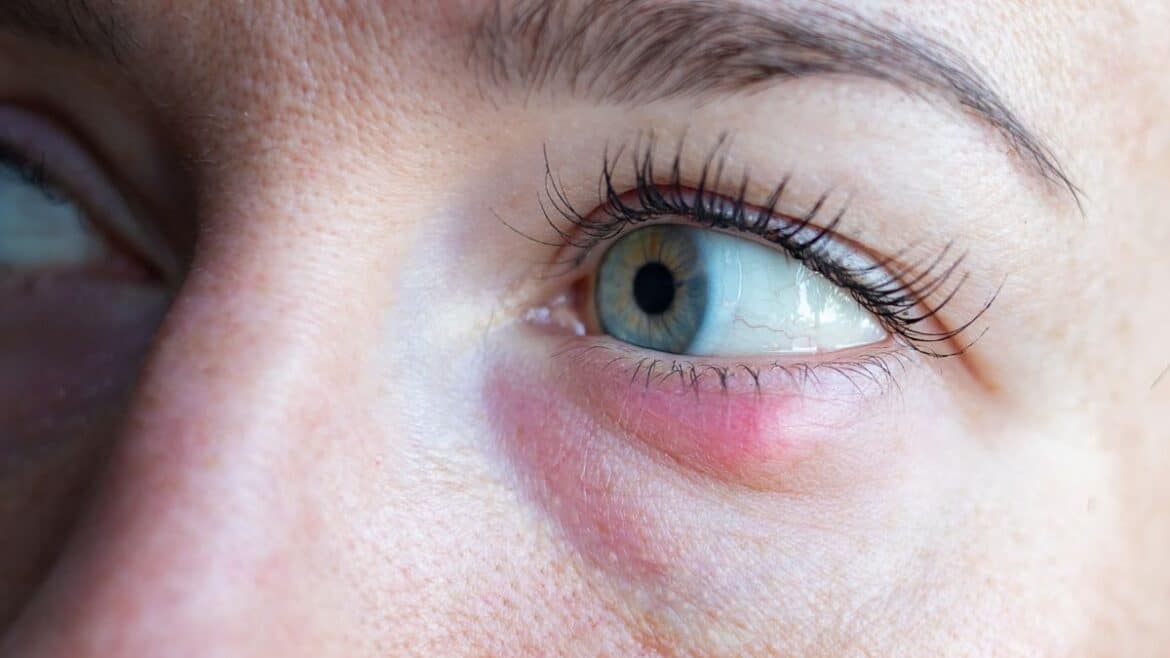
Learn how to recognize and effectively treat a stye. Learn about the causes, symptoms, home remedies, and preventative measures for your eye health.
Table of Contents
- What is a Stye? – Causes of Occurrence
- The Most Common Symptoms of a Stye
- How to Recognize a Stye – Diagnosis and Differentiation
- Treatment of a Stye – Home Remedies and Pharmacological Measures
- Possible Complications and Risks Associated with a Stye
- How to Prevent a Stye? Professional Prevention
What is a Stye? – Causes of Occurrence
A stye on the eye, also known as hordeolum, is a localized inflammatory condition of the eyelid, usually caused by bacterial infection. It typically appears as a painful, red bump located on the edge of the eyelid, sometimes filled with pus. Styes are divided into two types: external, which develops within the eyelash hair follicles or Zeis sebaceous glands, and internal, which arises in the Meibomian glands inside the eyelid. The vast majority of cases are caused by bacteria of the Staphylococcus aureus genus, which naturally exist on the skin, but can easily penetrate the glands and cause infection when the protective barrier of the skin or eyelids is breached. The main risk factors for developing a stye include poor hygiene, especially around the eyes, rubbing eyes with dirty hands, using expired or improperly stored makeup, and sharing towels or pillows. Additionally, people suffering from chronic eyelid conditions such as blepharitis or dry eye syndrome are at a higher risk for stye development due to more frequently disturbed gland protection and bacteria buildup in the eyelid area. Immune disorders and lowered immunity, e.g., during a cold, in diabetes, or in cases of chronic stress, also encourage the development of infection.
The initial stage of stye formation is blockage of the sebaceous gland duct or eyelash hair follicles. The secretion accumulating in the gland creates an ideal environment for bacteria to multiply, leading quickly to inflammation. As bacteria multiply, they release toxins and enzymes that intensify the inflammatory response, seen as painful redness, swelling, and sometimes a purulent discharge. Styes most commonly occur in those who touch their eyes without first washing their hands, especially children and people who lead active professional lives and are more exposed to contaminants. Additionally, wearing contact lenses and improper lens care, such as inserting lenses without disinfecting them or storing them in a contaminated case, also increases the risk of eyelid infections. Other encouraging factors include chronic inflammation, respiratory and food allergies, skin diseases such as rosacea or seborrheic dermatitis, and prolonged use of certain medications, such as glucocorticoids, which reduce local skin immunity. Note that a stye is not contagious in the traditional sense, but the bacteria responsible can be transferred by dirty hands or shared everyday objects. Thus, it is very important to follow basic hygiene rules, regularly wash your hands, and thoroughly remove makeup before sleep. Understanding these mechanisms and risk factors helps prevent the recurrence of styes, especially in people prone to such infections.
The Most Common Symptoms of a Stye
Although a stye is a relatively harmless condition, it can cause a variety of very unpleasant symptoms, impairing daily functioning and raising concern. The most characteristic and noticeable symptom is the appearance of a painful, red bump on the eyelid, typically along the lash line (in external stye) or on the inner eyelid (in internal stye). The lumps grow quickly, become tender to touch, and are distinctly separated from the rest of the eyelid. Usually, redness develops around the affected area, which can involve the entire eyelid. As the inflammation progresses, swelling may also occur, sometimes leading to partial or even complete closure of the eyelid. The swelling can be so pronounced that it makes normal vision difficult and causes a feeling of heaviness in the eye. Another typical, troublesome symptom is pain—ranging from mild discomfort to pronounced pulsation, worsening with blinking or touch. In advanced inflammation, the lump may accumulate pus. After a few days, a yellowish point may appear at the top of the lesion, which bursts on its own or under pressure, releasing pus. Relief from this symptom is usually associated with rapid improvement and reduction in pain.
Besides visible changes on the eyelid, a stye also causes general and subjective symptoms felt by the patient. Many people complain of itching, burning, or the constant sensation of a foreign body in the eye—patients often describe this discomfort as feeling like sand under the eyelid. Other possible symptoms include tearing, sensitivity to light, or blurred vision, due to eyelid swelling or the accumulation of secretions. In some cases, there is a general decline in well-being, especially if the inflammation extends to a larger portion of the eyelid or if there is a systemic infection (e.g., fever). A typical feature of a stye is that the lower or upper eyelid becomes hard, tight, and hot to the touch, and the patient may have trouble fully opening or closing the eye due to pain. The intensity of these symptoms varies depending on individual sensitivity and location of the stye; external styes usually cause more visible changes and faster abscess formation, while internal styes are harder to recognize and cause stronger pain when the eyeball is pressed. In rare cases, particularly in those with lowered immunity, a stye can lead to complications such as cellulitis (inflammation of the entire eyelid), spread of infection to surrounding orbital tissues, or even general health problems. It is essential to take the first signs of a stye seriously and carefully observe the development of symptoms, especially if they worsen or do not resolve within a few days.
How to Recognize a Stye – Diagnosis and Differentiation
Diagnosis of a stye is primarily based on its characteristic clinical presentation and the symptoms reported by the patient. A stye most often begins with localized pain, redness, and swelling of the eyelid margin, followed by the appearance of a distinct, painful bump in the area of the lashes or the Meibomian glands. Within several days the lump may grow and take on a yellowish tint, signaling the presence of pus and confirming the infectious nature of the change. On the surface of the stye, a pinpoint thickening or a small pustule is often seen, which may rupture and discharge pus after a few days, bringing symptom relief. Notably, the associated pain is usually pronounced, pulsating, and may make blinking or closing the eyelids uncomfortable. For most ophthalmologists, diagnosis can be established based on visual inspection and medical history, as symptoms are very typical. During an eye examination, the location is noted—for external stye, it is the eyelid margin near the lashes, while internal stye involves swelling deeper within the eyelid, often affecting its entire thickness. Slit-lamp examination enables precise visualization of inflamed glands, assessment of the depth of inflammation, and exclusion of potential complications, like the spread of infection into orbital tissues.
Differentiating a stye from other eyelid conditions is crucial, especially if treatment does not yield swift improvement or the lesion develops atypically. Most frequently, a stye should be distinguished from a chalazion, a chronic, painless lump resulting from obstruction and chronic inflammation of the Meibomian gland. A chalazion, in contrast to a stye, is usually bigger, hard, does not provoke acute pain or general symptoms such as extensive swelling or eyelid redness. The differential diagnosis also includes sebaceous gland cysts, warts, eyelid abscesses, and even eyelid tumors—especially in people over 50 or in cases of frequent recurrent suspicious lumps. The primary examination is careful visual inspection of the eyelid after everting it gently and evaluation of any discharge if present. In rare cases, microbiological examination (pus culture) is ordered, especially if atypical bacteria, antibiotic resistance, or recurrent infections occur in those with compromised immunity. In children, diabetic patients, or those with atopic dermatitis who experience frequent styes, assessment of the skin and mucous membranes of the eyelids and even dermatological consultation may be necessary. In diagnostic doubt, the doctor may consider imaging, such as eyelid ultrasound, to determine inflammation depth and extent. Quick and accurate diagnosis of a stye enables effective treatment implementation and reduces the risk of complications, especially the spread of infection to other ocular and facial structures.

Treatment of a Stye – Home Remedies and Pharmacological Measures
Treatment of a stye depends primarily on the severity of symptoms and type of the condition, but in most cases, the process can be started at home using safe and tested methods. The most commonly recommended first step is to use warm compresses—this is the simplest and most effective home remedy for speeding up the maturation and drainage of a stye. Heat improves blood supply to the eyelid, widens gland ducts, and accelerates the spontaneous rupture of the lump, enabling pus outflow. The compress should be applied several times daily (ideally 4-5 times per day), holding a clean gauze soaked in warm water or chamomile infusion over the closed eye for about 10-15 minutes. It is important not to squeeze the stye yourself, as this risks spreading the infection, worsening the inflammation, or causing infection of deeper eye structures and even an orbital abscess. Additional home support can include gentle eyelid massage toward the duct while the eye is closed, always maintaining high hygiene—hand washing is fundamental before any action near the eyes. In the early stages, before pus appears, herbal compresses (e.g., marigold or eyebright) may also be effective for their soothing and regenerating properties on eyelid skin. People wearing contact lenses should avoid them during infection and use glasses instead to minimize further irritation or bacterial spread. It is also crucial to avoid eye makeup and other cosmetic products near the eyes until the lesion is healed.
If, despite using home remedies, a stye does not improve after several days, symptoms intensify, or general signs such as fever, severe pain, or purulent discharge appear, it is worth using pharmacological measures—preferably after consulting an ophthalmologist. Pharmacologically, drops or ophthalmic ointments containing an antibiotic (e.g., gentamicin, neomycin, or erythromycin) are applied locally to fight the bacteria responsible and limit inflammation spread. In some cases, preparations with sulfonamides or other antiseptic agents are also recommended. These medications must be used as directed by a doctor, with proper hygiene. In cases where a stye is especially painful or resistant to topical treatment, or infection involves more of the eyelid or causes systemic symptoms, the doctor may initiate oral antibiotics. This is applied, in particular, to those with lowered immunity, diabetes, or recurrent infections. Sometimes, especially with internal or complicated styes, surgical intervention is needed, involving incision and drainage of pus, but this is a procedure performed only by an eye specialist. Artificial tears can be used to protect the eyes from further irritation and dryness, as well as agents that relieve swelling and itching. You should strictly avoid trying to pierce or squeeze the lump yourself, as this can spread the infection into deeper orbital tissues. Regular hygiene and compliance with medical instructions significantly shortens the duration of a stye and minimizes the risk of recurrence, and the proper choice of treatment methods—both home and pharmacological—enables a mild course and rapid recovery.
Possible Complications and Risks Associated with a Stye
A stye, though generally mild and self-limiting, can occasionally lead to complications requiring prompt medical intervention. The most frequent complication is the development of a chronic inflammatory state, resulting in the formation of a chalazion—a painless lump on the eyelid due to persistent pus in the Meibomian gland. A chalazion often requires surgical treatment, especially if it does not respond to ointments or warm compresses and begins to cause discomfort or vision disturbances. In more severe cases, if the stye is neglected or improperly treated, the infection may spread to neighboring eye structures such as the conjunctiva, eyeball, or eyelid skin. The infection can also spread via lymphatic or blood vessels, leading to eyelid felon or orbital cellulitis (cellulitis orbitae), manifesting as severe swelling, pain, fever, or even impaired eyeball movement. Such complications may require hospitalization and intensive intravenous antibiotics. Untreated or inadequately treated infections, particularly in those with reduced immunity, children, or the elderly, may lead to more serious health threats, such as an eyelid abscess (accumulation of pus in the soft tissues around the eye), which requires surgical incision and drainage. In rare instances, if the infection penetrates the orbit or bloodstream, it may result in sepsis (septicemia), a systemic infection that is life-threatening. Another rare, but possible, result of repeated or chronic infections is permanent damage to the eyelid glands, leading to chronic dry eye, discomfort, and a greater susceptibility to other infections and irritations.
Another significant risk associated with a stye is its impact on daily functioning and reduced quality of life. Even a single small stye can interfere with vision—due to eyelid drooping, swelling, and a foreign body sensation, it increases susceptibility to temporary visual acuity disturbances. For contact lens users, a stye can cause purulent corneal or conjunctival complications from bacterial transmission. Using makeup during infection further increases the risk of cosmetic contamination and re-infection, which, especially in women, can result in repeated ophthalmological problems and the necessity to replace all makeup tools. For chronic or recurring styes, further diagnostics should be performed for systemic diseases such as diabetes, atopic dermatitis, or immunosuppression, which predispose to frequent infections and complicate treatment. Improper handling of a stye—such as squeezing, scratching, or manipulating the lesion—can not only lead to secondary bacterial infections but also allow pus to penetrate the eyelid, increasing the risk of deep tissue infection. In extreme cases, improperly treated infection can negatively affect eyelid structure, causing deformation, scarring, and issues with proper closure—leading to persistent irritation, chronic tearing, or even impaired tear film function. Children and the elderly, whose immune systems are weaker, are especially at risk. In their cases, even a mild stye may spread infection more quickly and require faster ophthalmology consultation. Finally, recurring styes can signal both neglect of hygiene and underlying chronic or immune disorders, which require comprehensive diagnostics and management in order to prevent long-term health complications.
How to Prevent a Stye? Professional Prevention
To effectively prevent the appearance of styes, you should implement a series of daily hygiene and health habits that minimize the risk of eyelid infection. The most important element of prevention is systematic cleanliness of the eye area—especially for people prone to inflammation, allergy sufferers, and contact lens wearers. It is recommended to clean the eyelids daily with warm water or specialized eyelid hygiene products, which remove contaminants, makeup residue, and excess sebum. Avoid rubbing your eyes with dirty hands—always wash your hands before touching your face or eyes. Those who use contact lenses should strictly adhere to lens disinfection procedures and regularly replace lens cases to eliminate the risk of bacterial and fungal contact. Another important preventive aspect is avoiding sharing towels, pillows, cosmetics, or other items that touch the eye area—these actions limit germ transmission. Thorough removal of makeup before bedtime, and the selection of gentle, hypoallergenic eye products free from irritants and preservatives, is also critical. Taking care of makeup accessories, such as brushes and sponges, is another line of defense against bacterial buildup.
Attention should also be paid to general body condition—those who are weakened, fatigued, suffering from chronic diseases, diabetes, or immune disorders are much more vulnerable to eyelid infections. A diet rich in vitamins A, C, and E, and minerals such as zinc and selenium, supports immunity and proper ocular epithelium health. Regular physical activity, good sleep, and reduced stress positively affect natural defense mechanisms. People with recurring or chronic eyelid inflammation should consider regular ophthalmological check-ups and, when advised, use specialized shampoos or foams to clean eyelid margins. Responsible behavior also includes prompt response to the first signs of discomfort—you should not ignore redness, itching, or eyelid pain. Early intervention, such as warm compresses, can prevent inflammation from developing. It is also important to keep places where you spend a lot of time clean—regular laundering of bedding, changing pillowcases and towels, and disinfecting bathroom surfaces help maintain a bacteria-free environment. For those who work in dusty or irritating conditions, wearing safety glasses can protect the eyes from particles that might cause irritation and infection. Professional stye prevention is not only a set of daily hygiene rituals but also care for general health and awareness of alarming symptoms around the eyelids, as well as early medical consultation if they occur. By adopting a comprehensive approach and introducing healthy habits into daily life, you can effectively reduce the risk of styes and enjoy healthy eyes throughout the year.
Summary
A stye on the eye is a common problem, usually resulting from bacterial infection and inadequate hygiene. Prompt diagnosis, recognition of characteristic symptoms, and initiation of both home and pharmacological treatment allow effective resolution of this issue and minimize the risk of complications. Daily prevention—regular eye hygiene and avoiding risk factors—is also crucial. Remember that recurrent or persistent stye symptoms require ophthalmological consultation. Take care of your eye health using proven prevention methods.