Learn why blood vessels in the eye burst, the symptoms, and effective treatments. Learn about home remedies and professional diagnostics.
Table of Contents
- Broken blood vessel in the eye – what is it and how does it look?
- Most common causes of broken blood vessels in the eye
- Symptoms accompanying a broken blood vessel in the eye
- Home remedies for broken blood vessels – what is worth trying?
- Diagnostics and treatment of broken blood vessels – when to see a doctor?
- Prevention and prophylaxis of broken blood vessels in the eye
Broken blood vessel in the eye – what is it and how does it look?
A broken blood vessel in the eye, medically known as sub-conjunctival hemorrhage, is a fairly common but usually harmless condition that affects the eyeball. This phenomenon is the result of tiny blood vessels under the eye’s transparent conjunctiva becoming damaged. These vessels are delicate and prone to breaking under various influences, such as a sudden increase in pressure in the eye, intense coughing or sneezing, vigorous rubbing, or even minor trauma. When the vessel wall ruptures, blood leaks onto the surface of the sclera—the white outer part of the eyeball—but remains under the conjunctiva. As a result, a characteristic, intense red spot appears on the eye, which can vary in shape and size, from a tiny dot to an extensive, pronounced “blood stain.” Although the appearance may be alarming, in most cases it does not cause pain, impaired vision, or other systemic symptoms. The blood spot may cause concern, but it generally does not pose a serious health threat. Usually, the hemorrhage is reabsorbed naturally within several days to two weeks—during this time, the blood is gradually absorbed by the body, and the spot changes color from bright red through yellow to complete disappearance.
The appearance of a broken blood vessel in the eye is quite distinctive and easy for most people to recognize even without a medical consultation. The hemorrhagic spot often appears suddenly and without an obvious reason, covering various areas of the eye’s white—sometimes as a single small dot, other times as a broad red patch covering much of the sclera. Unlike redness or injection, which tinge the whole eye, a sub-conjunctival hemorrhage is limited to a clearly demarcated area. Its intensity and size may depend on the size of the damaged vessel and individual physiological factors. In some people, the change may develop from sudden laughter, crying, or wearing contact lenses if the conjunctiva was irritated and rubbed. Many patients only notice the spot during morning face washing or when looking in the mirror, since it does not cause burning, itching, photophobia, or visual disturbances. There’s usually no swelling or discharge either, distinguishing this state from certain infectious eye conditions. The only discomfort may be a slight foreign body sensation under the eyelid or a feeling of dryness, though this is rare. The final appearance of the lesion depends not just on the cause of the break but also on the overall condition of the blood vessels, patient age, genetic factors, and the influence of blood-thinning medications. In practice, a broken blood vessel in the eye mainly requires observation; only in repeated or particularly heavy hemorrhages is specialist consultation necessary to rule out bleeding disorders or serious systemic diseases.
Most common causes of broken blood vessels in the eye
Broken blood vessels in the eye are often the result of trivial events but can have quite different causes. The most common reason for sub-conjunctival hemorrhage is a sudden increase in pressure inside the eye or head area, leading to the stretching and breaking of the small blood vessels beneath the conjunctiva. Such abrupt pressure spikes can occur during sneezing, intense coughing, vomiting, or strenuous physical effort—even lifting weights at home or at the gym. A frequent cause is also mechanical injury—for example, accidental impact near the eye, or rubbing it with a hand, especially if the conjunctiva is scratched. Moreover, sudden temperature changes (like entering a warm room from the cold), strong emotional or physical stress, or energetic activity such as laughter can contribute. Vessel wall fragility plays a significant role—people with brittle vessels, often due to genetic predisposition, are more susceptible to hemorrhages even with small physical stimuli.
In addition to such everyday situations, systemic diseases and medications also affect vessel fragility in the eye. A very significant factor is hypertension—elevated blood pressure results in chronic overload of vessel walls, making them more prone to damage even with minor pressure fluctuations. Diabetes patients are also at higher risk, since the condition damages small vessels (microangiopathy), noticeable in the eye and other organs. Bleeding disorders, vitamin deficiencies (especially of vitamins C or K), and the use of anticoagulant or antiplatelet drugs such as aspirin or warfarin can predispose to broken vessels. In elderly people, natural degenerative changes in vessel walls increase their brittleness. Prolonged wearing of contact lenses, leading to irritation and micro-injuries, and chronic inflammation of the conjunctiva or eyelids, also elevate risk. Notably, some causes can interact synergistically—someone taking blood thinners and suffering from chronic diseases like diabetes or hypertension is much more at risk. Due to the delicate structure of blood vessels, children may have hemorrhages after intense crying or sneezing, while in pregnant women, natural changes in blood pressure and hormones may cause it.
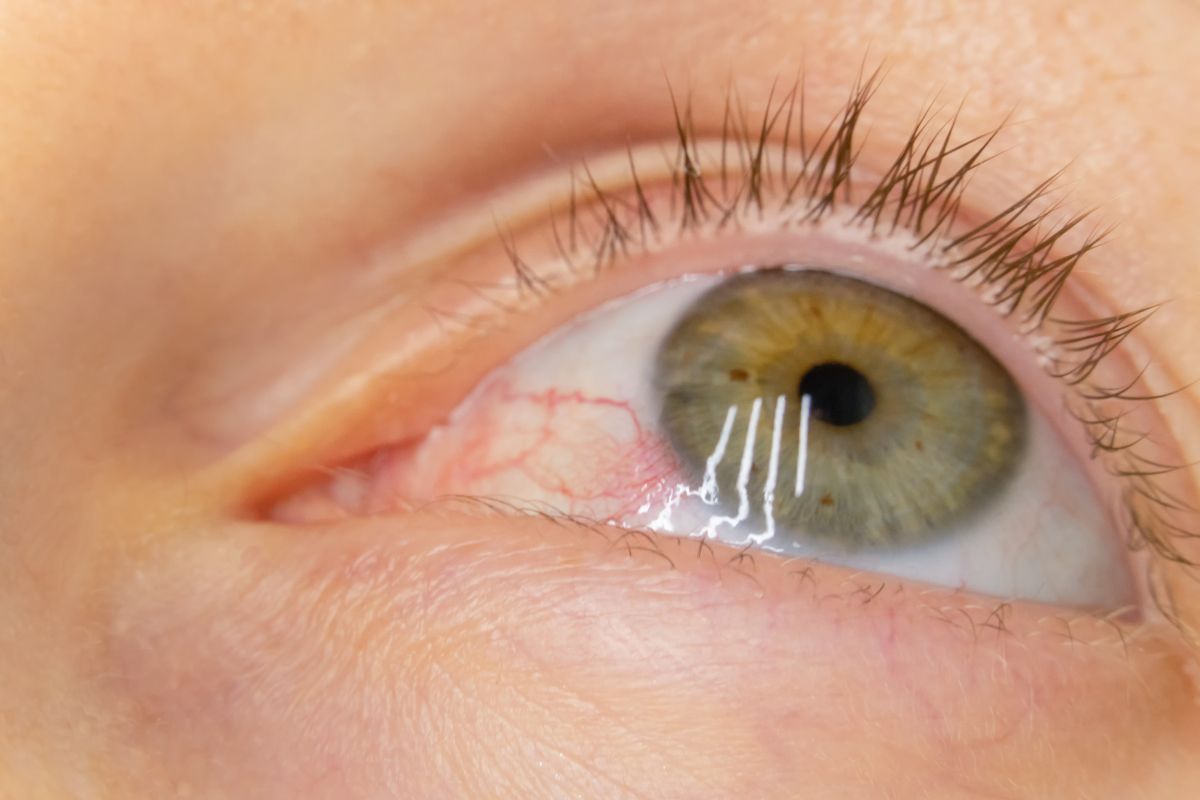
Symptoms accompanying a broken blood vessel in the eye
Most people can recognize a broken blood vessel in the eye by its distinctive visible symptoms. The clearest sign is a vivid red or purple spot on the sclera—the white part of the eye—of irregular shape and size, depending on the extent of the blood leak. Patients often describe it as a “bloody eye” or a “red spot in the eye.” This spot usually does not spread over the entire sclera, but if the hemorrhage is large, it can cover much of it, causing understandable aesthetic concern. Typically, broken blood vessels do not cause pain, burning, or a foreign body sensation—symptoms that are associated with other ophthalmic conditions such as conjunctivitis or injuries. However, some individuals, especially those with particularly delicate or irritated eye surfaces, may experience mild discomfort, slight itching, or a feeling of sand under the eyelids. The presence of blood in the eye does not affect vision sharpness, does not cause vision disturbances or photophobia, differentiating it from many more serious conditions with similar clinical presentations. Interestingly, the hemorrhage does not change significantly with blinking, eyelid massage, or eye rinsing, making it relatively easy to diagnose. Note that although the hemorrhage generally resolves on its own in a few days up to two weeks and leaves no trace, its color can gradually change—from bright red through brownish to yellowish, much like a bruise.
In some cases, a broken blood vessel may be accompanied by additional symptoms that require increased caution and may indicate a more serious underlying problem. If, apart from the red spot, there is pain, eyelid swelling, visual disturbances (blurred vision, double vision, sudden decrease in acuity), photophobia, discharge, or pulsating sensation in the eye—a prompt ophthalmological consultation is necessary. Such symptoms may suggest inflammation, deeper injuries or the presence of systemic diseases, including bleeding disorders, blood pressure spikes, or even neurological problems. Pay attention if hemorrhages occur in both eyes simultaneously, are recurrent, or are accompanied by spontaneous bleeding from the nose or gums—these kinds of symptoms may signal serious hematological diseases or vascular disorders and require quick diagnostics. In elderly patients or those with chronic diabetes or hypertension, broken blood vessels might be an early sign of vascular complications. In children, especially after prolonged coughing, crying, or vomiting, subconjunctival hemorrhages typically appear singly and usually do not require medical intervention, though their frequency and the presence of other alarming symptoms should be monitored. Also consider possible external factors—chemical irritation, prolonged exposure to dust, or improper use of contact lenses may cause microinjuries and hemorrhages, sometimes accompanied by burning or excessive tearing. Occasionally, a hemorrhage results from a minor injury forgotten by the patient, with the spot appearing hours later. Specialists also pay attention to systemic symptoms such as general weakness, fever, easy bruising, or small red spots on the skin, which may indicate hematological diseases or infections. Thorough context analysis helps assess whether the event is coincidental and harmless or requires broader diagnostics and proper treatment.
Home remedies for broken blood vessels – what is worth trying?
The appearance of a broken blood vessel in the eye often causes anxiety and questions about effective and safe home solutions. In most cases, a subconjunctival hemorrhage is mild and resolves on its own within several days to two weeks. However, appropriate home actions can support healing and prevent further breaks. The main element is protecting the eye from further trauma and excess fatigue—avoid rubbing your eyes, touching with dirty hands, and applying makeup near the lesion. Regular eye breaks, especially when working at a computer or reading for long periods, can reduce irritation and microtrauma risk. Applying cold compresses—such as a clean tissue soaked in cool water—may bring relief, lessen any swelling, and curb microbleeding by constricting the vessels. Remember not to apply ice directly to the eyelid or eye—always use a protective material barrier and limit application to a few minutes to avoid frostbite. Cool compresses are especially helpful in the first hours after the hemorrhage appears. Also, a diet rich in vitamins C and K strengthens blood vessel walls and supports quicker tissue repair. Sources of vitamin C include fresh vegetables and fruit such as peppers, parsley, or citrus fruits, while vitamin K is found in green leafy vegetables—spinach, kale, broccoli. Proper hydration, drinking at least 1.5–2 liters of water a day, and limiting stimulants—especially alcohol and cigarettes, which weaken blood vessels—help support their health. Prioritize regular, restful sleep and limit stress, which not only indirectly contributes to vascular problems but also negatively affects overall immunity.
With the popularity of natural remedies, questions arise about herbs and supplements for broken blood vessels. Caution is advised—while some products, such as rutin or extracts of horse chestnut and ginkgo biloba, have vessel-strengthening effects, all supplements should be used prudently, preferably after consulting a doctor, especially if the patient takes other medications with potential interactions. Moisturizing eye drops—so-called artificial tears—are also helpful to alleviate dryness, reduce burning, and protect the eye from further irritation. Store these products in the refrigerator for added relief during application. Avoid home-made preparations or over-the-counter redness reducers, especially those with vasoconstrictive effects (the so-called drops for “red eye”), which can mask infection or worse conditions. Remember, home remedies do not replace professional diagnosis when symptoms are frequent, accompany pain, visual disturbances, or other concerning signs. Any mechanical injury or the presence of additional complaints (such as a sandy feeling under the eyelids, photophobia, or excessive tearing) warrants a quick ophthalmology consultation. Effective self-care means not only hygienic habits, diet, rest, and appropriate compresses, but also vigilance and recognizing situations when specialist help is needed.
Diagnostics and treatment of broken blood vessels – when to see a doctor?
Most broken blood vessel cases in the eye are mild and do not need immediate medical attention. However, certain situations clearly call for ophthalmologic consultation. These warning signals include: repeated hemorrhages, pain in the eye, sudden deterioration of visual sharpness, photophobia, visible eyelid or eyeball swelling, and the presence of other concerning systemic symptoms such as fever or general body weakness. A doctor’s visit is also advised for chronic patients, such as those with hypertension, diabetes, hematological diseases, and those taking anticoagulants, as broken blood vessels may signal worsening health problems. Note that for children and pregnant women where hemorrhages come with other symptoms, extra caution and quick diagnostics are required. In the elderly, recurrences may indicate systemic disease, and each occurrence should be consulted to rule out more serious systemic disorders or blood clotting issues.
The diagnostic process starts with a thorough medical interview and an ophthalmic exam, where a specialist evaluates the extent and nature of the hemorrhage, checks visual acuity, movement of the eyes, and the presence of other, less visible changes. If the vessel break occurs often, or if there are symptoms suggesting systemic issues, the doctor may order laboratory tests, including blood count, clotting parameters, blood sugar, or blood pressure measurements. Occasionally, further imaging, such as ocular ultrasound or fluorescein angiography, is needed for precise assessment of vessel structure and patency. Treatment rarely requires medical intervention—most hemorrhages resolve by themselves within a few days to two weeks thanks to the body’s natural healing mechanisms. The main advice is to protect the eye from further trauma, discontinue contact lenses until healing is complete, and avoid rubbing and exposing the eyes to dust and chemicals. The ophthalmologist may recommend moisturizing drops for comfort, and sometimes, when appropriate, supplements such as vitamin C or rutin to support vessel regeneration. Underlying diseases or clotting disorders may require specialized therapy guided by an internist or hematologist. Proper, timely diagnostics solve not just the eye issue but help detect more dangerous conditions threatening patient health.
Prevention and prophylaxis of broken blood vessels in the eye
Preventing broken blood vessels in the eye relies primarily on removing or limiting risk factors, strengthening vessel walls, and adopting a healthy lifestyle that supports overall eye condition. The basis of prophylaxis is daily eye hygiene—do not rub your eyes, always wash hands before touching the eyes, and regularly wash your face, especially in dusty situations or while wearing contacts. Always follow contact lens hygiene rules and do not exceed usage times, to minimize irritation and microtrauma risk. For people spending hours at a computer, apply the 20/20/20 rule—every 20 minutes, look at something 20 feet away for 20 seconds. Proper eye hydration is maintained by ensuring air humidity indoors, avoiding cigarette smoke and air conditioning, and taking regular breaks during visually demanding tasks. Eyes should also be protected by sunglasses in summer (for UV protection and to reduce irritation from wind/dry conditions) as well as by using moisturizing drops, often called “artificial tears.” Supplementation with vitamins and minerals like vitamin C, K, rutin, bioflavonoids, zinc, and lutein supports blood vessel flexibility, reducing their fragility. Those predisposed to hemorrhages should add citrus fruits, parsley, black currants, spinach, cabbage, whole grain products, and legumes to their diet to supply essential nutrients for healthy circulation.
Regular medical checkups and treatment of chronic diseases that increase vessel breaking risk are also essential for prevention. Those with hypertension, diabetes, clotting disorders, or liver diseases should be under constant medical care and regularly monitor blood pressure and glucose, as any abnormalities directly impact the state of the body’s vessels, including the eyes. Cutting out stimulants like alcohol and cigarettes benefits vessel walls, as toxins and combustion products weaken vessels and increase their fragility. Regular physical activity boosts circulation and vessel flexibility, but avoid sudden heavy strain, such as lifting weights without preparation, as this can sharply increase intraocular pressure. People exposed to dust, chemicals, strong light, or other irritants should use eye protection such as safety goggles or masks. Stress-relief techniques also help—increased or chronic stress adversely affects circulation and may indirectly cause subconjunctival microbleeds. For seniors and children, regular eye health monitoring is crucial—watch for eye symptoms after intense crying or trauma in children and recommend more frequent ophthalmology visits for elderly people, especially with coexisting conditions. Any hemorrhage that appears for no clear reason, especially if repeated or accompanied by other complaints, should be consulted with a doctor to exclude more serious systemic conditions. Effective prevention thus encompasses a multi-pronged approach: from hygiene, diet, and supplements to regular medical control, reducing risk factors, and care for overall health.
Summary
Broken blood vessels in the eye are a common problem, usually not a sign of serious disease but possibly a signal of strain or other issues. It’s worth knowing the most frequent causes and accompanying symptoms to react effectively. In most cases, home remedies such as cold compresses and eye rest are enough. However, when concerning symptoms appear, professional diagnostics and an ophthalmologist consultation are necessary. Remember that proper prevention and eye care can significantly reduce the risk of future broken blood vessels.


