Differentiating melanoma from a harmless mole is often difficult for those without medical training, which is why practical rules, such as the ABCDE rule, were developed to help assess specific features of a skin lesion: A for asymmetry (uneven halves), B for border (uneven, jagged, blurred edges), C for color (multiple, uneven colors), D for diameter (rapid growth or evolution of the mark), E for evolution (changes in appearance—size, shape, color, occurrence of bleeding or itching). By contrast, typical moles are symmetrical, have an even brown color, well-defined borders, and do not change appearance over years. An additional criterion is the presence of warning signs—if a mole shows symptoms such as itching, burning, bleeding, peeling, the appearance of new colors, or rapid enlargement, you should consult a dermatologist. Melanomas can also develop from existing moles that begin to change dramatically—showing asymmetry, varied coloration, irregular borders, and elevation above the skin surface. Furthermore, melanoma can appear in people with fair skin or many pigment nevi, but does not spare those with darker complexions, so everyone should remain alert. Note that in the beginning, melanoma may not cause any symptoms, making it easy to ignore—regular skin checks, awareness of your moles, and prompt reaction to worrisome changes remain the most important aspects of prevention and early detection of skin cancers, including melanoma.
Symptoms of skin melanoma – what to watch for?
Skin melanoma is a cancer that often develops silently or does not produce any clear symptoms for a long time, which makes it particularly dangerous. The most characteristic symptom is the appearance of a new pigmented lesion on the skin or suspicious changes in an existing mole. Early warning signs include a sudden size change—if a mole begins to grow rapidly and exceeds 6 mm in diameter, this should raise concern. Moles from which melanoma develops often become irregular, asymmetrical—one part of the lesion may be clearly separated from another, and the whole may not resemble a classic round mole. Another important feature is uneven, jagged, or poorly defined edges spreading into healthy skin. Melanoma often stands out due to its unusual coloring—there may be a large number of shades within a single lesion; various shades of brown, black, gray, more rarely yellow, red, pink, or even white. Particularly troubling is a mole getting darker or black irregular dots appearing on it. Melanoma is also characterized by textural changes—nodules, hardening, or elevations that appear suddenly or cause the surface area of the change to increase over time. Pay attention to all evolutionary changes: rapid “transformation” of a mole, sudden reddening around it, or an increase in height—these raise suspicion of malignancy. Key warning signs for melanoma include subjective symptoms—moles beginning to itch, burn, hurt, or bleed. Particularly concerning is ulceration or the sudden release of serous fluid from the lesion. Bleeding moles should always be taken seriously if they are not associated with mechanical injury. Often, the first sign of nail melanoma is a longitudinal, dark, asymmetrical band on the nail plate, which may widen over time and even destroy the nail. In older people or those with fair skin, melanoma tends to develop in less visible places—on the soles of the feet, under the nails, in intimate areas, the scalp, or behind the ears. Vigilance is especially important in these locations, as early symptoms may go unnoticed for a long time, significantly hampering early intervention. Sometimes, patients also report enlargement of local lymph nodes or the appearance of new, growing lumps near a mole, indicating the possible start of metastasis.

In clinical practice, the ABCDE rule is used to distinguish early symptoms of melanoma from benign nevi and serves as a practical diagnostic guide. Each letter refers to key features: A – asymmetry, B – border irregularity, C – color variation, D – diameter over 6 mm, E – evolution (any changes in the lesion’s appearance). The more criteria met, the higher the chance of melanoma. Other warning signs are the appearance of new pigmented lesions in adults, especially after age 40, rapidly expanding lesions, sensation of skin tension around a mole, or chronic inflammation. When melanoma is located on mucous membranes (mouth, genitalia), the symptoms may be even harder to spot and may go unnoticed for a long time. This cancer can “mimic” a benign lesion for many months or years. Since melanoma can present in various clinical forms (from a flat spot to a highly raised nodule), any alarming sign regarding the appearance, structure, color, or behaviour of a mole should be taken seriously. Importantly, not all melanomas are dark—there are also amelanotic forms, practically devoid of pigment, appearing flesh-colored or light pink, making them even harder to diagnose. Pay attention to discoloration developing around a wide existing lesion as well as general symptoms such as weakness, enlarged lymph nodes, or even metastatic symptoms in advanced stages. Regular skin checks, self-examination, and promptly seeing a dermatologist when noticing any of these symptoms are key to detecting melanoma at an early, curable stage.
Melanoma diagnostics: tests and recognition methods
Diagnosing skin melanoma is a multi-step process aimed at the most accurate identification of the type, stage, and extent of the cancer. It is based on a thorough medical history and clinical examination of the skin in-office, during which the dermatologist assesses the nature of the lesion, its appearance, size, color, and any alarming features—based on the ABCDE rule and clinical experience. Dermatoscopy is a key tool—a non-invasive examination using a specialist microscope (dermatoscope) that allows for magnified and detailed observation of the pigment structure visible in the epidermis and dermis. Dermatoscopy is particularly useful for distinguishing benign from malignant moles, highlighting typical melanoma features such as irregular pigment network, spots of different colors, or an asymmetrical arrangement. In some cases, videodermatoscopy is also used, making it possible to archive images and monitor changes over time, which is particularly helpful for patients with many moles. In differentiating melanoma from other skin cancers or pigmented nevi, confocal microscopy can also be used, allowing cellular-level analysis. An important part of diagnostics is the full-body examination to identify unusual locations for melanoma, such as the scalp, genitals, under the nails, or mucous membranes.
However, the most decisive examination for melanoma diagnosis remains the histopathological examination. Suspicion of melanoma is an indication for surgical removal of the whole lesion—a so-called excisional biopsy with a margin of healthy tissue. Fragment (incisional) biopsies should be avoided as they carry a greater risk of complications. After removal, the material goes to a histopathology laboratory, where, under a microscope, the features of pigment cells are assessed: depth of invasion (Breslow scale), presence of ulceration, mitotic index, and the surgical margin. These parameters are crucial in determining further therapeutic steps, risk of metastasis, and prognosis. For nail or mucous membrane melanoma, particular caution in collecting samples is needed to avoid missing early stages. In advanced melanoma or suspected metastases, imaging studies such as ultrasound (USG) of local lymph nodes, computed tomography (CT), magnetic resonance imaging (MRI), or positron emission tomography (PET) are used. Imaging is key to assessing disease stage, detecting distant metastases, and planning therapy. In some cases, the physician may order a sentinel lymph node biopsy—involving identification and removal of the first lymph node to which cancer cells might have spread—providing exact assessment of melanoma progression and optimal therapy selection. Occasionally, genetic tests are performed to check for mutations predisposing to rapid tumour growth and for planning individualized molecularly targeted therapies. Laboratory diagnostics, including tumor markers, are of limited use, though they can be helpful in prognosis or disease monitoring. Comprehensive diagnosis using advanced imaging, histopathology, and molecular methods significantly improves early detection and long-term cure rates for melanoma.
Melanoma prevention – how to protect yourself from skin cancer?
Rational melanoma prevention is mainly based on minimizing exposure to risk factors, most importantly ultraviolet (UV) radiation, the main driver of DNA mutations leading to melanoma. Avoiding intense and prolonged sunbathing, both natural and artificial in tanning salons, is crucial—lamp radiation is just as dangerous to skin as sunlight. Particular caution is needed during peak sun hours, from 10 AM to 4 PM, when UV exposure is greatest, and during holidays in sunny countries. Protection includes the use of high-SPF (at least 30) sunscreens, regular reapplication every 2–3 hours and after swimming. Equally important is mechanical protection by wearing long sleeves, wide-brimmed hats, UV-blocking sunglasses, and staying in the shade whenever possible. Melanoma prevention in children and adolescents is vital, because sunburns at a young age exponentially increase the risk of skin cancer later in life. Parents should regularly apply sunscreen to their children, choose shady places during walks, and teach kids sun-safety rules from an early age. Awareness programs for both adults and youth are crucial, emphasizing year-round sun protection—not just in summer, but also in winter, especially in the mountains where UV intensity is high due to reflection off snow. Prevention also includes a healthy lifestyle, such as regular skin care and avoiding trauma to existing nevi, especially those exposed to friction from clothing or jewelry.
The foundation of self-screening is regular, monthly skin checks in a well-lit room, ideally with mirrors and a second person to help check hard-to-see areas such as the back or scalp. Pay attention to any new pigmented lesions and dynamic changes in existing moles—enlargement, shape or color change, itching, pain, or bleeding are all warning signs. Any doubts warrant visiting a dermatologist, who will assess lesions via dermatoscopy and decide on next steps. High-risk individuals (fair-skinned people, those with many moles, a history of skin cancer, or genetic burden) should regularly see a dermatologist—ideally yearly or more frequently if recommended. It’s useful to keep photographic records of moles to spot changes more easily. Melanoma prevention also requires a cautious approach to tanning salons—the World Health Organization officially classifies UV lamps as carcinogenic, so regular tanning salon use should be strongly discouraged. Wider initiatives like free skin check campaigns, screening programs, and public education on the effects of excessive sun exposure are also important. The earlier effective prevention is implemented—both through individual care and through public health policies—the greater the chances of reducing cases and improving outcomes for early-detected melanoma.
Treatment of skin melanoma – chances for cure and the latest methods
The treatment of skin melanoma rests on several key therapeutic pillars, tailored to the stage of the cancer, the patient’s clinical features, and individual risk factors. The best chance for total cure is in patients whose melanoma was detected at a very early stage (stage 0–I). The gold standard is radical surgical excision of the lesion with an appropriate margin of healthy tissue—early removal of the cancerous focus allows for 5-year survival rates as high as 90–100%. When excised lesions show features indicating metastatic risk (such as greater thickness, ulceration), the doctor may also recommend removal of adjacent lymph nodes and additional imaging. Unfortunately, in later stages of melanoma, the chances for permanent cure decrease, due to the tumour’s rapid metastatic spread via both lymphatic and blood vessels. In locally advanced stages and in patients with lymph node or distant organ metastases, treatment is a considerable challenge and relies on modern systemic methods, often involving targeted therapies or immunotherapy.
In recent years, melanoma treatment has been revolutionized by advances in modern systemic therapies. Immunotherapy uses, among others, immune checkpoint inhibitors (e.g., anti-PD-1 antibodies: pembrolizumab, nivolumab), which unlock the body’s natural immune response and enable it to recognize and destroy cancer cells. This treatment yields clear benefits even for patients with metastatic melanoma and sometimes leads to years-long remissions. For those with confirmed BRAF gene mutation (present in approx. 40-50% of melanomas), targeted therapy with BRAF inhibitors (dabrafenib, vemurafenib) and MEK inhibitors (trametinib, cobimetinib) is used to block cellular pathways triggering tumour growth. Sometimes targeted drugs are combined with immunotherapy for even greater effectiveness. Adjuvant therapy after surgery for advanced melanoma aims to lower recurrence risk—here too, immunotherapy and targeted treatments are beneficial. If surgery or systemic treatment isn’t possible, radiotherapy is used, though its role is limited mainly to managing symptoms or non-operable changes. Most oncology centers now offer access to innovative regimens and clinical trials—including adoptive cell therapies and cancer vaccines. Treatment decisions should always be made by specialized medical teams, based on disease stage (e.g., TNM classification), molecular features, and the patient’s general health. In advanced melanoma, psychological support, palliative care, and symptom management are vitally important to improve quality of life for patients and families. Advanced diagnostic and therapeutic methods, ongoing research, and screening programs are transforming both prognosis and access to new therapies—offering melanoma patients more possibilities for effective treatment and long-term survival even in the most challenging clinical situations.
Summary
Skin melanoma is one of the most dangerous cancers, and early detection provides the best chance for successful treatment. Knowing the characteristic symptoms, observing your moles, and distinguishing melanoma from ordinary moles are keys to early diagnosis. Quick and standardized diagnostic methods can detect suspicious changes at an early stage, while prevention—including avoiding excessive sunbathing and regular skin checks—significantly reduces the risk of disease. Modern melanoma treatments, tailored to disease stage, offer increasingly better outcomes. Take care of your skin, monitor your moles, and don’t delay a dermatology visit if you spot any suspicious symptoms.